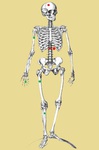
I-Benign Bone forming tumors
I-1.Osteoid osteoma(OO):
Definition : OO is a benign tumor containing a nidus of osteoid tissue hypervascularized.
Its size is less than 2 cm.
It is surrounded by reactive sclerosis.
The recent nidus is hypervascularized,
the former is calcified.
Frequency :12% of benign bone tumors.
Age 10-30 years.Sex ratio 2 - 3 H / 1 F
Clinical presentation :
-nocturnal pain relieved by aspirin.
-Stiff and painful scoliosis without neurological signs in children.
-Swelling.
The osteoid osteoma simulating a joint arthritis.
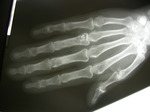
Topography(Fig. 7):
Metaphysis or diaphysis of long bones: superior extremity of femur,
tibia and humerus.
Posterior arch of the spine (lumbar),
hands,
feet.
Cortical,
spongy or sub periosteal bone (femoral neck and slope).
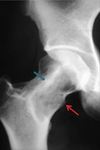
Conventional radiography:
A geographical Osteolysis <2 cm,
sometimes calcified,
surrounded by a large condensation which sometimes blows the cortical bone and can hide the nidus.
Sometimes periosteal reaction.
Spine: enlarged hemi-arch in the concavity of the scoliosis.
Sub periosteal: notch and peripheral condensation.
Intra-articular:effusion,
weakness,
some condensation: simulates arthritis .
Scintigraphy Te99m :
Central intense uptake in a diffuse uptake.
Useful if pain and normal standard radiography.
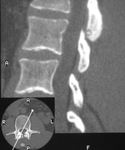
CT examination(Fig. 8,
Fig. 9):
the best exam to find the nidus.
Contrast injection is unnecessary.
MRI :
Nidus is poorly visible.
It shows peripheral edema(hypointense T1,
hyper intense T2,
contrast enhancement),
which mimics infection or malignancy.
Differential diagnosis:
bone forming tumors,
sclerotic lesions,
bone lesions with radiolucent centers,periosteal reaction,infection,osteosarcoma,Hemangioma ,osteoma
Treatment Options for this Tumor:
-Surgical excision of the nidus
-Percutaneous destruction with laser ,
Radio frequence or ethanol.
I-2.Osteoblastoma(OB):
Definition:Osteoblastoma is a solitary,
benign bone-forming tumor also called "giant osteoid osteoma" because size> 2 cm.
Comparing to OO,
peripheral sclerosis is less important but OB more frequently thins the cortex and blow-out the bone.
Frequency: 3% of benign bone tumors.
Age:10 to 30 years Sex ratio: 1H/2 F.
Clinical presentation : Less painful than osteoid osteoma,
scoliosis rare.
Topography(Fig. 10):
-Spine: posterior arch (lower back)
-Metaphysis or diaphysis of long bones (femur,
tibia,
humerus): Cortical,
medullary or periosteal.
-Skull,
face,
mandible (cementoblastoma),
extremities.
Conventional radiography:
-Spine:geographic osteolysis or condensation,
important cortical blowhole
-Long bone: geographic osteolysis,
condensation rarer than osteoma osteoid,
the bone loss may contain ossifications.
Sometimes,
pseudo-malignant feature.
-Cementoblastoma: ossified lesion surrounded by a radio-transparent halo.
-Extremities: gap containing partitions with cortical blowhole.
Scintigraphy :uptake Simulator to that of osteoid osteoma.
CT: bone matrix,
thin cortical but continous .
MRI : hypointense on T1,
moderate hyper signal on T2.
Peritumoral edema
Clinical form: aggressive osteoblastoma or malignant:
Radiological signs: as osteoblastoma but Local recurrence and sometimes metastasis.
Differential Diagnosis:
The differential diagnosis of osteoblastoma includes osteoid osteoma,
osteosarcoma,
giant cell tumor and aneurysmal bone cyst.
Treatment Options for this Tumor:
A biopsy is performed to confirm the diagnosis.
