Repeat measurements of the same parameters showed excellent concordance,
for instance hydration had a SEM of 3% (see figure 4).
Variation in measured erythema,
melanin,
hydration and transepidermal water loss (TEWL) in our untreated control was 20% or less over the two week period.
Measured elasticity was more variable with a standard deviation of 38-61%. Ultrasound related measurements were found to be strongly operator dependant (>10 operators in this study),
and were not analysed further.
With respect to hydration that is the focus of this presentation,
variation across time in our volunteer untreated patient was around 15% in upper and lower breast.
Importantly,
day-to-day variation of hydration was mirrored in the two measured breast areas,
indicative of patient-related changes over time rather than true measurement variability.
We recruited 43 patients between January and December 2015.
In keeping with most adjuvant breast cancer cohorts,
mean patient age was 64.8 years and mean BMI was 28.5.
We were unable to utilize RTOG toxicity grading due to an insufficient number of severe reactions and inter-observer variability in grading.
After exclusion of patients who did not meet our data acquisition threshold,
34 datasets remained.
For these 34 patients,
a total of 968 measurements of hydration were made throughout the study,
with a median of 11 (3-15) per tested site and median 29 (8-45) per patient.
Data did not meet criteria for normal distribution (QQ plot,
Shapiro-Wilk test),
and as such non-parametric analyses were employed for subsequent analyses.
Data was collapsed for each patient/site to mean value in 5-fraction intervals to account for variability in measurement times during radiation.
At baseline,
median hydration status was greater in lower breast at 227 (range 90-696) micro-Siemens (µS) compared with upper breast at 113 (range 58-310) µS or boost area at 147 µS (range 84-311) (p<0.01).
This is in keeping with higher moisture levels found in the inframammary fold.
During radiotherapy,
median hydration in each breast area for all patients reduced linearly as a function of fraction number by 23-29% at the end of treatment (p<0.005) (Figure 6).
There was a predominant return to median base-line hydration by first follow-up appointment 6-8 weeks post completion of radiotherapy.
To identify patients at risk of decreased breast hydration,
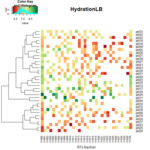
we next performed hierarchical clustering analysis on each area for each patient during radiotherapy (Figure 7).
This resulted in the identification of three distinct patterns of hydration change during treatment as summarised below.
- Group 1,
High hydration: Patients with high baseline hydration (mean 280 µS) who maintained hydration during treatment.
-
Group 2,
Low hydration: Patients with low baseline hydration (mean 150 µS) who maintained low hydration readings during treatment.
-
Group 3,
Intermediate hydration: Patients with intermediate baseline hydration (mean 220 µS) who developed lower hydration during radiotherapy (mean hydration at completion of treatment 120 µS).
When hydration over the course of radiotherapy was re-analysed by outcomes of clustering analysis,
only,
Group 3 patients showed significant progressive reduction in hydration status during radiotherapy,
with a decline of 42% in upper breast,
47% in the lower breast and 46% in boost areas (p<0.001)(Figure 8).
There was a decline late in treatment in Group 2 women,
but this did not reach statistical significance for the whole time-frame of radiation.
As there was general concordance between hydration status/change during radiotherapy at all 2-3 sites tested for an individual patient (not shown),
we next assessed whether this related to basic patient factors.
Age (p<0.045),
but not height,
weight or BMI,
was significantly related to hydration grouping,
with young patients having higher hydration levels and being less likely to experience changes during radiotherapy compared with those of low hydration status (Figure 9).
When we examined the use of topical preparations during radiotherapy (typically,
Solugel or Aqueous),
it seemed that patients with lower moisture levels tended to apply creams more often,
but that this did not appear effective in improving measured hydration.
There was insufficient data to test this statistically (Figure 10).