Conventional radiography has an important place in bone lesion.
In lytic lesion,
it either helps to do the diagnosis or is sufficient to do it and avoid other needless exam.
Once a lytic lesion is identified,
a radiologist must be able to provide a definitive diagnosis or a reasonable differential diagnosis for the lesion and provide appropriate recommendations to the referring clinician.
To approach the diagnosis of an osteolytic lesion ,
some radiographic signs have to be described and constitute clues for diagnosis. After their description,
they are confronted to some epidemiologic data and the clinical context.
I-Radiographic signs
I-1-Patterns of osteolysis:
The radiological appearances of bone destruction has been summarized in a classification system by Lodwick.
The system is very useful to describe the aggressiveness of a bone tumor.
Lodwick described three types of destruction
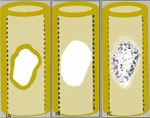
I-Geographic destruction (Fig. 1):
IA: geographic sclerotic margin
IB: geographic unsharp margin
IC: geographic no margin
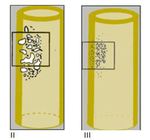
II-Moth eaten like destruction (Fig. 2):
Areas of destruction with ragged borders.
Destruction is similar to moth-eaten clothes with holes of destroyed bone. It implies more rapid growth
III-Permeative destruction (Fig. 2 ):
Ill defined lesion with multiple “worm holes”; It implies an aggressive malignancy
I-2-Matrix:
In regard to tumor matrix,
mineralization of both chondroid and osteoid matrix can be visible on radiographs.
Mineralization of chondroid matrix is seen as dot-like,
popcorn-like,
arcs and rings of calcifications within the bone tumor,
while osteoid matrix has a cloud-like,
wispy,
cotton like appearance.
Some lesions that can have radiographically visible chondroid matrix include enchondroma,
chondroblastoma,
and chondrosarcoma.
Osteoid matrix can be seen in osteosarcoma and osteoid osteoma/osteoblastoma.
I-3-Periosteal reactions:
Periosteal reaction is either solid or interrupted.
Interrupted periosteal reaction indicates that the associated lesion is aggressive
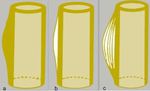
-solid periosteal reaction(Fig. 3):With slow-growing processes,
the periosteum has plenty of time to respond to the process.
That is,
it can produce new bone just as fast as the lesion is growing.
Therefore,
one would expect to see solid,
uninterrupted periosteal new bone along the margin of the affected bone.
-lamelatted periosteal reaction(Fig. 3 b,c): with rapidly growing processes,
the periosteum cannot produce new bone as fast as the lesion is growing.
Therefore,
we see an interrupted pattern which can manifest itself in several ways,
depending on just how steadily the lesion grows.
If the lesion grows unevenly in fits and starts,
then the periosteum may have time to lay down a thin shell of calcified new bone before the lesion takes off again on its next growth spurt.
This may result in a pattern of one or more concentric shells of new bone over the lesion.
This pattern is sometimes called lamellated or "onion-skin" periosteal reaction
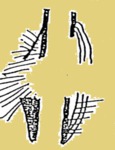
-sunburst,
hair on end (Fig. 4): If the lesion grows rapidly but steadily,
the tiny fibers that connect the periosteum to the bone (Sharpey's fibers) become stretched out perpendicular to the bone.
When these fibers ossify,
they produce a pattern sometimes called "sunburst" or "hair-on-end" periosteal reaction,
depending of how much of the bone is involved by the process.
-Interrupted periosteal reaction(Fig. 5):
Codman’s triangle: When a process is growing too fast for the periosteum to respond with even thin shells of new bone,
sometimes only the edges of the raised periosteum will ossify.
When this little bit of ossification is seen tangentially on a radiograph,
it forms a small angle with the surface of the bone,
but in fact not a complete triangle.
So,
when a process is growing too fast for even the Sharpey's fibers to ossify,
one may only see a soft tissue mass arising from the bone,
perhaps with small Codman's triangles at its margins or a plurilamellar interrupted periosteal reaction
- complex pattern of periosteal reaction (a fracture or infection in the same area as a tumor)Fig. 6
I-4-Extension:
-soft tissue extension: Usually implies malignancy or aggressive benign lesion such as osteomyelitis with infiltration of fat
-multiple lesions
II) Clinical data and location
II-1-Age
the age of the patient is an important piece of information in musculoskeletal radiology.
Typically,
only certain lesions occur within any given age range; therefore,
the age of the patient must be considered in order to generate a correct differential diagnosis
II-2-Clues by location of lesion:
II-2-1-In the transverse plane:
Location in the transverse plane can lead to diagnosis:
Central (enchondroma),
Eccentric (giant cell tumor,
chondromyxoid fibroma),
Cotical (Non ossifying fibroma,
osteoid osteoma),
Parosteal (parosteal osteochondroma)
II-2-2-In the longitudinal plane :
-Epiphyseal
-Metaphyseal
-Diaphyseal
II-2-3-Characteristic location:
Some locations lead to particular diagnosis ( e.g chordoma for the clivus or the sacrum,
adamantinoma for the tibia…)
II-3-Clinical and biological data:
It is important to consider the clinical and biological context,
e.g; A lytic lesion in patient with pain,
fever ,
a hyperleucocytosis reminds an osteomyelitis…
When a lytic lesion is suspected,
the radiologist must keep in mind the possibility of a normal variant,
such as a pseudocyst and the existing of “leave me alone lesion”.
Indeed,
those lesions are benign and have a characteristic radiographic appearance and/or location that are inherently diagnostic and have to be known to avoid further unnecessary exams.