Congress:
EuroSafe Imaging 2017
Keywords:
Breast, Action 8 - Radiation protection training and learning material, Action 11 - Dialogue with industry, Action 3 - Image quality assessment based on clinical indications, Action 6 - Education and training in medical radiation protection, Action 5 - Exchange and collaboration with medical industry, Action 4 - Quality of radiological equipment, Mammography, Equipment, Cancer
DOI:
10.1594/esi2017/ESI-0036
Description of activity and work performed
Since the introduction of mammography,
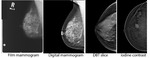
many incremental technological innovations have made it possible to obtain mammograms with higher image quality using significantly lower radiation dose as compared to mammograms conducted in in the 1970’s and early 1980’s (figure 2).
Some significant innovations and milestones:
- 1969 Dedicated mammographic unit with molybdenum target tube and compression cone replacing conventional tungsten target x-ray tubes with direct exposure industrial type films (figure 3)
- 1972 Screen-film system introduced for mammography reduce the dose 10 to 20 times
- 1976 Rare earth screen-film system and special cassette reduce the dose by 50%
- 1976 Mammography x-ray unit for magnification with microfocal spot
- 1978 Mammography unit with grid
- 1990 Fully automatic adjustment of technique factors (anode track,
filter,
kV,
mAs)
- 1999 Introduction of first Digital mammography system
- 2008 Breast tomosynthesis system CE mark
- 2010 Contrast–Enhanced Spectral Mammography system CE marked
More recent developments have seen the introduction of innovative technologies in the field of dose optimization and clinical efficacy and are available on all/most of the new equipment place on the EU market:
- Automatic exposure controls that deliver optimal dose over a wide range of breast sizes and compositions
- Breast tomosynthesis options that improve clinical performance
Historical Performance Metrics
The evolution of mammography systems has provided both systematic reductions in radiation dose and improvements in image quality.
Figure 4 illustrates the trends in mammography dose and image quality for the period from 1974-2014 as provided by the US FDA1. More recent data from 2012,
also from the US FDA,
lists the average digital mammography dose in the US to be 1.43 mGy,
showing around a 28% reduction from the approximately 2 mGy levels in 20052.
And even more recently,
clinical trial data on breast tomosynthesis indicate a significant improvement in cancer detection,
using systems that perform tomosynthesis scans at similar doses to 2D mammography.
Training
Advances in technologies have clearly transformed breast screening since its introduction; however the role of education and training is also an extremely important tool in the process of dose optimization.
While COCIR Members accept responsibility for maintaining the proper competence levels of their own staff and trainers,
it is the healthcare providers’ responsibility,
to assess and maintain their equipment,
their own staffs’ competency and to liaise with the relevant manufacturers for their training requirements as well as to enable their staff to participate to training and education.
Manufacturers propose/offer specific training programs on existing and new dose reduction techniques and on the use of these product features in daily practice.
The provision of specific training curricula aim to ensure that the user is well trained on dose optimisation and facilitates dose awareness in daily practice.
Manufacturer’s training is designed to support customer facilities in an effort to improve operating knowledge and increase the skill level of personnel.
These programs consist of a variety of delivery mechanisms such as:
- Hands-on and didactic training to reinforce skills needed to operate equipment
- Operator Manuals to demonstrate information on dose optimisation tools and dose reduction strategies
- Information on dose related displays,
indices,
and where dose information is located
- Onsite training,
classroom instruction,
remote instructor-led training and observation,
online tutorial self-help,
telephone support,
publications,
seminars,
peer to peer physician training,
and industry association educational material.