The primary goal of diagnostic testing in suspected PE is to identify patients with a high risk of deterioration or clot progression necessitating treatment with anticoagulation2. Due to its protean presentation, this presents a common clinical challenge for which the evidence-base has changed rapidly over the last ten years.
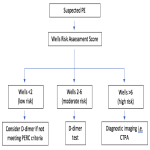
A significantly lower diagnostic yield of CTPAs in recent decades suggests an issue of overutilisation in emergency departments3,4. The QH suspected PE diagnostic pathway5 recommends the use of the Wells score, a validated clinical decision tool designed to risk stratify a patient’s pre-test probability for PE with the potential to reduce CTPA utilization without increasing the risk of missing PE diagnoses6,7,8.
For patients with a low to moderate pre-test probability (Wells score 0 to 6), a serum D-dimer measurement can exclude the presence of a clot and obviate the need for a CTPA if it is lower than a pre-defined threshold value
9. The Choosing Wisely Australia campaign in conjunction with the Royal Australian and New Zealand College of Radiologists supports the use of this clinical decision rule
7.
Several studies have shown that D-dimer levels increase with age10,11, thereby limiting the yield and cost-effectiveness of D-dimer testing among older patients. The QH pathway recommends the use of an age-adjusted D-dimer threshold of age × 10 ng per milliliter in patients greater than 50 years old, and a threshold of 500 ng per milliliter in patients aged less than 50 years old6. This is in accordance with the criteria used in the ADJUST-PE study12,13 which showed an increased specificity of age-adjusted D-dimer values in older populations while maintaining negative predictive value14.
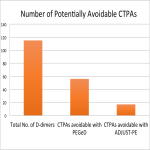
In the Pulmonary Embolism Graduated D-dimer (PEGeD) study, a D-dimer threshold of less than 1000 ng per milliliter in those with a Wells score of 4 or less, and a threshold of less than 500 ng per milliliter in those with a Wells score between 4 to 6, showed an increase in the percentage of patients who had PE excluded by D-dimer testing alone and further decreased the need for CTPA when compared with the age-adjusted strategy. PEGeD criteria reduced the number of patients proceeding to CTPA from 51.9% when the standard D-dimer threshold of 500 ng per milliliter in low risk patients was used, to 34.4%. Furthermore, there was no increase in clinically significant adverse outcomes and no patients who had PE excluded by D-dimer testing had a venous thromboembolism (VTE) on follow-up15.
While it is well established that PE can be excluded with a Wells score less than 2 and a D-dimer less than 500 ng per milliliter3,16, there is little Australian specific data to support the use of the age adjusted ADJUST-PE or pre-test probability adjusted PEGeD criteria17, and the rate of utilization of such evidence in Australian emergency departments is currently poorly characterized.
Methods
A retrospective review of Synapse, our imaging viewer, was performed to identify CTPA examinations ordered in 2020. From this a random sample of cases was selected.
Inclusion criteria
- ED patients aged over 16 years old presenting to our ED with a clinical history or examination findings suggestive of PE
- CTPA performed for clinical suspicion of PE
- CTPA ordered by ED staff
Exclusion criteria
- CTPA showing equivocal/non-diagnostic results
- Non-diagnostic quality CTPAs due to contrast timing or artifacts
- PE was an incidental finding (e.g. during malignancy staging or investigation for infection)
- Known pregnancy
- CTPA not ordered by ED staff
Using these studies, a detailed appraisal of the clinical notes, medical history, vital signs and D-dimer result if tested was performed. If a Wells score was not documented, a retrospective Wells score was calculated using the criteria listed on the QH Suspected PE diagnostic pathway4. A score of 3 points for PE as the likeliest diagnosis was given if it was documented as the top differential or if the documented clinical findings would not make an alternate diagnosis more likely. Vital signs at triage, if available, or at time of clinician review were used. If there was no documentation of signs of current deep VTE, previous VTE, haemoptysis, malignancy history or previous immobilisation/surgery within 4 weeks, the patient did not receive points for those criteria.
Those who received a D-dimer test were reviewed to determine whether either ADJUST-PE or PEGeD criteria were utilised or could have been used to avoid the CTPA.