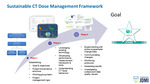
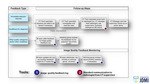
An iterative four phase protocol change management approach was used for the CT dose committee to achieve the goals - identify,
plan,
execute and monitor (Figure 1,2).
In the identification phase,
a CT dose tracker tool (Radimetrics,
Bayer) was leveraged to identify the most frequently used protocols,
mapped out by scanner and location,
and to detect of opportunities for dose reduction.
With an array of various dose metrics,
the dose length product (DLP) was selected as the best metric to track dosage for this committee [4].
At weekly working groups comprised of clinical,
leadership and project management staff,
the members confirmed the selected protocols and parameter changes based on the lead radiologist’s expertise in consultation with other Division heads and clinical physician leads.
In the planning phase,
approval was first sought out from the respective imaging Division head for the parameter changes.
Protocol parameter changes included any of the following: target image noise standard deviation,
helical pitch,
tube voltage (kV),
tube current (mA),
tube rotation time (s),
number of perfusion phases,
anatomical coverage,
contrast material injection protocol,
reconstruction parameters and storage.
Following this approval,
the committee finalized logistics for executing the protocol parameter changes at each scanner and developing the communication to all CT technologists who might become impacted by the changes.
In the execution phase,
the protocol parameter changes were updated in the scanners for the specific protocol and trialed for one week at one hospital site.
During this week,
radiologists evaluated the image quality for all the scans reported for the updated protocol.
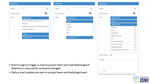
This feedback was collected via an in-house developed web-based tool for image quality assessment (Figure 3).
This tool not only served to flag the committee when a particular parameter change was affecting image quality promptly (i.e.
images produced were deemed non-diagnostic),
but it also allowed the radiologists to rate image quality and artefacts,
and provided the related reason as to why the quality of the image was not adequate (such as field of view,
contrast material,
positioning,
etc.).
After the one week trial and if no negative feedback was received from radiologists or technologists,
then changes were applied to the remaining hospital sites.
Nevertheless,
feedback was always welcomed from all radiologists along with any technical feedback.
In the monitoring phase,
the CT dose committee reviewed the dose levels outcomes on a weekly basis that covered analyzing the impact on DLP levels and investigating outliers.
In addition,
radiologist feedback via the image quality assessment tool was reviewed; any image quality feedback (quality too poor or too good) triggered an evaluation of the parameter changes via CT dose committee discussion.
After all the changes have been implemented and clinically operationalized and to create a framework for sustainability,
the CT image feedback tool remained active and serves as an ongoing sensor for any unexpected variation or deviation (Figure 4).
The feedback tool is integrated into JDMI’s PACS and readily available to all reporting radiologists.
One of the key features of the tool is the differentiation of feedback that might require immediate action from basic feedback on non-urgent quality variations.
The purpose of the “action required” flag is to potentially rectify reconstruction issues so long as the raw data exist on the CT scanner,
or to act quickly if calibration or any other immediate technical intervention is deemed necessary.
Data from the feedback tool are collated on an ongoing basis and discussed at the following monthly CT dose committee meeting (Figure 5).