Surgical resection by curettage,
intralesional excision or en-bloc excision are all treatment options depending on the site.
Cryosurgery,
radiation and chemotherapy may be used in aggressive and surgically unresectable lesions of the spine.
I-3.Osteoma:
Histology: Development of dense bone from the periosteum.
Frequency: 0.4% of the population.
Age : from 30 to 50 years,
Sex ratio: 2 H / 1 F
Clinical presentation: asymptomatic: incidental finding on imaging of the sinuses.
Symptoms only present if their location within the head and neck region is causing problems with breathing,
vision,
or hearing.
Sometimes: swelling,
recurrent sinusitis,
mucocele.
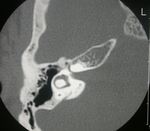
Topography(Fig. 11):frontal sinus (50%),
other sinuses,
skull,
maxilla,
Internal auditory meatus ,
rarely long bones
Conventional radiography: Central osteomas are well delineated sclerotic lesions with smooth borders,
without surface irregularities or satellite lesions; very dense opacities,
homogeneous,
well circumscribed,
round or lobed(Fig. 12).
Peripheral osteomas are radiopaque lesions with expansive borders that may be sessile or pedunculated.
CT : incidental findings.
Clinical forms:
• Gardner syndrome:
- Autosomal dominant.
Multiple osteomas (sinus and long bones)
+ Polyposis coli (risk of degeneration) + dental anomalies
+ Soft tissue tumors (fibroma,
lipoma subcutaneous,
desmoid tumor,
epidermal cyst) .
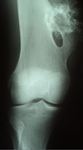
• Parosteal osteoma:
- Border-malignant Benign because of local recurrence.
From 20 to 40 years,
posterior knee.
Dense juxta-cortical mass lobed.
Differential diagnosis:
Need to be differentiated from enostosis which also appear as densely sclerotic well-defined lesions on x-ray.
Treatment options:
If asymptomatic : abstention.
If cosmetic problem or local complication: Surgery.
I-4.Bone island
It consists of well-differentiated mature bone tissue within the marrow,
also referred to as enostosis.A coincidental finding.
Differential diagnosis: osteoblastic metastasis (breast- or prostate cancer).
II-Benign cartilage forming tumors:
II-1.Chondroma
Definition : Enchondroma is a solitary,
benign,
intramedullary cartilage tumor
Frequency: 12% of benign bone tumors.
Age: from 20 to 40 years,
Sex ratio: 1H/1F
Clinicalpresentation: asymptomatic,swelling,pathologic,fracture,
deformities.If pain appears and the tumor increases in size,
suspect malignant transformation,
especially if the tumor was near the belts.
Topography(Fig. 13): small bones of the hands (50%) (metacarpo phalangeal),
feet,
long bones (meta or diaphysis),
rib
Conventional radiography: geographic osteolysis borded with osteosclerosis,blowhole cortical,
containing pitted calcifications(Fig. 14).
The tumor may be consists in a heap of calcifications (Fig. 15).
CT scanning : analysis and detection of calcifications of the matrix.
MRI: T1 hypo intense,
T2 hyper intense (hyaline cartilage rich in water) calcifications :low signal on T1 and T2.
Late contrast enhancement with speckled appearance(Fig. 16).
Complications:
-Fracture
-Degeneration in chondrosarcoma: the risk increases near the belts,
very rare in extremities.
Clinical forms:
1. Ollier’s disease:
is not hereditary, unilateral shortening or deformity of a limb;
Many chondromas of the long bones,
high risk of degeneration.
2.
Maffucci syndrome : multiple Enchondromatosis with angiomatosis of soft parts ,phleboliths soft tissue,
high risk of degeneration.
3.
Juxtacortical chondroma : calcified soft tissue mass adjacent to the cortical bone of a finger or a toe.
Differential diagnosis:
-In some locations it can be difficult to differentiate between enchondroma and bone infarct.
-It is almost impossible to differentiate between enchondroma and low grade chondrosarcoma based on radiographic features alone.
