Type:
Educational Exhibit
Keywords:
Interventional vascular, Catheter arteriography, Angioplasty, Stents, Thrombolysis, Acute, Aneurysms, Ischaemia / Infarction
Authors:
A. Dahan, M. Foo, M. Brooks, H. Asadi; Heidelberg, VIC/AU
DOI:
10.26044/ranzcr2021/R-0401
Imaging findings OR Procedure details
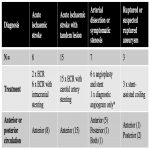
A total of 33 patients received IV ASA between October 2019 to October 2020 as part of an emergency neurointerventional procedure, including ECR, CAS, intracranial arterial stenting, angioplasty, stent-assisted coiling, and one diagnostic angiogram. Almost all patients were also given IV heparin as per institutional protocol and the neurointerventionalist’s discretion. The procedural details are summarized in Table 1.
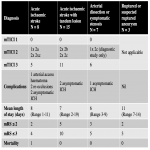
Amongst the three patients who underwent stent-assisted coiling for ruptured or suspected ruptured intracranial aneurysms, all cases were technically successful and there were no peri-procedural complications nor mortality (see Table 2). The mean length of stay was 11 days.
Amongst the 30 patients who received recanalization therapy, the ‘modified Thrombolysis In Cerebral Infarction’ (mTICI) score was used to grade technical outcome on final angiographic run, with successful reperfusion defined as any score above mTICI 2b.[12] 29 out of 30 patients (97%) had successful reperfusion, with 22 (73%) achieving complete reperfusion (mTICI 3). There was a single mortality, in a patient with AIS and a tandem occlusion secondary to an extensive carotid artery dissection; foretelling a poor prognosis from presentation. After ECR and CAS, the patient unfortunately suffered recurrent stent occlusions and eventual fatal cerebral infarction. Whilst there were no cases of symptomatic ICH, there were five cases of asymptomatic ICH and one arterial access haematoma, all of which were managed conservatively. The mean length of stay was 7 days for those presenting with AIS, and 6 days for those presenting with arterial dissection or symptomatic stenosis.
Short term clinical outcomes were also assessed in the form of ‘modified Rankin Scale’ (mRS) on discharge.[13] Amongst the whole cohort, 36% achieved an mRS score of 2 or less, implying functional independence, and 97% of patients (all except the one mortality) achieved mRS score of 3 or less, implying independent ambulation but assistance required for some daily tasks.