Authors:
M.-G. Knuttinen, T. G. Van Ha, C. Straus, B. Funaki; Chicago, IL/US
Purpose
Percutaneous radiofrequency ablation (RFA) of liver tumors has been extensively described and is considered safe and effective. It continues to be a promising technique in prolonging survival by achieving local control while preserving local liver parenchyma.
The location of these tumors, however, has its own unique challenges. Lesions must be carefully selected as unintended thermal injury to nearby structures can occur and has been reported in percutaneous, laparoscopic and open procedures (Siperstein et al, 2000; Pearson et al, 1999). Since the liver is closely opposed to the diaphragm, injury to the diaphragm is a major concern in the ablation of subcapsular lesions in proximity to the diaphragm. Clinically, diaphragmatic injury causes pain, diaphragmatic paralysis as well as other abdominal and thoracic complications.
Targeted CO2 insufflation has been described as a way to manipulate intra-abdominal organs to gain safe access routes (Raman et al, 2004). In particular, Raman et al described CO2 insufflation as a way to minimize diaphragmatic injury in a porcine model during RFA. However, these authors stressed several drawbacks to this technique including possible increased risk of bleeding, limited role of ultrasound guidance, and inherent risks of CO2 insufflation. Additional studies have focused on the use of a saline barrier, though this may be difficult especially in the liver dome and in areas where there is no confined space to maintain the saline infusion (Raman et al, 2002). Other authors have performed a transpleural approach for certain dome lesions, but this carries a risk of pneumothorax, hemothorax, symptomatic pleural effusions and diaphragmatic thermal injury (Venkatesan et al, 2006).
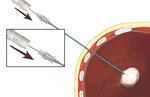
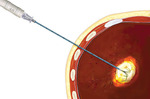
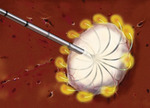
We offer the novel approach of using an angioplasty balloon catheter as a protective device serving as a barrier between the ablated liver and the diaphragm. This technique might provide a safe and effective way to expand the use of percutaneous RFA of liver tumors that are in the undersurface of the diaphragm. Additionally, this technique could be used as an aid in protection of other organs adjacent to areas being ablated.