Features that favor the diagnosis of a low-grade chondrosarcoma:
-Higher age
-Size > 5 cm
-Activity on bone scan
-Fast enhancement on dynamic contrast enhanced MR series
-Endosteal scalloping of the cortical bone
Treatment options:
asymptomatic chondroma in extremities : Abstention
Painful or worrisome lesions should be treated with biopsy followed by intralesional resection.
Large defects can be filled with bone graft.
All specimens must be analyzed carefully for malignancy.
II-2.Chondroblastoma
Histology: benign tumor made of chondroblasts, giant cells and cartilage.
frequency : <1% of primary bone tumors
Age: 5 to 25 years ,
sex ratio : 2 H / 1 F
Clinical presentation : pain,
restricted mobility.
Topography(Fig. 17): epiphyses of long bones before welding of the cartilage growth : humerus ,
femur,
tibia, apophyses,
pelvis,
tarsus and patella.
Conventional radiography: geographic osteolysis with dense peripheral osteosclerosis ,
sometimes blowhole cortical,
calcifications and solid periosteal reaction.
CT: detection of calcifications,
bone cortical thin
MRI: Needless,
sometimes misleading.
Intermediate signal on T1 and T2,
peripheral rim of low signal on T1 and T2.Peripheral edema (hypo intense T1,
hyper intense T2) : reminds pseudo-osteitis or malignant tumor.
Clinical forms:
- Extension to the metaphysis,
- blowhole cortical
- Expansion to joints,
- Pseudo-aggressive feature(Fig. 18,Fig. 19,Fig. 20)
- condensing tumor
Differential diagnosis: of an epiphyseal lesion in young patients: chondroblastoma,
osteomyelitis and ganglion cyst.
Treatment options: surgery
II-3.Chondromyxoid fibroma(CMF)
Definition : benign tumor containing fibrous tissue,
chondroid and myxoid.
Frequency: 0.5% of primary bone tumors.
Age: 10 to 30 years,
sex: H> F
Clinical presentation : moderate pain,
chronic functional disability.
Topography(Fig. 21): metaphyses of long bones of the lower limb mainly proximal tibia
Conventional radiography(Fig. 22): geographic osteolysis,
multilobed,
with dense peripheral rim and partitions.
Although the name suggests that CMF is a chondroid lesion,
calcifications are usually not seen.
Sometimes blowhole cortex.
Clinical form:
- Central location: fusiform expansion.
- Eccentric lesion: cortical sometimes invisible on conventional radiography.
- Hemispherical bone defect: cortical notch.
- Pseudo-malignant feature: cortical destruction,
periosteal reaction.
Differential diagnosis: CMF resembles Nonossifying fibroma
Treatment options: surgery
II-4.Exostosis = Osteochondroma:
Definition: Solitary osteochondroma is a developmental abnormality of bone.
It occurs when part of the growth plate forms an outgrowth on the surface of the bone.
This bone outgrowth may or may not have a stalk.
When a stalk is present,
the structure is called pedunculated.
When no stalk is present,
it is called sessile It is covered with a cartilaginous cap <1 cm in adults)
Frequency : 35-40% of benign bone tumors
Age : 10 to 30 years sex equally in males and females
Clinical presentation: asymptomatic,
sometimes pain,
swelling.
If increases in volume in adult suspect degeneration in chondrosarcoma.
Topography(Fig. 23): metaphyses of long bones (lower limbs> upper limbs),
belts,
ribs,
posterior vertebral arch.
Conventional Radiography(Fig. 24): perpendicular to the metaphysis,
goes to the diaphysis.
The cortical and cancellous bone of the exostosis and the bone holder are in continuity.
Sessile or pedunculated.
Cap sometimes calcified.
CT: cartilage cap <1 cm.
MRI : may be used to look for cartilage on the surface of the bony growth Cortical low signal on T1 and T2 ,
spongy fat signal
Cartilaginous cap hypointense T1,
hyperintense T2: <1 cm.
No contrast enhancement early.
Calcifications not seen.
