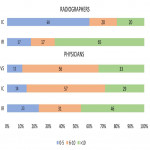
The questionnaire was answered by 80 professionals from four university hospitals, 51% of them were physicians and 49% radiographers. 82% of radiographers were involved in interventional radiology procedures and 18% in interventional cardiology procedures, while 45% of physicians were involved in interventional radiology procedures, 24% in interventional cardiology procedures and 31% were vascular surgeons. Distribution of surveyees regarding years of experience as a member of the interventional team is given in Figure 1.
51% of surveyees were acquainted with equivalent dose limit for the lens of the eye, 35% with equivalent dose limit for the extremities and 30% of them were aware of dose threshold for deterministic effects of the lens of the eye. 71% of surveyees confirmed that they wear their dosimeter regularly and 29% of them were aware of their annual effective dose.
Great majority of surveyees (89%) was aware that wearing ill-fitting protective garments can result in insufficient protection. Protective glasses were used by 33% of surveyees; among physicians who are always in the interventional suite during the procedure, only 38% of them use protective glasses.
40% of surveyees were aware that use of protective gloves when hands are in the primary beam may cause increase of operator's exposure and 37% that use of disposable protective patient drapes placed on the patient in a way that they are partially in the primary beam may increase operator's exposure.
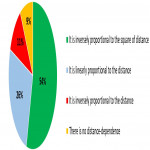
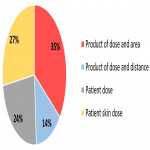
Distribution of answers regarding the change of dose with the distance is shown in Figure 2 and regarding the definition of dose-are product (DAP) in Figure 3.
91% of surveyees were aware that greater thickness of the patient will result in higher operator's dose and 70% that operators are exposed mainly to radiation scattered from the patient. Only 28% of surveyees knew that during lateral projections standing on the detector side will deliver lower dose to the operator, 67% chose to stand on the tube side and 5% didn’t know which side to choose in order to decrease their dose.
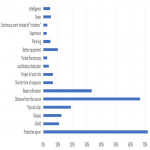
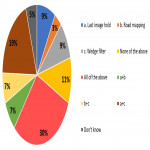
Surveyees were asked to identify ways of protection they consider as the most effective. Distribution of answers to that question is given in Figure 4.
With the fact that dose rate is greater in cine mode than in fluoroscopy mode were acquainted 56% of surveyees, but 96% of them were aware that careful planning and preparation for the procedure is one way of decreasing patient dose. 95% of the surveyees knew that by decreasing patients dose operator’s dose is decreased as well. 82% of them knew that patient dose can be reduced if AEC is used during the procedure and 47% are aware that use of magnification can influence patient dose.
Surveyees were asked to choose which of the offered means may reduce patient dose; distribution of answers to this question is shown in Figure 5; 30% of them recognised all offered answers as means for decreasing patient dose.
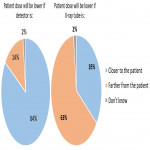
Distribution of answers to questions regarding influence of detector and X-ray tube distance from the patient is shown in Figure 6.
63% of surveyees is aware that skin deterministic effects may occur in case of more complex interventional procedures while 35% knew dose threshold for these effects; 74% was aware that avoidance of exposing the same area of the skin in different projections may reduce probability of occurrence of skin deterministic effects and 63% that lateral projections result in increase of patient dose.
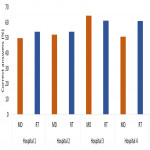
Overall results are shown in Figure 7. Almost half of the participants gained their knowledge from older colleagues and more than three quarters of them self-assessed their knowledge as insufficient. Similar knowledge of physician and radiographers was found but working experience in interventional suite was important. Also, level of the knowledge is lower in specialities other than radiology and/or cardiology. In hospitals where medical physicist is available better results were achieved in case of both, physicians and radiographers.