Congress:
EuroSafe Imaging 2021
Keywords:
Radioprotection / Radiation dose, CT, Radiation safety, Quality assurance
Authors:
M. R. Onur, Y. BAYTAR, S. Ardali Düzgün, M. N. Özmen, D. Akata
DOI:
10.26044/esi2021/ESI-15279
Results or findings
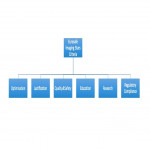
Eurosafe Imaging Stars criteria consist of 21 criteria that are classified into six main topics (Fig. 1).
I. Optimization criteria
- CT protocols
- Overview: CT protocols and their acquisition parameters should be easily accessible.
- Challenge: CT protocols in radiology departments with multiple different vendor CT scanners may differ due to protocol titles and acquisition parameters of CT scanners.
- Recommendation: Acquisition parameters of CT studies should not vary in a wide range between CT scanners. CT protocol names should also be matched with commonly used lexicon codes such as RADLEX and LOINC.
2. CT dose management system (DMS)
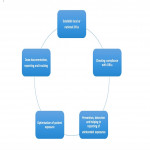
- Overview: This criterion necessitates the presence of a DMS in radiology departments (Fig. 2).
- Challenge: DMSs may differ according to their capability for receiving radiation dose parameter information from CT scanners and/or Picture Archiving and Communication System (PACS).
- Recommendation: Appropriate retrieving data from different CT scanners can be accomplished with the achievement of matching different terms of different CT scanners that represent the same CT parameter.
3. Use of local diagnostic reference levels (DRL) for CT
- Overview: DRLs refers to a specified radiation dose level at which an investigation of the high dose levels may be initiated.
- Challenge: Misregistration of CT examinations into wrong CT protocols may cause errors in the determination of DRLs.
- Recommendation: DMSs should have software that detects CT examination-protocol matching errors.
4. Data collection for clinical indication-based DRLs
- Overview: DRL is one of the most helpful quantitative parameters in radiation safety that allows benchmarking in a radiology department.
- Challenge: Radiology departments may only provide DRLs of anatomically classified CT examinations.
- Recommendation: Collaboration between dose management software and hospital information system and PACS may be helpful to subgroup anatomically classified CT examinations according to clinical indications.
5. Specific pediatric CT protocols
- Overview: This criterion emphasizes the necessity and easy accessibility of pediatric CT protocols in radiology departments.
- Challenge: Specific CT protocols for pediatric patients need to be adjusted according to body size, weight, and age because children are more heterogeneous in that way.
- Recommendation: Specific CT protocols for the pediatric age groups with facilities of high pitch, organ-based radiation dose reduction, etc., should be present in the equipment.
6. Specific fluoroscopy protocols for dose reduction in children
- Overview: Fluoroscopy is a more frequently used imaging technique in children compared to adults deserves to be included in radiation safety policy.
- Challenge: Protocol optimization and acquisition parameters in fluoroscopy are less pronounced compared to CT that causes less awareness in radiologists about dose optimization in fluoroscopy.
- Recommendation: Fluoroscopy equipment should have specific pediatric protocols.
7. Image quality assessment program in place
- Overview: Image quality assessment programs aim to preserve image quality whilst keeping radiation dose to the patient as low as is reasonably possible.
- Challenge: Establishment of an appropriate image quality assessment program in the department.
- Recommendation: Image quality assessment programs may depend on qualitative and quantitative analysis of CT images with standardized, indication-specific criteria [1].
II. Justification
8. Process for evaluating cross-sectional imaging requests
- Overview: Radiation safety policy begins with the assessment of a cross-sectional imaging referral in terms of appropriateness criteria.
- Challenge: Relevant clinical information and expectations from the requested exam should be provided by the referrer.
- Recommendation: A scoring system may be used in the evaluation of the imaging request which includes the patient’s age, gender, body habitus, past imaging history, and risk of contrast nephropathy.
9. Local policy for identification of referrer
- Overview: Identification of referring physicians is important for discussing the appropriateness of prescribed imaging, clarify the clinical question, and plan the CT protocol.
- Challenge: Difficulties in the identification of a referrer physician might result in the postponement of scan or repeat exams.
- Recommendation: A referring physician and contact info column should be added to the electronic referring system.
- Imaging referral guidelines
- Overview: Imaging referral guidelines are developed in order to justify the requested exam with evidence-based algorithms.
- Challenge: Imaging referral guidelines may not be used practically due to the discrepancy between guidelines and the regulations of national healthcare programs.