Complications
1 - Degeneration in chondrosarcoma
-Radio standard: cortical break,
large calcifications in soft tissue.
-CT: dense matrix in the center,
anarchic calcifications,
cap cartilaginous> 1 cm,
regardless of mineralized tissue,
a lot of soft tissue
-MRI : cartilage cap> 1 cm,
contrast enhancement .
2 - Neurovascular compression : Pseudo-aneurysm (popliteal artery).
3 - Bursitis of the Knee or the shoulder.
Fluid collection sometimes containing calcifications (ultrasound).
4 –Spinal cord compression
5 – Pathologic fracture
Clinical form
1 – Exostosis disease family:
Autosomal dominant, occurs <20 years: Multiple exostoses,
extended femoral necks,
coxa valga,
short ulna,
curved,
radial head dislocation.
High risk of complications.
2 – hemimelic epiphyseal dysplasia:’ Tarsomegaly’
unilateral epiphyseal exostosis <10 years.
Talus,
tarsal bones,
lower extremity of the femur and tibia.
Hypertrophy of the pineal gland (calcified mass).
3 - Post-radiation osteochondroma
4 - Sub-ungual Exostosis - First toe
Treatment options:
Aymptomatic exostosis: abstention.
If suspected degeneration: Surgical biopsy
III-Fibrous bone lesions:
III-1.Fibrous Cortical defect (FCD) and non-ossifying fibroma (NOF):
Definition: It is a benign well-defined lesion made of fibrous tissue,
fibroblasts and giant cells.
Generally,
the FCD for the young child disappears during growth.
NOF probably corresponds to a FCD non-involuted.
FCDs are small (< 3 cm),
eccentrically located,
metaphyseal cortical defects,
fibroxanthomas (>3 cm) are larger,
eccentric,
intramedullary lesions that abut the cortex; they have a typical,
superficial,
scalloping pattern in the adjacent cortex.
Frequency: FCD: 30 - 40% of children from 6 to 11 years,
NOF: 5% of benign bone tumors biopsied.
Sex ratio: 1.5 H / 1F
Clinical presentation: asymptomatic,
except if pathologic fracture (FNO).
Topography(Fig. 25): FCD: cortical metaphysis of long bones: femur,
tibia,
fibula and humerus.
NOF: the same location but may concern medullary.
Conventional radiography(Fig. 26):
FCD: well defined cortical osteolysis.
NOF usually has a sclerotic border and can be expansile.
NOF may occur as a multifocal lesion.
No periosteal reaction (except if pathological fracture).
The radiographic appearance is almost always typical
CT scan and MRI are needless: they show the cortical lysis.
MRI shows fibrous signal (low signal T1 and T2) and different aspect of contrast enhancement.
Scintigraphy: needless: fixing small.
Evolution:
DC disappears or condenses.
FNO migrates to the diaphysis and / or condenses; They regress spontaneously with gradual fill in.
Clinical form:
Jaffe-Campanacci syndrome: association of multiple non-ossifying fibromas with cafe au lait skin patches,
mental retardation,
hypogonadism or cryptorchidism,
ocular disease and cardiovascular malformations.
The FNO disappear spontaneously.
The multiple FNO are found in 38% of cases of neurofibromatosis.
Neurofibromatosis was found in 5% of cases of multiple FNO.
Treatment options:
DC: no treatment.
FNO: abstention or curettage filling depending on the size and symptoms.
III-2.Fibrous dysplasia:
Definition: It is an uncommon benign disorder characterized by a tumor-like proliferation of fibro-osseous tissue: an immature tissue that cannot differentiate into mature bone.
This may be due to a mutation in a cell surface protein.
It is normally a monostotic (solitary) tumor that arises during periods of bone growth in older children and adolescents and slowly enlarges.
Frequency: Monostotic fibrous dysplasia accounts for 75 to 80% of cases.
Polyostotic fibrous dysplasia may occur as multiple lesions in adjacent bones and accounts for 7% of benign bone tumors.
Most patients are diagnosed in the first three decades of life.
Polyostotic fibrous dysplasia are typically diagnosed in the first decade of life.
