Keywords:
Colon, Gastrointestinal tract, Other, Radiation therapy / Oncology, Cancer
Authors:
N. Hearn1, D. Atwell1, K. Cahill1, J. Elks1, D. Vignarajah1, J. Lagopoulos2, M. Min1; 1Birtinya, QLD/AU, 2Sippy Downs, QLD/AU
DOI:
10.26044/ranzcr2021/R-0076
Results
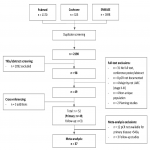
Forty-nine primary and three follow-up publications were included in systematic review after screening (see Fig 1).
Prescribed standard radiation doses ranged from 37.8-54Gy, with boost dosing of 5-22.2Gy, resulting in a total radiotherapy dose of 54.6-65Gy administered in 23-38 fractions (EQD210 52.95-66.25Gy, median 56.42Gy). The proportion of patients completing a prescribed treatment course >54Gy was high (range 89-100%, median 100%) but was not reported in 11 publications.
Surgical interval varied (median: 8 weeks, range: 2-14 weeks) and was not specified in five publications. Surgical complication data of patients treated to >54Gy was available in 25 publications, with median morbidity of 15% (range: 0-100%), median mortality of 0% (range: 0-6%) and median rate of anastomotic leakage 0% (range: 0-6%).
Survival data and late oncological outcomes were available in 22 primary and three follow-up publications. Functional assessment or patient-reported outcome measures were reported in only five publications. Late toxicity was reported in eight studies, four of which used standardised grading. The highest reported rate of late grade ≥3 toxicity was 14%.
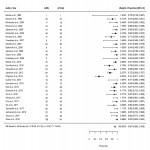
Pooled estimates of pCR, toxicity and R0 resection across 37 eligible publications eligible for meta-analysis (n = 1817 patients) were 24.1% (95% CI: 21.2-27.4%; see Fig 2), 11.2% (95% CI: 7.2-17.0%, see Fig 3) and 90.7% (95% CI: 87.9-93.8%, see Fig 4). Within inverse planning studies (17 publications, n = 959 patients), these rates were 25.7% (95% CI: 21.0-31.1%), 9.8% (95% CI: 4.6-19.7%) and 95.3% (95% CI: 91.6-97.4%).
Regression analysis did not identify any significant predictor of pCR (p > 0.05) nor account for between-study heterogeneity (R2 = 0%). Similarly, acute toxicity was not significantly related to any of the evaluated covarites (p > 0.05), nor account for significant heterogeneity (R2 = 8.02%). Rate of R0 resection positively correlated with the use of inverse-planning techniques (r = 1.0783, p = 0.0391) but no other cofactor (R2 = 24.90%), which may represent confounding by multifactorial improvements in outcomes in more recent trials.