- Recommendation: National imaging referral guidelines should be prepared in accordance with national healthcare regulations that support the referring practitioner in selecting and justifying radiological procedures.
11. Operational CDS in clinical practice
- Overview: CDSs quickly determine if a patient meets the appropriateness criteria for a requested exam.
- Challenge: Clinicians may view CDS as technology telling doctors how to practice medicine, cost of the software and, the update of the system according to current practice guidelines.
- Recommendation: A user-friendly, flexible and, evidence-based CDS system in accordance with local needs should be preferred.
- Local justification policy for women of child-bearing age
- Overview: Women of child-bearing age are potentially more vulnerable to risks of radiation.
- Challenge: Common imaging referral guidelines and CDS may not be appropriate in imaging referrals of this patient group.
- Recommendation: A proper justification criterion for imaging referrals in women of child-bearing age should be implemented in CDS.
III. Quality and Safety
13. Clear radiation protection tasks for radiographers
- Overview: Increasing utility of X-ray based exams necessitates awareness and support of radiographers to establish a dose reduction program.
- Challenge: Radiographers may not be interested in dose reduction strategies.
- Recommendation: Predefined checklists for radiographers and periodic performance evaluation program with a feed-back mechanism can improve the collaboration.
- Patient information on radiation issues
- Overview: Patients and/or caregivers should be informed about the procedure, possible risks of ionizing radiation and, benefits of the exam.
- Challenge: Disinformation about the X-ray used imaging examinations is not uncommon in internet sources that should be dealt with.
- Recommendation: Patient information should be provided in easily accessible internet portals and/or hard copies. Pediatric patients and women of childbearing age should especially be addressed.
15. Regular equipment quality control
-
- Overview: The performance of CT scanners should not be below the standard in order to ensure patient safety and image quality.
- Challenge: Quality controls of imaging equipment are usually performed by the vendors.
- Recommendation: Quality controls of imaging equipment should be performed at least annually and by independent experts.
- Access to medical physicist’s expertise
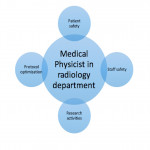
- Overview: The tasks of a medical physicist in a radiology department consist of patient care, teaching and, research activities in radiation safety (Fig. 3).
- Challenge: Medical physicists may not be familiar with X-ray and CT physics.
- Recommendation: A medical physicist that completed the core curriculum determined by EFOMP or ESP should be employed.
17. Operational clinical audit program including radiation protection
- Overview: Clinical audits regarding radiation safety are helpful for the quality assessment in the daily practice of dose reduction strategies.
- Challenge: To develop a program of effective clinical audits in the department regarding radiation dose optimization.
- Recommendation: ESR has introduced a guide tool named Esperanto for developing clinical audits in radiology departments.
18. Operational benchmarking program
- Overview: Benchmarking programs enable radiology departments to compare radiation dose levels of CT protocols as well as CT scanners and CT technologists for each protocol.
- Challenge: CT scanners might result in notable dose differences.
- Recommendation: CT scanners of the same vendor may be included in benchmarking between radiology departments.
IV. Education
19. Educational program in radiation protection
- Overview: New scanners, emerging technologies, and techniques necessitate an ongoing education program dedicated to enhancing the competence of staff.
- Challenge: Inexperienced staff members and/or those identified to not fully comply with requirements of the department might be in need of a more intense and focused program.
- Recommendation: Education program arranged to expand the theoretical comprehension and practical expertise of staff along with the promotion of a safety culture is crucial.
V. Research
20. Radiation protection research activities
- Overview: Research activities in radiology departments may be helpful in the improvement of radiation safety strategies by contributing to the findings of the research which may depict the presence and causes of deficiencies of the policies.
- Challenge: Research activities in radiation safety need to be performed with the collaboration of the radiation safety team in the department.
- Recommendation: Dose management systems provide enormous data for research activities including dose levels and underlying causes of an excessive dose.
VI. Regulatory compliance
21. Local implementation program for Basic Safety Standards (BSS) Directive (2013/59/EURATOM)
- Overview: European Council Basic Safety and Standards Directive (BSSD), 2013/59/Euratom brings about a core radiation protection standard for departments.
- Challenge: Many departments fail to meet the terms of this directive especially those related to justification and to support clinical audit structure.
- Recommendation: Dedication for improved patient safety, cooperation with European agencies, national bodies and, governmental institutions would be beneficial.