Sex: Females and males are equally affected.
Topography(Fig. 27): Fibrous dysplasia can occur anywhere but is usually found in the proximal femur,
tibia,
humerus,
ribs,
and craniofacial bones.
Skeletal deformities can occur as a result of repeated pathological fractures through affected bone.
Clinical presentation: Monostotic fibrous dysplasia is asymptomatic incidentally finded on x-ray.
Pain and swelling at the site of the lesion or pathological fracture can also be present.
Female patients may have increased symptoms during pregnancy.
Conventional radiography(Fig. 28):
Well defined osteolytic lesion in a long bone with a ground glass or hazy appearance of the matrix.
There is a narrow zone of transition and no periosteal reaction or soft tissue mass.
The lesions are normally located in the metaphysis or diaphysis.
There is sometimes focal thinning of the overlying cortex,
called "scalloping from within".
The radiological appearance can be a bone deformity,
discrete lucency,
patchy,
sclerotic,
expansile.
FD may also contain cystic parts,
calcifications and ossifications.
MRI or CT scans can be helpful in delineating the extent of the lesion and identifying possible pathological fractures
Clinical forms
-autosomal dominant disorder affecting the mandible and maxilla bones in children in their teenage years.
-Polystotic fibrous dysplasia is known to have multiple associations with other disorders:
*Albright's syndrome: combination of polyostotic fibrous dysplasia,
precocious puberty,
and cafe au lait spots
*Mazabraud's syndrome: association of fibrous dysplasia and soft tissue tumors
*Other endocrine abnormalities including hyperthyroidism,
Cushing's disease,
thyromegaly,
hypophosphatemia,
and hyperprolactinemia have been associated with fibrous dysplasia.
Differential diagnosis:
-In young patients with location in proximal humerus or femur: solitary bone cyst or aneurysmal bone cyst.
-In eccentric locations: NOF or adamantinoma (tibia).
-When calcifications are present: chondroid lesion (enchondroma).
Treatment:-the biopsy confirms the diagnosis,
but surgery is not necessary for an asymptomatic lesion unless there is a risk for pathological fracture.
-Lesions whose behavior is latent do not need any evaluation or treatment because of the high risk of local recurrence after surgery.
-After surgery,
biphosphate medicines long-term are effective in reducing symptoms and increasing cortical thickness.
IV- Vascular bone lesion: Hemangioma
Definition:It is a benign bone common lesion characterized by vascular spaces lined with endothelial cells.
Age:The peak incidence is in the fifth decade
Sex ratio: 1male/2females.
Topography(Fig. 29): About 50% of osseous hemangiomas are found in the vertebral bodies (thoracic especially) and 20% are located in the calvarium.
The remaining lesions are found in the tibia,
femur and humerus ( Metaphysis or diaphysis)
Clinical presentation: asymptomatic,
discovered on x-ray or autopsy.
Vertebral hemangiomas can cause neurological symptoms if they extend into the epidural space.
Symptoms may vary with other factors that cause vascular distension or reactivity,
such as dependency,
activity,
pregnancy and menstruation.
Conventional radiography(Fig. 30 ): It depends on the location of the lesion:
-Asymptomatic vertebral angioma: Demineralization with coarse vertical trabeculae: grid aspect,
a"corduroy" appearance.
-Symptomatic and compressive vertebral angioma T3 - T9: blowing the posterior wall,
extending into the posterior arch and the soft tissues.
-Calvarial angioma : geographic gap containing honeycomb,
blowing the cortical: resemble radiating wheel spokes.
-Hemangiomas in the metaphysis or epiphysis of long bones appear as poorly defined lytic lesions that give a spiculated pattern known as "Irish lace".Normally there are multiple,
small,
somewhat irregular lytic areas surrounded by variable areas of scelrosis.
