Keywords:
Head and neck, Other, Radiation therapy / Oncology, Cancer, Outcomes, Quality assurance
Authors:
R. Marwah, D. Goonetilleke, J. Smith, M. Chilkuri; Douglas, QLD/AU
DOI:
10.26044/ranzcr2021/R-0522
Conclusion
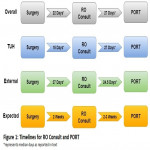
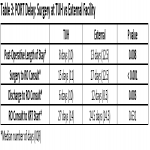
These findings reinforce that PORT delay for patients with HNSCC remains a prevalent issue. This study demonstrated that there was a delay from surgery to RO consult, especially for patients who had surgery at an external facility, highlighting the need to improve communication and coordination of care. Strategies being implemented to improve this include automated referrals from the head and neck multidisciplinary team (HNMDT) meeting and email communication to cancer care coordinators at both centres at the time of referral, with a weekly task generated via Oncology Information Systems (Mosaiq) for the TUH care coordinator to follow up on each patient’s status. Another prominent reason identified for delays was the time from RO consult to treatment start, demonstrating a need to improve timely institution of treatment. A strategy being implemented to improve this is the automatic generation of a treatment start date on the planning request form at the time of RO consult (that is 6 weeks from surgery date, taking into context the clinical situation) and to coordinate the planning process to ensure this timeframe is met. As an ongoing quality improvement strategy, automated quarterly reports will be generated and sent to the HNMDT to track and address gaps.