Purpose
The purpose of this review is to retrospectively assess the approaches and management of traumatic splenic injuries over a twelve-month period at a major tertiary institution in Australia.
Methods and materials
Splenic injuries are one of the most frequently seen trauma-related injuries and can be classified as blunt or penetrating1. Non-operative management of blunt splenic injuries has become a widely-implemented standard of care. This has been facilitated in part by introduction of angioembolisation.2 The decision regarding conservative management, embolisation or surgery depends on factors including haemodynamic stability of the patient, splenic computed tomography (CT) injury grade, patient age and concurrent injuries.3,4
Traumatic splenic injuries are categorised in clinical practice using the American Association for the Surgery...
Results
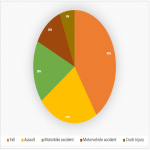
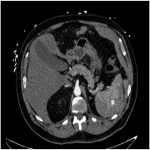
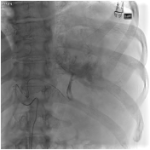
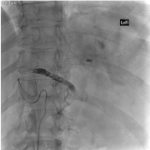
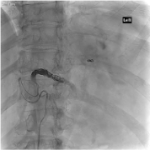
Twenty-two splenic embolisation procedures were undertaken at our tertiary trauma institution over the twelve-month period between January 2021 to December 2021. 82% of splenic embolisations occurred in the setting of blunt splenic trauma. Mechanisms of injury included falls (41%), assault (24%), motorbike accident (18%), motor vehicle accident (12%) and crush injury (6%). 18% of injuries were AASTgrade 5 and 59% were AAST grade 4. The remaining 23% were below AAST grade 4 but proceeded to embolisation given haemodynamic status or active bleed on CT. Embolisation...
Conclusion
We retrospectively analysed all blunt trauma-related splenic embolisations performed in our tertiary trauma institution over a one-year period. Angioembolisation remains a safe and effective treatment modality in the setting of traumatic blunt splenic injury. Our outcomes and approaches to traumatic splenic embolisation remains comparable with the available literature. Further analysis and research is required to determine the safety and efficacy of proximal and distal embolisation techniques.
References
1.Coccolini F, Montori G, Catena F et al. Splenic Trauma: WSES Classification and Guidelines for Adult and Pediatric Patients. World J Emerg Surg. 2017;12(1):40. doi.org/10.1186/s13017-017-0151-4
2.Schnüriger, B. , Inaba, K. , Konstantinidis, A. , Lustenberger, T. , Chan, L. & Demetriades, D. Outcomes of Proximal Versus Distal Splenic Artery Embolization After Trauma: A Systematic Review and Meta-Analysis. The Journal of Trauma: Injury, Infection, and Critical Care. 2011;70 (1), 252-260. doi: 10.1097/TA.0b013e3181f2a92e.
3.Ahuja C, Farsad K, Chadha M. An Overview of Splenic Embolization. AJR Am J...