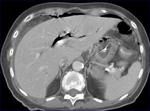
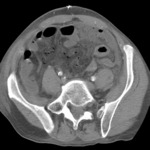
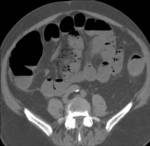
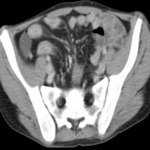
58% patients had a final diagnosis classified as urgent.
The initial clinical diagnosis resulted in many false positive urgent diagnoses,
which were significantly reduced after radiographs,
ultrasonography or CT.
Interpretation of abdominal radiographs was nonspecific in 67% patients,
normal in 23%,
and abnormal in 10%.
CT detected more urgent diagnoses than did ultrasonography: sensitivity was 89% (95% confidence interval 87% to 92%) for CT and 70% (67% to 74%) for ultrasonography (P<0.001).
Abdominal radiography had 0% sensitivity for appendicitis,
pyelonephritis,
pancreatitis,
and diverticulitis.
Sensitivities of abdominal CT were highest for bowel obstruction and urolithiasis at 75% and 68%,
respectively.
The presence of oral contrast material can aid evaluation of the appendix because,
first,
appendicitis is unlikely in the setting of a contrast-opacified appendix and,
second,
the appendix may be more readily identifiable if the terminal ileum and cecum are opacified with
oral contrast material
Acute appendicitis is particularly difficult to diagnose in the patient with very little or no retroperitoneal adipose tissue.
Conversely,
images of an obese patient or a patient with a large pelvis are prone to degradation from noise artifact.
An optimal imaging strategy in patients with abdominal pain would lead to timely identification of urgent conditions,
without exposing patients to unnecessary forms of imaging.
The results confirm what we knew intuitively: CT is more accurate than plain films.
Although CT is more expensive and exposes patients to higher radiation doses,
it makes little sense to order plain films when it’s likely that the patient will end up undergoing CT anyway.