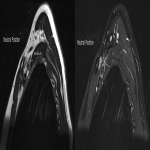
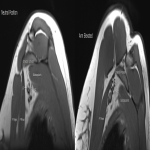
Case 1: A 23-year-old male office worker with long term clinical picture in keeping with neurogenic thoracic outlet syndrome, including pain, dysesthesia, and reduced power in the left upper limb, worsened with the arm positioned overhead. Subtle muscle wasting was present to supraspinatus, deltoid and abductor digiti minimi muscles. Roos test was positive.
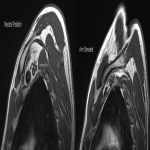
MR (sagittal T1) demonstrated reduction of the costoclavicular space with dynamic manoeuvres from 27mm to 7mm resulting in bony compression of the brachial plexus within the costoclavicular space. Contour abnormality of the plexus was also demonstrated.
The patient underwent a left first rib excision. At surgery a bulky anterior scalene muscle and fibrous bands tethering the plexus and subclavian artery were identified. Significant improvement in the patient’s pain and muscle power was demonstrated at post-surgical clinic review.
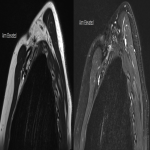
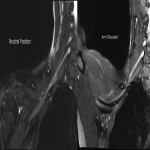
Case 2: A 43-year-old female with clinical right neurogenic thoracic outlet syndrome, in particular right forearm neuropathic pain. Sagittal T1 images again showed significant narrowing of the costoclavicular space with the minimum distance in neural and abduction 20mm and 4mm respectively, with loss of the normal fat signal surrounding the plexus. Coronal T2 STIR images demonstrated an abnormal buckled contour of the brachial plexus with subtle reduction in T2 signal of the plexus within the costoclavicular space.
The patient underwent right first rib resection with good clinical outcome and improvement in neuropathic pain.
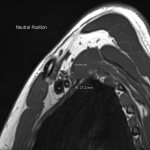
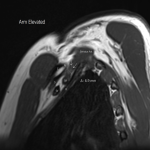
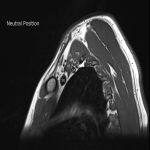
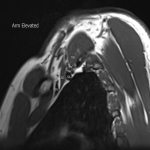
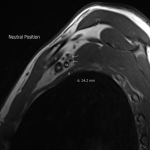
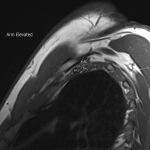
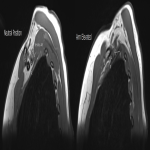
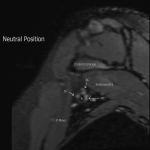
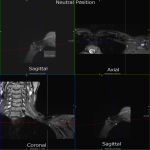
Case 3: A 34-year-old male patient with a clinical picture consistent with neurogenic thoracic outlet syndrome. MR images (T1 weighted sagittal) show a capacious costoclavicular space in the neutral position measuring 24mm at the narrowest point. With the arm elevated, this reduced markedly to a minimal distance of 4mm, with the brachial plexus interposed between the clavicle and first rib at this point. Flattening of the subclavian vein was also demonstrated. No variant anatomy or other cause for compression was seen either radiographically or surgically. The patient underwent resection of the right 1st rib with good clinical response.
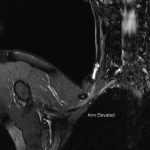
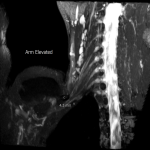
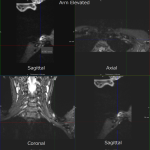
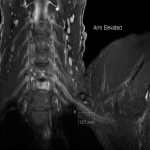
Case 4: A 27-year-old female patient with clinical features in keeping with right sided neurogenic thoracic outlet syndrome. MR images (3d SPACE STIR images formatted in a coronal plane) demonstrate narrowing of the costoclavicular space, with the arm elevated, to 6mm. Minor compression of the subclavian artery is also seen.
The patient underwent partial first rib resection and scalenotomy with no compressive lesion or variant anatomy identified at surgery.
Case 5: A 49-year-old female patient with a prolonged symptoms of neurogenic thoracic outlet syndrome including neck, chest, upper back and upper limb pain, paraesthesia, muscle weakness and muscular atrophy. MR images demonstrated significant narrowing of the costoclavicular space with the arm elevated narrowing from 26mm to 5mm.
The patient underwent decompressive surgery with first rib resection and anterior and middle scalenectomy with thoracic outlet syndrome confirmed with the presence of extensive scar tissue surrounding the brachial plexus. In addition, fibromuscular bands between the anterior and middle scalene muscles were also identified. The patient had clinical improvement although not entire resolution of symptoms, which could relate to the duration of the compression prior to release.
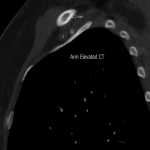
The cohort of 50 patients undergoing CT chest examinations for non-brachial plexus/thoracic outlet pathology had an average minimum costoclavicular distance of 13.5mm (range 5-24, SD 4.6). This distance aligned with that described in the literature10. All five patients in the case series were in the lower range of costoclavicular distance, with three of the five falling more than two standard deviations below the mean. Although the sample size is small and the comparability of the CT distance to that of the MR study is uncertain, the findings support the suggestion that the costoclavicular distance is narrower in patients with neurogenic thoracic outlet syndrome. The findings also suggest a wide variability of normal degrees of compression within the general population, highlighting the importance of radiological and clinical correlation.