Keywords:
Arteries / Aorta, Pulmonary vessels, Respiratory system, CT, CT-Angiography, Audit and standards, Screening, Acute, Embolism / Thrombosis
Authors:
K. P. Settipalli, B. Powell
DOI:
10.26044/ranzcr2023/C-301
Conclusion
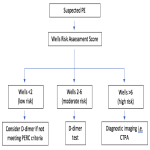
The positivity rate of 11.1% is lower than the reported yield rates at other Australian hospitals and significantly less than the Royal College of Radiologists recommended rate of 15.4-37.4%. The RESPECT-ED study reported an average positive rate of 14.6% among 15 Australian emergency departments18 and the Canberra Hospital and Health Service reported 16.2%5. This suggests that appropriate use of D-dimer testing in accordance with the QH diagnostic pathway has a large potential to reduce CTPA utilisation. Only 31.4% of patients in the low to moderate risk group, who did not meet the PERC criteria, received D-dimer testing, suggesting that D-dimer testing could have conceivably avoided up to 68.6% of the CTPAs in this group.
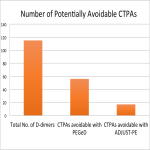
Additionally, the results show low levels of compliance with ADJUST-PE and minimal use of PEGeD criteria. Overall, it was poorly documented as to which, if any, criteria was used and some patients proceeded to CTPA despite a D-dimer level that could have precluded this for reasons not documented. Compliance with ADJUST-PE criteria could have avoided 4.4% (17) CTPAs and PEGeD could have avoided 14.8% (56) CTPAs in the low to moderate risk group if used appropriately. Given the poor uptake of D-dimer testing in general, it is difficult retrospectively validate these criteria and evaluate their potential ability to prevent negative diagnostic studies, however these results do suggest PEGeD has a greater potential to decrease CTPA use than ADJUST-PE.
These results indicate other factors are involved in the decision-making process when investigating for possible PE. These factors require further characterisation in additional research in order to determine the cause for low CTPA yield. Additionally, the importance of accurate documentation of the clinical risk assessment and Wells score should be further emphasised. Integrating the QH diagnostic pathway into the Electronic Medical Records may help to address these issues and serve as a reminder to follow the pathway for ordering clinicians. Further larger prospective trials are needed to validate the use of ADJUST-PE and PEGeD criteria.