Triggered by the 50% implementation rate we tried to find potential obstacles for implementing DRLs in general and especially in children.
To that end we scrutinized relevant inventories executed by the  National Instiute for Public Health and the Environment (RIVM) in the last 10 years.
National Instiute for Public Health and the Environment (RIVM) in the last 10 years.
RIVM reports
The RIVM conducts scientific research on behalf of government policy and the oversight exercised in the area of public health,
the environment and nature.
The institute is an independent branch of the Ministry of Health,
Welfare and Sport (VWS).
It also conducts research for the Ministry of Infrastructure and the Environment (I&M) and the Ministry of Economic Affairs,
Agriculture and Innovation (EL&I). The last 50 years the RIVM published several reports about different aspects of radiation protection,
mostly at the request of the  Health Care Inspectorate.
Health Care Inspectorate.
perceived problems
In two of the last published reports2,3 (published after the introduction of DRLs in the Netherlands) mention was made of following problems:
- The evaluation of DRLs in children is more complicated than in adults,
because the values are much more influenced by patients weight.
- On a local level it is sometimes impossible to find enough patients of a certain age category to define local exposure level.
- The methods used are highly variable between institutions (and often wrong).
These problems are not specific for the Dutch situation and they allready have led the ESR to establish the European DRL project in Paediatric Radiology (PiDRL).
The specific objectives of the PiDRL-project are to
- agree on a methodology for establishing and using DRLs for paediatric imaging
- update and extend the European DRLs to cover more procedures and a wider patient age/weight range based on current knowledge.
However in a report on the quality of radiology departments we found two more "cultural" factors that can be of influence in adopting DRLs: the availability of written protocols and the participation of the medical physicist in optimization of protocols.
written protocols.
When dose levels are structurally to high one should investigate the cause(s).
One important reason can be ad hoc or systematically too extensive protocols.
Without a written protocol this is hard to recover.
In a report about the quality of radiology departments4 in 2010 about 90% of general hospitals had dedicated protocols for ct in children and lower numbers for other body parts.
For fluoroscopy the numbers were remarkably lower (67%).
In a more recent survey this number wasn't much better (see table 1).
| |
general hospital |
academic (pediatric) hospital |
| ct |
|
|
| head |
18/20 (90%) |
7/7 (100%) |
| abdomen |
15/20 (75%) |
7/7 (100%) |
| chest |
14/20 (70%) |
7/7 (100%) |
| vertebral column |
12/20 (60%) |
7/7 (100%) |
| neck |
10/20 (50%) |
7/7 (100%) |
| pelvis |
10/20 (50%) |
6/7 (86%) |
| fluoroscopy |
|
|
| micturition cystography |
17/20 (85%) |
7/7 (100%) |
| esophagus/stomach |
13/20 (65%) |
7/7 (100%) |
| large intestine |
13/20 (65%) |
7/7 (100%) |
| small intestine |
9/20 (45%) |
7/7 (100%) |
| |
|
|
table 1: availability of written protocols.
There was a striking difference between general and academic hospitals: the scores for all academic hospitals were nearly 100%.
From the reports it's not quit clear what's the reason for this difference,
but one possible explanation is the fact that certain types of examination aren't executed in the hospital.
The legislator of Euratom problably also felt the need for written protocols because "Written protocols for every type of standard medical radiological procedure are established for each equipment forGenral relevant categories of patients" (BSS:Article 58.a).
influence of medical physicist
An interesting finding concerning (written) protocols is that in the inventory of 20142 it became clear that in case of revision of scan protocols in 25/27 participating hospitals a radiologist was involved,
in 21/27 a technician and only in 10/27 a medical physicist.
Obviously the protocol was looked upon as the responsability of the radiologist and/or technician and only in a minority of hospitals also the medical physicist had a role.
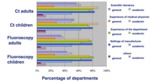
In figure 1 similar results are presented from the report of 2010: General departments trust their own experience,
the settings of the manufacturer and to a lower extent the scientific literature.
Th academic centers also trust their own experience,
the settings of the manufacturer and scientific littarature,
but also have high confidence in their medical physicist,
especially in ct (>80%).
And here again the legislator of BSS had a forsighted vision and state that "The practitioner,
the medical physics expert and those entitled to carry out practical aspects of medical radiological procedures are involved,
as specified by Member States,
in the optimization process" (Article 57.1b).