Keywords:
Interventional vascular, CT-Angiography, Radioembolisation, Acute, Trauma
Authors:
J. Edey, D. MacManus, A. Halder
DOI:
10.26044/ranzcr2022/R-0078
Methods and materials
Splenic injuries are one of the most frequently seen trauma-related injuries and can be classified as blunt or penetrating1. Non-operative management of blunt splenic injuries has become a widely-implemented standard of care. This has been facilitated in part by introduction of angioembolisation.2 The decision regarding conservative management, embolisation or surgery depends on factors including haemodynamic stability of the patient, splenic computed tomography (CT) injury grade, patient age and concurrent injuries.3,4
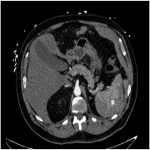
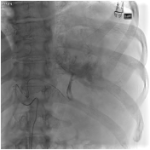
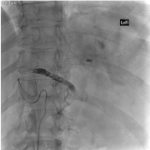
Traumatic splenic injuries are categorised in clinical practice using the American Association for the Surgery of Trauma (AAST) splenic trauma classification3, which grades injuries as I-V depending on extent of injury, depth and nature of haematoma or laceration identified on CT scan.1,5 For traumatic splenic injuries, splenic artery embolisation is often implemented if angiographic findings of active bleeding or presence of vascular injuries such as pseudoaneurysm and arteriovenous fistula are identified.3,6 Two commonly used embolisation approaches are distal and proximal splenic artery embolisation.7
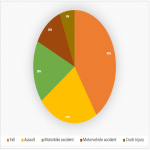
The departmental database was searched to identify all patients who had undergone splenic embolisation between January 2021 and December 2021. Selective retrospective chart reviews were performed using hospital electronic medical records. Information collected included patient demographics, severity of splenic injury, mechanism of injury, method of embolisation and complications. Data analysis was performed using descriptive statistics and Microsoft Excel.