Prior to AVS, cross sectional imaging is undertaken to exclude some rarer causes of PA such as adrenal cortical carcinoma, which may warrant adrenalectomy without AVS. CT imaging is particularly useful as a pre-procedural planning tool, as it can help identify the location of the adrenal veins and establish any anatomical variants (4).
Medications that affect the renin-angiotensin-aldosterone axis will need to be withheld for a predetermined amount of time, depending on the medications in question. Heparin may be administered to reduce the risk of iatrogenic adrenal vein thrombosis. The procedure should preferably be scheduled in the morning during the peak of physiological cortisol levels (1, 4). The use of synthetic adrenocorticotrophic hormone (synthetic ACTH) prior to AVS remains a question of debate (1).
The adrenal veins can be sampled sequentially or simultaneously. In the case of sequential sampling, the right adrenal vein is often sampled first as it is the more difficult and more time consuming of the two; sampling the right vein first reduces the interval between sampling time of each vein.
The right adrenal vein is small (2-4mm in diameter) and short, most often entering the inferior vena cava at the T11/12 interspace from the posterolateral direction (1, 4) A number of discrepancies regarding the anatomy of the right adrenal vein may have an effect on the interpretability of any individual AVS, such as the possible presence of multiple right adrenal veins and the possible shared trunk with an accessory hepatic vein (1, 5). Multiple catheter options are available for the selection of the right adrenal vein, with caution being advised to avoid too deep of cannulation which may potentially sample beyond a tributary draining an APA or may increase the propensity for vein rupture/venous infarct.
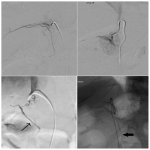
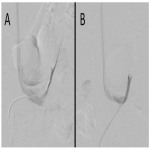
Once a prospective vein is cannulated, a venogram is performed utilizing digital subtraction angiography, to aid in confirming that an adrenal vein is cannulated. Careful low volume injection must be performed here to avoid vein rupture. The typical appearance of the right adrenal vein is a tangle of vessels at the location of the adrenal gland. The gland itself can have a varied appearance, sometimes demonstrating the diagnostic feature of an inferior emissary vein (1). Following confirmation of the correct venous target, aspiration of the vein is undertaken with great care. The first few mL of sample is usually discarded as it usually contains iodinated contrast agent.
In sequential sampling the left adrenal vein will be aspirated next. The let adrenal vein has a more predictable anatomic location, joining the inferior phrenic vein to form the phrenic adrenal trunk, which joins the superior aspect of the left renal vein. There are many catheter options available, with a Simmons-2 being a commonly used choice to distally enter the left renal vein first, then retracting the catheter to engage the phrenic-adrenal trunk (1, 4). Sampling this proximal common trunk rather than deeper cannulation is usually advised to avoid missing an aldosterone rich tributary, and to avoid possible adrenal vein thrombosis/vessel rupture (1). A small study of 22 patients has compared sampling the phrenic adrenal trunk with the adrenal vein proper, revealing no difference in the aldosterone/cortisol ratio at each site (6).
Interpretation of results can vary depending on the variety of selectivity indices used to determine sampling adequacy. Current guidelines suggest indices of >5 and >2 as adequate, depending on whether sampling is stimulated or unstimulated with synthetic ACTH respectively (1, 2, 4).