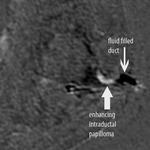
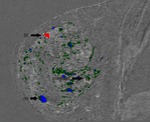
Purpose
Breast MRI has been shown to be a highly sensitive (71-100%) method for the detection of breast cancer.
However,
false negative examinations do occur.The relatively poor specificity (68% for the American College of Radiology Imaging Network (ACRIN) 6883 trial) of breast MRI,
compared with mammography (93-100%),
has been a major concern.(1) The false positive rates cited by prior studies are 32.2 to 40.6%(1-3).
False positives studies lead to further testing and unnecessary biopsies,
thereby increasing costs,
morbidity,
and patient anxiety.
False positive diagnoses result from...
Methods and Materials
We retrospectively assessed diagnostic performance for 1,100 consecutive screening (n=349) and diagnostic (n=751) cases performed from April 2006 to December 2007 for women aged 25-89 from four sites for which dedicated breast MRI reports and ground truth (biopsy for cancer cases; one year negative follow-up for negative cases).
Screening examinations were indicated based upon family history,
carriers or relatives of genetic mutations associated with breast cancer risk,
high risk syndromes,
high risk histology,
breast density,
or prior personal history of breast cancer.
Diagnositic study indications...
Results
Using BIRADS 4-6 as positive interpretations sensitivity,
specificity,
PPV and NPV were (231/239 (96.6%),
742/86 (86.2%),
231/350 (66%) and 742/750 (98.4%) respectively.
The area under the MRI receiver operating characteristic (ROC) curve was 0.956.
When the BI-RADS 6 cases are excluded the sensitivity decreases 92/100 (92%),
but the specificity increases 741/834 (88.9%).
As expected,
if BI-RADS 3 are included as positive,
the sensitivity increases 233/239 (97.5%) but the specificity decreases 645/861 (74.4%).
For the screening cohort,
the sensitivity and specificity were 6/6 (100%) and 325/342...
Conclusion
The dedicated breast MR system led to significantly better diagnostic performance for all case metrics (sensitivity,
specificity,
NPV,
PPV,
and ROC area than has been historically reported for breast MRI employing conventional scanners.There usually is a tradeoff,
such that higher sensitivity is related to lower specificity and vice versa.
In this study,
however,
the dedicated breast MRI system achieved higher sensitivity,
while the false positive rate actually was lower than in studies evaluating breast MRI performed on whole body scanners.
The lack of specificity of...
References
Bluemke DA,
Gatsonis CA,
Chen MH,
et al.
Magnetic resonance imaging of the breast prior to biopsy.
JAMA 2004; 292:2735-2742.
Teifke A,
Hlawatch A,
Beier T,
et al.
Undetected malignancies of the breast: dynamic contrast-enhanced MR imaging at 1.0 T.
Radiology 2002; 224:881-888.
Fischer U,
Kopka L,
Grabbe E.
Breast carcinoma: effect of preoperative contrast-enhanced MR imaging on the therapeutic approach.
Radiology 1999; 213:881-888.
Personal Information
Steven E.
Harms,
MD,
FACR is recognized nationally in the area of magnetic resonance imaging (MRI).
He was formerly on the faculty at the University of Arkansas for Medical Sciences (UAMS),
Baylor University Medical Center in Dallas,
and M.
D.
Anderson Cancer Institute.
During his 14 years as director of MRI at Baylor,
Dr.
Harms and his research team developed numerous MRI applications including TMJ,
knee,
orbit and RODEO Breast MRI.
He is past president of the Society of Magnetic Resonance in Medicine and received...