Keywords:
Abdomen, Interventional non-vascular, Urinary Tract / Bladder, CT, Ablation procedures, Complications, Neoplasia
DOI:
10.26044/ranzcr2023/C-66
Results
CASE REPORTS
CASE 1
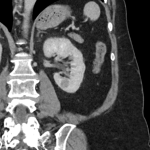
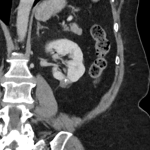
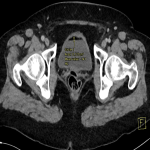
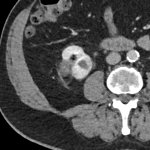
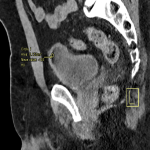
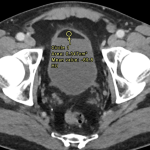
A 54-year-old female was undergoing staging contrast-enhanced Computed Tomography (CT) scans for her known anal squamous cell carcinoma, and had an incidental finding of a 1.1 cm predominantly hypoechoic renal lesion in the lower pole of the left kidney (Fig 1). A follow-up scan 1 year later demonstrated interval growth, with newest largest dimension measuring 1.8 cm. After discussion at a Urology multidisciplinary meeting and in consultation with the patient, the decision was made to proceed with renal microwave ablation. The procedure was performed using a 14-gauge probe with an energy of 100W over 6 minutes. Biopsy for histology was obtained at the time of the procedure, which demonstrated atrophic tubules and inflammatory changes, negative for malignancy. Follow-up imaging demonstrated adequate post-ablation appearances without evidence of recurrence (Fig 2). Imaging 1 year following ablation demonstrated a fat-fluid level in the bladder, consistent with post-ablation chyluria (Fig 3). The patient had a transient decrease in her plasma protein immediately following the procedure, which corrected spontaneously. She had no post-procedural urinary symptoms, and urine microscopy was normal. No treatment was required.
CASE 2
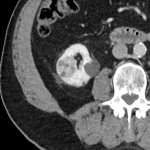
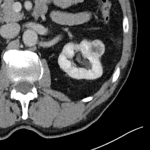
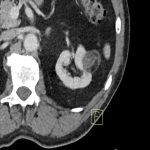
A 74-year-old male with a history of mechanical aortic valve, hypertension and sarcoidosis had an incidental finding of a 2.8 cm right renal lesion in 2013 and was undergoing yearly CT surveillance, which demonstrated an approximate 1 mm/year growth in the lesion (Fig 4). He was asymptomatic with no haematuria. Incidentally, on a scan performed in October 2017, a new left upper pole renal lesion was identified, measuring 2.7 cm in maximal dimension. Upon consultation with the patient and after discussion at a multidisciplinary meeting, the decision was made to proceed with bilateral renal microwave ablation, 1 month apart. The left renal lesion was ablated initially, using a 14-gauge probe with a 60W ablation for 10 minutes, with tract ablation. The right renal lesion was ablated 1 month later, requiring hydrodissection of the adjacent colon. The lesion was then targeted with a 14-gauge probe, with an 80W ablation energy over 10 minutes. Core-biopsy of the lesions with histology revealed a left-sided oncocytic tumour / chromophobe renal cell carcinoma, and a right-sided oncocytic tumour. Follow-up contrast-enhanced CT scan in February 2022 demonstrated adequate bilateral post-ablation appearances of both renal lesions (Fig 5), and fat-fluid density in the urinary bladder reflecting chyluria (Fig 6). The patient was asymptomatic, with no pain or haematuria post-procedure.
CASE 3
A 75-year-old male had an episode of right-iliac-fossa pain requiring a visit to his General Practitioner, on a background of non-bothersome lower-urinary-tract symptoms secondary to prostatomegaly. Investigation with contrast-enhanced CT was performed, which identified an incidental 2.3 cm left renal lesion (Fig 7). The patient had a history of hypertension, but otherwise no other social or occupational risk factors for urothelial malignancy, and no haematuria. The patient opted for renal microwave ablation instead of renal-sparing operative intervention, and underwent biopsy and ablation in December 2020. The renal lesion was ablated using a 14-gauge probe, with ablation settings of 140W for 6 minutes and tract ablation (Fig 8). Histopathology revealed a low-grade oncocytic lesion, with the differential of an oncocytoma / chromophobe renal cell carcinoma. Post-procedural contrast-enhanced CT performed in August of 2022 demonstrated fat-fluid level in the urinary bladder, in keeping with chyluria (Fig 9). The patient was asymptomatic, with no haematuria or lower urinary tract symptoms. Urine microscopy and blood biochemistry were normal.