Type:
Educational Exhibit
Keywords:
Artificial Intelligence, Conventional radiography, Technology assessment, Quality assurance
Authors:
S. Karunasena, M. Vasimalla, C. Jones
DOI:
10.26044/ranzcr2022/R-0203
Conclusion
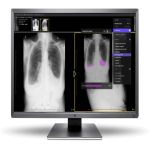
For AI assist devices to positively impact healthcare, as intended by their developers, successful implementation into clinical practice is of utmost importance. Integration into existing RIS and PACS systems, across multiple sites, with varying clinical settings and a diverse mix of users, is inherently complex. Through careful planning the use of pre-determined success metrics, we have demonstrated how successful device implementation can be achieved.
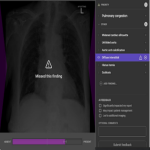
Results from both the pilot study and the post-implementation survey indicated that the AI device was very well integrated into the existing radiologist workflow, and users were not detracted from using the device due to technical difficulties or lack of understanding with regards to how to use the device. All radiologists in the pilot study agreed there was no significant learning curve as a hurdle to going ahead and using the device.
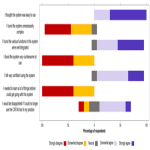
Radiologists’ feedback, from per-case data and post-pilot survey data demonstrated that device use led to changes in a significant proportion of CXR reports. Importantly, the proportion of result changes was higher with radiologists who had less consultant radiologist experience (0-5yrs) compared to the whole group. It would be interesting to explore this impact with radiologists in training – it is suspected that this group would have even more significant increases in report accuracy from the use of an AI assist device and ultimately availability of this tool would improve patient care. The effect on reporting accuracy with AI device usage with respect to level of radiology experience, including radiologists in training as a experience group, would be a good avenue for further research.
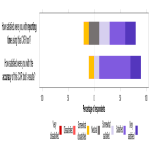
Feedback after wider implementation showed the majority of radiologists who had access to the device continued to use it at the two-month mark, and indicated it positively impacted their reporting. There was no perceived reduction in efficiency with use of the device which is thought to be a major contributing factor in the high rate of adoption – with pressures surrounding volume of work in busy healthcare systems, radiologists would be less likely to use a tool that was associated with a time cost, even it if increased their accuracy. The fact that 25% of radiologists felt the AI device improved their efficiency is another testament to good planning with regards to technical integration. Perhaps the best indicator of successful device implementation is that the majority of radiologists who participated in providing feedback stated they would be disappointed if device access was lost.
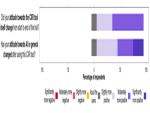
Furthermore, the feedback demonstrated radiologists’ attitude towards this AI assist device, and the use of AI devices in clinical practice in general, improved after using this device. This positive perception is without doubt a highlight of this review, as it paves the way for more AI assist devices to be implemented into clinical practice with the common goal of improving patient care in the landscape of a national healthcare system.