Purpose or learning objective
Purpose:
The purpose of this quality improvement project (QIP) was to assess awareness of the relative radiation risk of commonly ordered radiological investigations as a means of determining whether medical staff are appropriately justifying imaging requests at the Royal London Hospital, United Kingdom.
Methods or background
Background:
Investigations involving ionising radiation are integral to almost every patient's pathway through hospital. Although the risk is small, in the United Kingdom (UK) an estimated 100-250 deaths occur each year from cancers directly related to medical exposure to radiation [1]. On top of this, the quantity of investigations being carried out is rising exponentially - in the year 2018 5.15 million CT scan were performed in the UK [2].
National public bodies, such as the General Medical Council (GMC), and national legislation, such as...
Results or findings
Results:
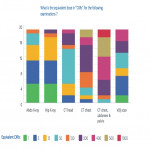
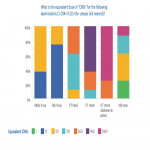
1. What is the approximate equivalent dose in “CXRs” for the following examinations ? (one CXR= 0.02 mSv)
[Fig 6]
[Fig 2]
[Fig 4]
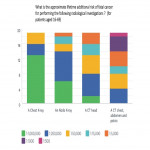
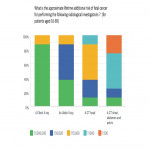
2. What is the approximate lifetime additional risk of fatal cancer for performing the following radiological investigations?
[Fig 7]
[Fig 3]
[Fig 5]
Limitations/ points of discussion:
Small study numbers.
There are constantly evolving radiation reducing imaging technologies and techniques.
Individual doses are heavily dependent on patient age, sex, weight etc.
Retrospective studies looking at cancer risk require follow up...
Conclusion
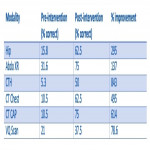
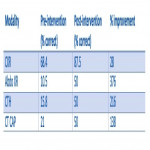
This small quality improvement project highlighted the poor baseline knowledge of radiation risk amongst clinicians of ranging grades within the acute medical department of a large London teaching hospital.
Although our initial target of '100% knowledge' was by no means met, this QIP clearly demonstrates that simple interventions, such as departmental ”grand rounds” and informative posters, are important and effective ways to help inform clinical colleagues on the relative radiation risk to their patients. This, in turn, will undoubtedly improve patient care and patient safety....
References
[1] Royal College of Radiologists and National Radiological Protection Board. Patient dose reduction in diagnostic radiology.Documents of the National Radiological Protection Board1990;1:No 3.
[2] Diagnostic Imaging Dataset Annual Statistical Release 2017/18
https://www.england.nhs.uk/statistics/wp-content/uploads/sites/2/2018/11/Annual-Statistical-Release-2017-18-PDF-1.6MB-1.pdf
[3] Good Medical Practice, The duties of a doctor registered with the GMC
https://www.gmc-uk.org/ethical-guidance/ethical-guidance-for-doctors/good-medical-practice
[4]The Ionising Radiation (Medical Exposure) Regulations 2017 https://www.legislation.gov.uk/uksi/2017/1322/contents/made
[5] Mettler F, Huda W, Yoshizumi T, Mahesh M. Effective doses in radiology and diagnostic nuclear medicine: a catalog. Radiology. 2008;248:254–263
[6] Lin, Eugene C. “Radiation risk from medical imaging.” Mayo...
Personal information and conflict of interest
T. Lopez Bernal:
Nothing to disclose