Keywords:
CNS, Neuroradiology brain, Oncology, MR, Diagnostic procedure, Cancer, Metastases
Authors:
A. Lasocki1, L. Caspersz1, G. McArthur2; 1Melbourne, VIC/AU, 2Parkville, VIC/AU
DOI:
10.26044/ranzcr2021/R-0383
Results
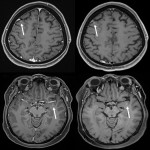
One hundred examinations were performed. Fifty-four patients (58%) were male and the median patient age was 63 years (range 27-87 years). Seventy-six examinations demonstrated no evidence of active IM when combining both sequences. Of the 24 examinations with active IM, T1-SPACE allowed the identification of additional lesions in five patients. In two of these patients, small solitary IM (measuring 5 mm and 4 mm) were not identified when first assessing MPRAGE, but were visible on T1-SPACE (Figure 1). Of note, both had also been missed during the routine clinical read (by non-study radiologists). In one of these patients, expedited follow-up imaging confirmed an IM, and prompted treatment with SRS. The other patient was treated systemically. Three further patients had some IM visible on MPRAGE, but T1-SPACE identified additional IM. In all five patients, the additional lesions identified on T1-SPACE were able to be subsequently identified on review of MPRAGE images. No additional findings were demonstrated by MPRAGE on the second round of assessment, when MPRAGE was assessed after T1-SPACE.
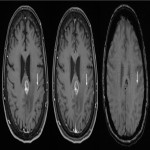
In 18 examinations, T1-SPACE identified additional equivocal findings which could not definitely be attributed to normal vessels, but were confidently attributed to artefact on subsequent review of the MPRAGE images (Figure 2). Seventeen were considered to represent normal vessels, and the remaining finding was attributed to motion artefact. Thus, based on correlation with MPRAGE, these findings were considered normal, and no additional imaging was required beyond routine follow-up. Figure 3 summarizes the additional findings identified on T1-SPACE.
Our findings are consistent with the existing literature, confirming that 3D-TSE improves detection of intracranial metastases. The identification of solitary small IM with the aid of T1-SPACE altered management, by allowing treatment at a smaller size. Even when IM are identified, there is potential benefit in identifying additional metastases if SRS is planned, as these additional lesions can be treated simultaneously. Reassuringly, while our findings support that using 3D-TSE alone may result in a higher FP rate, correlation with 3D-GRE allowed the uncertainties associated with 3D-TSE to be readily resolved.