Aims and objectives
Pulmonary vasculitis is a life-threatening complication of systemic lupus erythematosus (SLE).
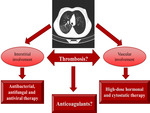
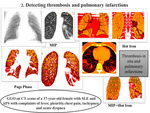
Due to the presence of antiphospholipid syndrome (APS) thrombosis in situ can occur in any SLE patient especially with pulmonary vasculitis [1].
The diagnosis of vasculitis relies on a combination of clinical features,
chest imaging,
lung function test results and histopathology [2].
On computed tomography (CT) scans,
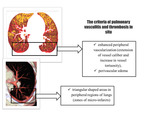
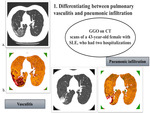
pulmonary vasculitis is characterized by the appearance of ground-glass opacity (GGO).
However,
GGO is a non-specific pattern that can refer either to the interstitial or vascular involvement...
Methods and materials
Study population
Between 2013 and 2015,
inNorth-Western State Medical University named after I.I.
Mechnikov (Saint Petersburg),
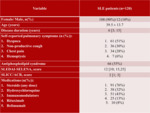
120 patients (Table 1),
aged 39.5 ± 13.7,
with active SLE (SELENA-SLEDAI 12[10; 15.25]),but without known chronic respiratory diseases,
underwent laboratory tests,
electrocardiograms and echocardiograms,
pulmonary function and imaging tests at baseline and after 6 months of therapy.
55% of SLE patients had secondary APS.
Imaging tests
Patients were prospectively assessed usingGE LightspeedVCT64 SliceCT Scanner.
For reconstruction of standard native CT scans we used work station,
which includespost-processing software....
Results
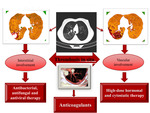
According to the diagnostician's conclusionsan addition of post-processing software to CT increased sensitivity of CT in diagnosis of pulmonary vasculitis and thrombosis in situ in patients with SLE and APS (Fig. 3).
No differences in assessmentinvolved regions were detected during the comparison of the results of color maps with CT angiograms (p = 0.031) and perfusion scans (p=0.042).
Statistics showed that the mean area under the receiver operating characteristic curve value increased significantly (p<0.05) by using post-processing software in assessment of pulmonary vasculitis (Fig. 4)...
Conclusion
Addition of post-processing software to CT analysis improved diagnostic performance in diagnosis of pulmonary vasculitis and thrombosis in situ in patients with SLE and APS.
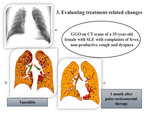
Color mappingequips radiologists to more easily differentiate between vascular and interstitial involvement and evaluate treatment-relatedchanges.
Post-processing techniques should become a routine part of radiological practice in pleuropulmonary pathology in SLE and APS as they can be a useful addition to native CT scans (Fig. 9) and assist clinicians with the diagnosis and treatment planning.
Personal information
Iana Leineman,
MD
Department of radiology and radiotherapyof NWSMU named after I.I.
Mechnikov
Russia,
Saint-Petersburg,
191015Kirochnaya str.
41
E-mail:
[email protected]
Regina Faizenberg,
MD
Department of radiology and radiotherapyof NWSMU named after I.I.
Mechnikov
Russia,
Saint-Petersburg,191015Kirochnaya str.
41
Tamara Golimbievskaya,
MD,
PhD
AssociateProffessor
Department of radiology and radiotherapyof NWSMU named after I.I.
Mechnikov
Russia,
Saint-Petersburg,191015Kirochnaya str.
41
Irina Itskovich,
MD,
PhD
Proffessor
Head of Department of radiology and radiotherapyof NWSMU named after I.I.
Mechnikov
Russia,
Saint-Petersburg,191015Kirochnaya str.
41
Mihail Shostak,
MD,
PhD
Associate Proffessor
Department of...
References
Kevin K.
Brown.Pulmonary Vasculitis /Proceedings of the American Thoracic Society.
- 2006 Mar.
– Vol.
3,
N 1.
– P.
48–57.
Kim J.S.
Thoracic involvement of systemic lupus erythematosus: clinical,
pathologic,
and radiologic findings/ J.S.Kim,
K.S.
Lee,
E.M.Koh//Journal of Computer Assisted Tomography. — 2000.— Vol.
24,
N 1.— P.
9–18.
Kakati S.
Pulmonary manifestations in systemic lupus erythematosus (SLE) with special reference to HRCT/ B.
Doley,
S.Pal,
U.
J.Deka//Journal of AssociationofPhysiciansofIndia. — 2007.— Vol.
55.— P.
839–841.