Keywords:
Musculoskeletal system, Neuroradiology peripheral nerve, MR, Imaging sequences, Other
Authors:
L. Pugh, T. Lloyd
DOI:
10.26044/ranzcr2022/R-0244
Purpose
Thoracic outlet syndrome (TOS) consists of upper limb neurological and vascular symptoms due to compression of the neurovascular bundle as it passes through the thoracic outlet1. Compression may occur within the interscalene space, the costoclavicular space and the recto-pectoralis minor space however is most common within the costoclavicular space and is exacerbated by abduction of the arm which further narrows this space2. The aetiology of neurogenic thoracic outlet syndrome is thought to most likely be due to hyperextension neck injury (which may be minor) in patients with underlying predisposition due to anatomical variability3.
Vascular thoracic outlet syndrome can be diagnosed with Doppler ultrasound and CT (Computed Tomography) angiography displaying compression / stenosis of the vascular structures. Despite being the more common subtype with a neurogenic component present in up to 95% of cases of thoracic outlet syndrome3,5 the diagnosis of neurogenic thoracic outlet syndrome is often more challenging. Clinical features are generally vague and overlap with other causes of nerve compression and pain syndromes4. Clinical tests are often positive in asymptomatic volunteers1 and often rely on arterial compression, which is a poor indicator of neurological compression of the brachial plexus3. The classical presentation described is upper limb paresthesia and pain exacerbated by certain shoulder movements including abduction. The exact location of symptoms varies depending on the level of compression. Weakness and muscle atrophy feature as late signs5.
Despite the challenging clinical picture, the diagnosis of neurogenic thoracic outlet syndrome is traditionally considered a clinical diagnosis with sensitivity and specificity of MRI thought insufficient to contribute meaningfully6. Although data remains limited, recent literature suggests that with improvement in MRI technique and dynamic imaging7, with the ability to often demonstrate direct compression of the plexus with the use of 3T MRI8,9.
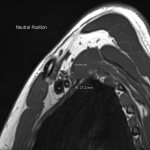
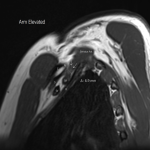
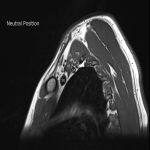
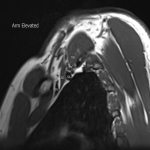
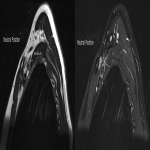
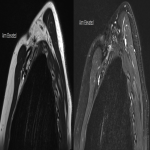
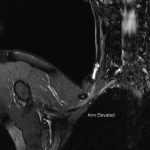
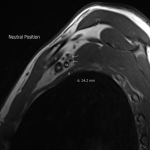
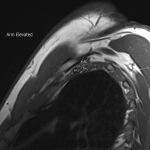
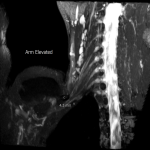
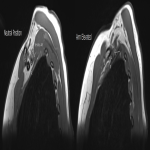
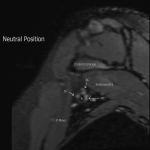
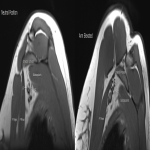
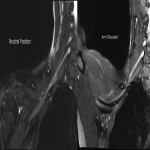
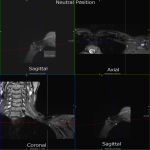
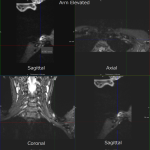
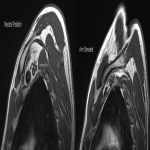
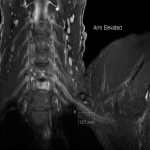
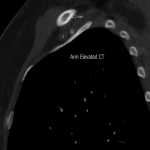
The dynamic and positional nature of thoracic outlet syndrome has been outlined in the literature with dynamic MRI demonstrating more marked reduction in the costoclavicular space with the shoulder abducted in patients with thoracic outlet syndrome compared to a cohort of asymptomatic volunteers10. Neurovascular compressions are often not demonstrated in the neutral position, highlighting the necessity for dynamic MRI10. In contrast, the scalene triangle and rectopectoralis minor space demonstrate an equal or lesser degree of compression in thoracic outlet syndrome patients compared to asymptomatic patients3.
In this case series, we outline our tertiary Australian hospital experience with dynamic brachial plexus MRI demonstrating narrowing of the costoclavicular space and brachial plexus compression with the arm abducted, and subsequent surgical outcomes in these patients.