A recent International Atomic Energy Agency Integrated Regulatory Review Service (IAEA-IRRS) mission to assess the regulatory framework for nuclear and radiation safety in Ireland, concluded that Ireland benefits from an effective and independent radiation safety regulatory body and made several recommendations to further strengthen Ireland’s regulatory safety framework [3].
These included:
- An effective legal framework for the regulation of patient protection should be implemented,
and arrangements to inspect and enforce measures to ensure patient protection should be put in place.
- The regulatory body responsible for patient protection should be independent and not have responsibilities for or interests in providing medical radiation treatments,
and all regulatory bodies in this area should coordinate their work effectively
Structure of radiation protection in Ireland (Fig.
3)
Health Service Executive (HSE)
The HSE is the public body responsible for the provision of health and personal social services for everyone living in Ireland.
The Medical Exposure Radiation Unit (MERU) of the HSE,
was established to fulfil the regulatory functions assigned to the CEO,
HSE in Irish Legislation Statutory Instrument 478,
2002 which gave effect to the Council Directive 97/43/Euratom.
MERU
The role of the MERU,
HSE is to regulate patient radiation protection practices in radiological facilities and receive advice from the National Radiation Safety Committee (NRSC).
The MERU is tasked with:
· Conducting/overseeing clinical audit in facilities using medical ionising radiation.
· Managing the mandatory incident reporting system.
· Providing guidance on relevant matters as guided by the NRSC
· Ensuring quality assurance programmes are in place.
· Maintaining a register of installations.
· Supporting and managing the work of the NRSC and its subcommittees.
NRSC
The NRSC was established in 2007 and is tasked with providing expert advice to the HSE on the medical use of ionising radiation.
The NRSC recommended in 2010 that all radiological installations keep a Radiation Protection Manual [4] on site.
The responsibilities of the NRSC include to:
· Provide advice to the HSE and the Minister for Health to protect patients from the harmful effects of ionising radiation.
· Receive reports of clinical audits,
incidents and inspections.
· Gather lifetime data on equipment and an assurance that each piece of equipment is recorded as being maintained.
· Monitor DRLs.
Environmental Protection Agency (EPA)
The EPA is the designated competent authority responsible for regulating the use of ionising radiation in Ireland.
This function was formerly under the remit of the Radiological Protection Institute of Ireland (RPII).
This is achieved through a system of licensing and inspection,
which is designed to ensure that the risk to workers and members of the public from ionising radiation is kept to a minimum.
The EPA’s Office of Radiological Protection (EPA-ORP) regulates and licences almost 1700 practices in Ireland,
including hospitals,
dentists,
veterinary surgeons,
universities,
institutes of technology and industrial users.
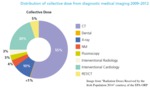
In 2014 the RPII (now EPA-ORP) published the most up to date assessment of radiation dose received by the Irish population from both natural and manmade sources [5] (Fig.
4).
Faculty of Radiologists Radiation Protection Committee (FRRPC)
The Faculty of Radiologists is primarily responsible for postgraduate training programmes and examinations in radiology in Ireland.
The role of the FRRPC is to ensure that the faculty is aware of all relevant current and future radiation protection issues,
to make representations on radiation protection issues on behalf of the faculty and to address any radiation protection issues sent to the faculty for its consideration or opinion.
The FRRPC liaises with the NRSC,
MERU,
EPA and ESR to meet its objectives.
EuroSafe Action 2 – Clinical Audit
In 2014/15 the HSE Quality Assurance and Verification Division (QAVD) performed an audit across a number of individual radiology units in Ireland entitled “Audit of patient pregnancy protocols and diagnostic reference levels as outlined in the Medical Exposure Radiation Unit’s (MERU) Patient Radiation Protection Manual” [6].
This audit resulted in a number of recommendations to ensure compliance of all facilities using medical ionising radiation with national and European legislation including:
· To establish a Radiological Clinical Audit Working Group to ensure that local clinical audit is carried out systematically and regularly reviewed by the radiation safety committee.
· To develop a local written policy on the management of DRLs
· To implement a radiation protection training schedule to include the following: patient radiation protection training; DRLs training; and to utilise current systems to record training in a systematic way.
The Irish Medical Council requires that all doctors in Ireland maintain their professional competence,
which includes the completion of at least one clinical audit per year [7].
Clinical audit,
with an emphasis on radiation protection,
is facilitated by the Faculty of Radiologists in the national radiology training programme and each radiology trainee receives dedicated training in performing clinical audit.
