Keywords:
Head and neck, Other, Radiation therapy / Oncology, Cancer, Outcomes, Quality assurance
Authors:
R. Marwah, D. Goonetilleke, J. Smith, M. Chilkuri; Douglas, QLD/AU
DOI:
10.26044/ranzcr2021/R-0522
Results
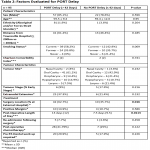
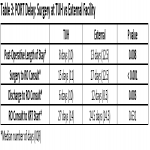
A total of 95 patients were included in the analysis. Overall, 71% (67/95) of patients experienced delay in starting PORT and 64% (61/95) had an OTT delay (Table 1). Aboriginal and Torres Strait Islander patients had a higher rate of PORT delay (89% vs 67%, n = 59, P = 0.204). Surgery at an external facility (tertiary referral hospital outside of Townsville) was significantly associated with a higher incidence of PORT delay (81% vs 58%, P = 0.016) (Table 2). Discharge to RO consult was a median of 6 days for patients who had surgery at Townsville Hospital, and 12 days for those from an external facility (p = 0.003) (Table 3).
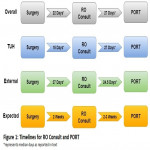
Overall, the median time from surgery to RO consult was 22 days and the median time from RO consult to PORT commencement was 27 days. The study found that 54% (n=51) of patients waited greater than 3 weeks after their surgery for an RO consult while 25% (n = 24) waited greater than 4 weeks (Figure 1, Table 2). For patients who waited greater than 4 weeks, the delay was secondary to one or more of the following: patient preference (21%), post-operative complications (54%), delay in post-operative referral (75%) and delay in RO consult (29%) (Figure 2). Despite this delay, there was a further delay from RO consult to PORT commencement in 75% of patients, and only 13% of patients were treated with accelerated fractionation to compensate for the delay.