Keywords:
Breast, MR, Mammography, Ultrasound, Equipment, Imaging sequences, Technical aspects
Authors:
S. Harms1, B. J. Hillman2, G. Stevens3, R. Stough4, A. Hollingsworth4, K. Kozlowski5, L. Moss6; 1Fayetteville, AR/US, 2Philadelphia, PA/US, 3Bastrop, TX/US, 4Oklahoma City, OK/US, 5Knoxville, TN/US, 6Worcester, MA/US
DOI:
10.1594/ecr2012/B-0799
Results
Using BIRADS 4-6 as positive interpretations sensitivity,
specificity,
PPV and NPV were (231/239 (96.6%),
742/86 (86.2%),
231/350 (66%) and 742/750 (98.4%) respectively.
The area under the MRI receiver operating characteristic (ROC) curve was 0.956.
When the BI-RADS 6 cases are excluded the sensitivity decreases 92/100 (92%),
but the specificity increases 741/834 (88.9%).
As expected,
if BI-RADS 3 are included as positive,
the sensitivity increases 233/239 (97.5%) but the specificity decreases 645/861 (74.4%).
For the screening cohort,
the sensitivity and specificity were 6/6 (100%) and 325/342 (94.8%) respectively.
The diagnostic cohort had a sensitivity and specificity of 225/233 (94.4%) and 415/517 (74.6%) respectively.
A total of 13/120 (11%) false positive cases were considered high risk histologies for which excision or chemoprevention is commonly recommended,
including lobular carcinoma in situ (6),
atypical ductal hyperplasia (1),
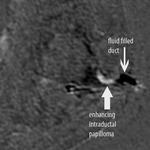
atypical lobular hyperplasia (4) and papilloma (2). The false negative cases consisted of subtle ductal carcinoma in situ (DCIS) (2/6 33%) and infiltrating ductal carcinoma (4/6 66%).
When diagnogstic data from MRI,
mammography,
and sonography were all availble,
the ROC curve areas were 0.956 for MRI,
0.851 for mammography,
and 0.864 for breast sonography.