Purpose
Approximately 15% of patients with locally advanced rectal cancer achieve a pathological complete response (pCR) to standard neoadjuvant chemoradiotherapy with 45-50Gy[1-3]. Improving pCR may facilitate surgery-sparing treatment paradigms and improve overall oncological outcomes[4, 5]. Radiotherapy dose escalation above 60Gy was previously shown to improve pCR rates in a previous meta-analysis[6]; however, no review of the literature has considered outcomes in studies using modern inverse planning techniques or moderate escalation protocols (54-60Gy).
This systematic review and meta-analysis aimed to establish pCR, toxicity and clear margin (R0)...
Methods and materials
A systematic search of Pubmed, EMBASE and Cochrane databases for synonyms of ‘rectal cancer’, ‘radiotherapy’ and ‘boost’ was performed. Studies were screened for radiotherapy prescription >54Gy. Prespecified quality assessment adapted from the Joanna Briggs Critical Appraisal Checklist[7] was performed for meta-analysis inclusion suitability. Pooled estimates of pCR, acute toxicity (grade ≥3) and R0 resection rate were determined with random-effects restricted-maximum likelihood estimation. Heterogeneity was assessed with Higgins I2 and Cochran Q statistic. Subset analysis examined outcomes in modern inverse planning studies. Pooled estimates were calculated...
Results
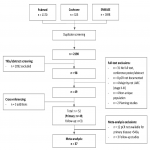
Forty-nine primary and three follow-up publications were included in systematic review after screening (see Fig 1).
[Fig 1]
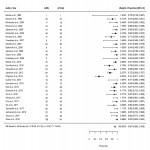
Prescribed standard radiation doses ranged from 37.8-54Gy, with boost dosing of 5-22.2Gy, resulting in a total radiotherapy dose of 54.6-65Gy administered in 23-38 fractions (EQD210 52.95-66.25Gy, median 56.42Gy). The proportion of patients completing a prescribed treatment course >54Gy was high (range 89-100%, median 100%) but was not reported in 11 publications.
Surgical interval varied (median: 8 weeks, range: 2-14 weeks) and was not specified in five publications....
Conclusion
Radiotherapy dose escalation above 54Gy is associated with high rates of pCR and does not appear to increase risk of acute grade ≥3 toxicity events. pCR rates approaching 25% may be achievable utilizing moderate escalation (54-60Gy) with modern inverse planning techniques; however, a clear dose-response relationship was not identified in regression analysis and additional evidence is awaited given the prevalence of heterogenous single arm studies to date.
References
[1] Sanghera P, Wong DW, McConkey CC, Geh JI, Hartley A. Chemoradiotherapy for rectal cancer: an updated analysis of factors affecting pathological response. Clin Oncol. 2008;20:176-83.
[2] Maas M, Nelemans PJ, Valentini V, Das P, Rödel C, Kuo L-J, et al. Long-term outcome in patients with a pathological complete response after chemoradiation for rectal cancer: a pooled analysis of individual patient data. Lancet Oncol. 2010;11:835-44.
[3] Ngan SY, Burmeister B, Fisher RJ, Solomon M, Goldstein D, Joseph D, et al. Randomized Trial of Short-Course Radiotherapy...