Study Aim
To assess the diagnostic accuracy and clinical utility of PTLNB to guide optimal oncological management (allowing for clinical context) of patients with lung nodule(s) under respiratory and oncology investigation at CCLHD NSW regional thoracic oncology centre over 1.5 year period. Correlation with nodule size and morphology was also performed.
Methods
Retrospective study of consecutive series of adult patients undergoing PTLNB for focal lung lesion(s) was performed (with institutional Ethics Committee approval for quality improvement study).
There were 113 consecutive procedures in 111 patients (M = 62, F = 49; median age = 73 years) performed between July 2019 and December 2020. Data was collected regarding lesion size, morphology, procedure technique and biopsy pathologic findings. EMR charts were reviewed to assess impact of the PTLNB result on optimal oncology management. Final diagnosis was based on integrated imaging, pathologic and clinical outcome at >1 year follow-up.
Procedures were performed using intermittent CT fluoroscopic guidance by several IRs, general radiologists and supervised trainee registrars using range of techniques according to operator preference and individualised patient factors, with variable attendance of on-site cytopathologist.
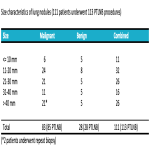
Lung nodule size was determined according to Fleischner society recommendations [8]:
(<= 10 mm (n=11); 11-20 mm (n=32); 21-30 mm (n=26); 31-40 mm (n=16); > 40 mm (n=26) [Fig 2].
Biopsy results were interpreted by single pathologist as integrated singular histology / cytology result.
Biopsy findings
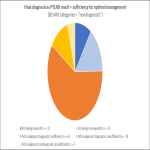
Final diagnosis was of a malignant nodule in 83/111 cases, and benign disease in 28/111 cases [Fig 3].
Two patients with lung adenocarcinoma underwent repeat biopsy. One patient required repeat sampling to complete molecular characterisation (initial biopsy was positive for adenocarcinoma); the other patient required second procedure after the first biopsy showed atypical cells only.
PTLNB result showed benign disease in 28 procedures (specific diagnosis in 11/28 cases, and other benign findings or insufficient material in 17/28 cases) [Fig 3].
Benign diagnoses included: abscess with organism identified n=5, hamartoma n=3, sarcoid n= 1, LCH n=1.
Malignant pathology was diagnosed in 85 procedures: NSCLC n=61, small cell lung cancer (SCLC) n=5, metastatic disease n= 13, lymphoma n=4 .
Overall per procedure analysis showed 91/113 (80.5%) procedures were diagnostic for either specific benign disease or definite malignancy.
Nondiagnostic rate was 22/113 (19.5%) for all nodules, and 11/43 (25.6%) for nodule <= 20 mm.
Malignant nodules
There were 85 PTLNB procedures in 83 patients with final diagnosis of malignancy [Fig 3].
80/85 (94.1%) procedures showed true positive malignancy.
5/85 (5.9%) procedures were false negative. 3 of these were subsolid nodule morphology, and 1 lesion was > 10 cm with necrosis. Final diagnosis of malignancy in these cases was achieved by: surgical resection / biopsy n=3, repeat percutaneous biopsy n=1, clinical outcome consensus n=1.
In further 13/85 (15.3%) procedures the results were insufficient for complete tumour immunohistochemical and molecular characterisation to determine optimal targeted immunotherapy, despite true positive diagnosis of malignancy.
67/85 (78.8%) procedure results were completely sufficient for oncology management, showing true positive malignancy with full pathological profile for optimised treatment.
For malignant nodules <=20 mm (n=30), PTLNB was inadequate in 5/30 (16.7%) [failed to confirm malignancy in 3/30 (10%); limited by insufficient material for full typing in further 2/30 (6.7%)]. 3 out of these 5 cases showed subsolid character nodule.
Example cases
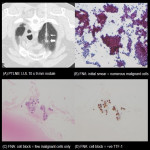
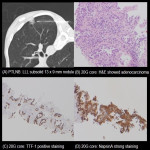
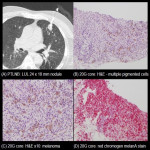
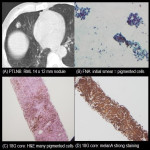
PTLNB of LUL 10 x 9 mm nodule showed lung adenocarcinoma - insufficient for molecular testing (haemoptysis limiting procedure) [Fig 4] compared with PTLNB of LLL 13 x 9 mm nodule showed lung adenocarcinoma - sufficient for complete molecular testing [Fig 5].
PTLNB of LUL 24 x 18 mm nodule showed metastatic melanoma - insufficient for molecular testing (mainly due to cell loss during multiple slide cut downs) [Fig 6] compared with PTLNB of RML 14 x 12 mm nodule showed metastatic melanoma - sufficient for complete molecular testing [Fig 7].