Purpose
To identify an optimal imaging strategy for the accurate detection of urgent conditions in patients with acute abdominal pain.
Methods and Materials
Imaging plays an important role in the treatment management of patients because clinical evaluation results can be inaccurate.
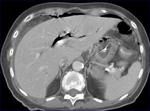
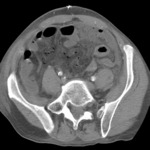
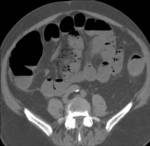
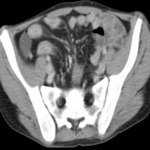
Performing CT is most important because it facilitates an accurate and reproducible diagnosis in urgent conditions.
321 patients with non-traumatic abdominal pain of 2- 120 hours duration.
All patients had plain radiographs abdominal,
ultrasonography,
and CT after clinical and laboratory examination.
Results
58% patients had a final diagnosis classified as urgent.
The initial clinical diagnosis resulted in many false positive urgent diagnoses,
which were significantly reduced after radiographs,
ultrasonography or CT.
Interpretation of abdominal radiographs was nonspecific in 67% patients,
normal in 23%,
and abnormal in 10%.
CT detected more urgent diagnoses than did ultrasonography: sensitivity was 89% (95% confidence interval 87% to 92%) for CT and 70% (67% to 74%) for ultrasonography (P<0.001).
Abdominal radiography had 0% sensitivity for appendicitis,
pyelonephritis,
pancreatitis,
and diverticulitis.
Sensitivities of...
Conclusion
Although CT is the most sensitive imaging investigation for detecting urgent conditions in patients with abdominal pain,
using ultrasonography first and CT only in those with negative or inconclusive ultrasonography results in the best sensitivity and lowers exposure to radiation.
References
Erik K.
Paulson,
Courtney A.
Coursey CT Protocols for Acute Appendicitis: Time for Change.
AJR 2009; 193:1268–1271
Shannon P.
Sheedy et al.
CT of Small-Bowel Ischemia Associated with obstruction in Emergency Department Patients: Diagnostic Performance Evaluation1 Radiology: Volume 241: Number 3—December 2006
Sun Ho Ahn et al.
Acute Nontraumatic Abdominal Pain in Adult Patients: Abdominal Radiography Compared with CT Evaluation.
Radiology 2002; 225:159–164
Andersson RE,
Petzold MG.
Nonsurgical treatment of appendiceal abscess or phlegmon: a systematic review and meta-analysis.
Ann Surg 2007; 246:741–748