The HSE,
in conjunction with the faculty,
offer an annual clinical audit prize for trainees sponsored by the NRSC and the HSE.
The aim of the prize is to promote participation in clinical audit among trainees and consultants and to highlight innovative practice.
EuroSafe Action 3 – DRLs
Since 2008,
the HSE has been collecting statistics on population dose levels from the use of medical ionising radiation.
These data have been used by the Population Dose and Optimisation Subcommittee of the NRSC to update the national Diagnostic Reference Levels (DRLs) in Ireland (Fig.
5).
Previous DRLs used in Ireland relied heavily on data collected from UK and European sources,
whereas the most up to date set of DRLs (2014) are based on data from Irish hospitals.
Our national DRLs are used to benchmark local practice and local DRLs are recommended as the first step in the optimisation of procedures,
as they are most relevant to the patient cohort,
examination type and equipment available locally.
Service providers are required to establish and use DRLs for each of their routine procedures.
DRLs should be reviewed annually,
when there is a significant change in protocol or where they are consistently exceeded.
One of the advantages of the 2011 introduction and subsequent rollout of the National Integrated Medical Imaging System (NIMIS) in Ireland has been the provision of centralized data collection software (Radimetrics,
Bayer HealthCare) that can be used for the purposes of dose tracking and optimisation.
Some hospitals have alternative radiation dose tracking systems in place,
for example DoseWatch (General Electric) used in Cork University Hospital (CUH).
At CUH,
a multidisciplinary CT/IR dose-team has been created which has worked to validate automated measurement of size specific dose estimates [8] ,
assessed the accuracy of patient centering for CT [9] ,
calculated local DRLs and assessed factors which influence patient radiation exposure at CT [10].
It was recommended by the HSE in 2014 that all hospitals with CT,
interventional radiology or those performing paediatric exposures should implement the use of dose tracking and alert solutions within the following 3 years.
The use of dose-tracking software has been encouraged by the FRRPC and the allocation of medical physics resources to this task has been proposed.
National standardisation of CT protocols is another key strategic theme of the FRRPC and NRSC; this is important for quality control and accurate DRL calculation.
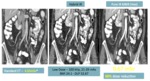
This will also provide a means of sharing and benefitting from experience gained in different institutions which are connected with NIMIS e.g.
sharing of low-dose CT protocols that have been validated [11] (Fig.
6).
EuroSafe Action 6 – Education and training in medical radiation protection
Radiation protection training is a central role of the Faculty of Radiologists.
Medical students and doctors are required to undertake radiation protection training and medical student knowledge regarding radiation protection has been shown to be improved by radiation protection education in Ireland [12].
Radiation Protection training forms a core part of the radiology training programme in Ireland.
This currently comprises a lecture series specifically focused on radiation protection as well as a training module in clinical audit.
The faculty is currently reviewing the curriculum for the basic training portion of the programme and plans are being formulated to introduce competency-based assessment with one component anticipated to include a project based around radiation protection and dose optimisation. The faculty also has strong input from radiation oncology.
The radiation oncologists,
who also sit on the NRSC,
in association with the School of Therapeutic Radiography in Trinity College Dublin have been involved in training on incident reporting and analysis,
radiotherapy during pregnancy and radiation audits. In order to comply with Irish legislation,
the medical council mandate that all non-radiology doctors that utilize ionising radiation (e.g.
cardiologists and vascular surgeons) undertake a radiation protection course prior to any use of ionising radiation in their practice.
To assist with compliance,
an online radiation training programme is envisaged.
The University College Dublin (UCD) School of Radiography have undertaken large amounts of work in the area of radiation protection,
and particularly in dose optimization in CT.
UCD offer an online course entitled “Computed Tomography: Safe CT”,
which details essential dose optimisation techniques so that users are more conscious of radiation protection within the modality [13].
UCD also provide two additional fully online radiation protection modules,
one a compulsory module for the UCD medicine graduates,
aimed at ensuring all graduates have core knowledge,
skills and competencies of radiation protection topics,
especially related to their roles as referrers; this aligns with the European Commission’s RP175 guideline [14].
The second is a Professional Certificate in Radiation Safety [15] which is offered to all professionals working with ionising radiation; this aims to introduce radiation workers to the principles of radiation safety and the application of these principles in the safe use of radiation sources in their profession.
It also provides the necessary tools for those who will become trainers in radiation protection.