Type:
Educational Exhibit
Keywords:
Neuroradiology brain, MR, Education, Other
Authors:
A. Taylor, M. Chew, J. Drummond
DOI:
10.26044/ranzcr2023/C-275
Imaging findings OR Procedure details
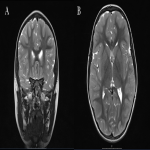
Cortical Tubers are a common radiological findings in TS, with a prevalence of over 90%(5). They are composed of disorganized neuronal and glial cells commonly seen in the frontal lobes (2). Studies have shown a link between the number of cortical tubers and cognitive disability, neurobehavioural disability and epilepsy (2, 6, 7).
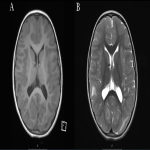
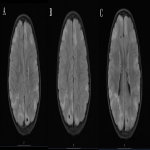
On MR imaging they are typically high signal intensity on T2W/FLAIR and low signal intensity on T1W (5). Due to lack of myelination, infants may display cortical tubers with inverse signal intensity patterns (2).
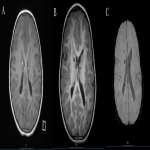
Subependymal nodules are benign hamartomatous tumours that occupy the lining of the ventricles occurring in more than 90% of people diagnosed with TS(8). Their natural history is they tend to calcify over a patient’s lifetime, with the vast majority being calcified by adulthood. Given the vast majority are calcified, CT imaging is the modality of choice. If they are not calcified they present with high-signal-intensity on T1W and Iso-signal-intensity on T2W and can have variable enhancement. Subependymal nodules are typically benign, however possess the ability to degenerate to Subependymal Giant Cell Astrocytomas(5).
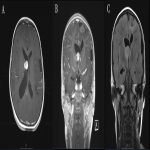
Subependymal-Giant-Cell-Astrocytomas (SEGA) are enlarged slow growing Subependymal Nodules. Due to their sluggish growth characteristics their prognosis is typically reasonable. Symptoms secondary to their mass effect can occur such as ventricular obstruction and hydrocephalus (5). SEGA have similar characteristics on MR imaging as subependymal nodules – although SEGAs commonly enhance this is not a reliable feature to differentiate from subependymal nodules. SEGAs can be comprised of solid and cystic components, and commonly found at the Foramen-of-Monro (8).
White matter abnormalities in TS include radial migration lines/bands, cortical tuber associated superficial abnormalities and white-matter cyst-like lesions. Typically, white matter abnormalities are T2 hyper intense and T1 iso to hypo intense (5, 9). Radial white matter bands are thin lines – curvilinear or straight- that represent pathological development of migratory pathways of neurons and glial cells (1, 5). Commonly these occur bilaterally in the frontal lobes (2). Superficial white matter abnormalities are usually associated with all cortical tubers, reflecting ‘reduced myelin or increased gliotic reaction’ (1). White-matter cyst-like lesions appear in deep white matter in proximity of the lateral ventricles, they are typically well demarcated and iso intense to Cerebrospinal Fluid (1, 5).