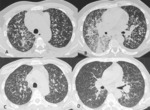
Typical radiologic findings include:
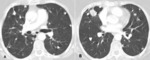
- multiple rounded nodules: the presence of multiple soft tissue nodules (hematogenous metastases) is the most common radiologic finding of pulmonary metastasis.
Nodules tend to be round or oval,
or they may have lobulated contours.
They usually have smooth and sharply defined margins,
however,
poorly defined or irregular.
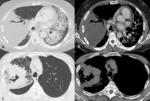
The size and number of nodules vary greatly from miliary metastases 1-4mm small,
numerous,
same sized nodules (Fig.
1 A,B),
to cannon- ball metastases (fewer,
large,
well defined masses); their distinction from nonmalignant pulmonary disease such as fungal infections (Fig.
1 B,C),
septic emboli,
tuberculosis,
Wegener granulomatosis or rheumatoid nodules may be difficult.
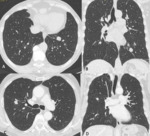
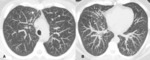
- Lymphangitic carcinomatosis: lymphangitic carcinomatosis refers to tumor growth in the pulmonary lymphatics.
It results from hematogenous spread to the lung,
with subsequent lymphatic invasion,
or from direct lymphatic spread of tumor from mediastinal and hilar lymph nodes.
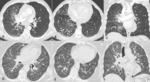
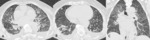
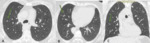
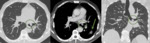
Lymphangitic carcinomatosis is characterized by smooth or nodular thickening of the axial interstitium (the peribronchovascular interstitium) and the peripheral interstitium (the interlobular septa and the subpleural interstitium) (Fig.2-3).
The findings of lymphangitic spread may be bilateral and diffuse however; in about 50% of patients the abnormalities appear focal,
unilateral or asymmetric hilar lymphadenopathy and pleural effusion may also be present.
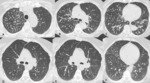
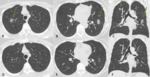
The clinical context is mandatory in making a differential from other conditions such as pulmonary edema or sarcoidosis (Fig.
4).
Atypical radiologic findings include:
- solitary mass/ solitary nodule:occasionally,
a metastatic tumor can be present as a solitary well or poorly defined solitary mass (more than 3 cm) that can be present cavitation or air-fluid level,
or solitary nodule.
The differential diagnosis of a solitary pulmonary nodule detected in a patient with known malignancy is a challenge and the definitive diagnosis may require biopsy.
It’s difficult differentiate from other pulmonary disease such asprimary lung carcinoma,
lymphoma or single metastatic nodules (Fig.5-6).
- cavitary nodules:a cavity is a gas-filled space within a pulmonary nodule,
a mass or a consolidation.
The cause of cavitation is presumed to be either tumor necrosis with the expulsion of the necrotic part of the lesion via the bronchial tree.
Chemotherapy is also known to induce cavitation.
The wall of a cavitated metastasis is usually thick and irregular (Fig.
7).
Differential diagnosis is infectious inflammatory diseases (Fig.
8),
Wegener granulomatosis and rheumatoid.
- calcified nodules:although calcification of a pulmonary nodule is usually suggestive of its benign nature,
it can also occur in metastatic nodules (Fig 9).
Mechanisms responsible for calcifications include bone formation (osteosarcoma,
chondrosarcoma),
dystrophic calcification (treated metastasis),
and mucoid calcification (mucinous adenocarcinoma of the gastrointestinal tract and breast).
Differential diagnosis is calcifications in infectious disease such varicella pox and other benign conditions (Fig.10).
- Endobronchial metastasis: endobronchial involvement occurs either by direct deposition of tumor cells to the bronchial wall by means of aspiration,
lymphatic spread,
or hematogenous spread or by local invasion of tumor from the adjacent lymph nodes or lung parenchyma into to the airway wall.
The form of development of endobronchial metastases are defined in four type as follows: type I,
direct metastasis to the bronchus (Fig.
11); type II,
endobronchial invasion of parenchimal secondary mass; type III,
endobronchial invasion of secondary mediastinal or hilar lymphadenopathy; type IV,
extention of a peripheral metastatic parenchymal lesion along proximal bronchus.
At imaging,
a tapered narrowing of the airway lumen,
or sessile or polypoid endobronchial mass may be observed.
Atelectasis may be present as a consequence of airway obstruction.