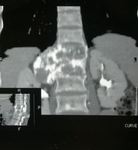
CT(Fig. 30):
• Asymptomatic vertebral body angioma: on axial CT scan,
vertebral body lesions have a "polka dot" pattern as the vessels are seen in cross section,
surrounded by fat (d <- 30 UH)
• Symptomatic and compressive vertebral angioma : irregular trabeculae (honeycomb) surrounded by a stroma tissue density (> 20 HU),
hypervascular and sometimes soft tissue damage behind the posterior vertebral wall (bilobed aspect).
MRI:
• Asymptomatic vertebral Angioma : Signal fat (hyperintense T1hypointense T1FAT SAT)
• Symptomatic and compressive vertebral angioma : hypointense T1,
hyperintense T2 and intensely enhanced,
soft tissue reached.
Clinical forms:
• Angiomatosis and lymphangiomatosis: <30 years,
2 H / 1 F,
bone and visceral hemangiomas (liver,
spleen,
lungs,brain,
soft tissue).
Clinical presentation: masses,
hepato splenomegaly,
pleural and pericardial effusions,
cardiac and respiratory failure,
anemia,
DIC.
X-RAY:multiple geographic osteolysis,
surrounded by a thin dense border,blowing the cortex.
Sometimes soft tissue phleboliths or abnormalities of the lymphatic system.
CT: liquid density.
MRI: fluid signal (serous) or fat (lymph).
• Massive Osteolysis: Gorham’s disease : in children and young adults,
reaching two adjacent bones,
in belts or spine.
Osteolysis progresses to "ghost"bone.
Treatment: unnecessary unless the lesion is symptomatic
V-Cell round lesion : Eosinophilic granuloma(EG)
Definition: It is a non-neoplastic proliferation of histiocytes,
known as part of a spectrum of Langerhans cell histiocytosis formerly known as histiocytosis X.
EG is usually monostotic,
but can be polyostotic.
Topography: EG is found in the skull,
mandible,
spine and long bones.
Sex ratio: The male to female ratio is two to one.
Age: It occurs most commonly in children aged 5 to 10.
Clinical presentation: EG is normally symptomatic made of Local pain,
swelling and the ESR may be elevated.
X-Ray Appearance(Fig. 31): It is non-specific and differs by location.
The skull may have a lesion with sharp,
punched out borders that is uneven across the inner and outer table causing a "beveled edge".
Pelvic lesions are often poorly defined.
Spine lesions are normally found in the vertebral body.
EG is found in the diaphysis or metaphysis of long bones in the center of the medullary cavity.
The lesion may cause endosteal scalloping or a periosteal reaction.
CT scan and MRI delineate the extent of the intramedullary and cortical penetration.
Differential Diagnosis: EG should be included in the differential diagnosis of any sclerotic or osteolytic lesion,
either well-defined or ill-defined,
in patients under the age of 30,
includes Ewing's sarcoma,
osteosarcoma,
metastases and osteomyelitis.
The diagnosis EG can be excluded in age > 30.
Clinical forms:
-Letterer-Siwe disease is a fulminant systemic disease that comprises 10% of Langerhan's cell histiocytosis,
occurs in children under 3 years old and is rapidly fatal.
-Hand-Schuller-Christian disease (HSC) is a chronic disseminated form of Langerhan' s histiocytosis and occurs in older patients.
The well known triad of HSC is diabetes insipidus,
exopthalmos and skull lesions.
-EG can convert to systemic forms of the disease.
It makes up 60-80% of all cases of Langerhan's cell histiocytosis.
Treatment options: depends on the form of the disease:
-With localized disease,
often a biopsy alone is enough to incite healing.
-Other treatment modalities of EG include curettage,
excision,
steroid injection,
radiation and observation.
-Chemotherapy is recommended for systemic disease.
VI-Others:
VI-1.Solitary bone cyst:
Definition : Solitary bone cyst,
also known as unicameral bone cyst,
is a true cyst,
a fluid filled cavity lined by a thin membrane
Frequency: 3% of primary bone tumors.
The most frequent peripheral benign bone tumor in children.
Age: from 5 to 20 years,
Sex ratio: 3H/1F
Clinical presentation: asymptomatic
Topography(Fig. 32): metaphysis of long bones mainly proximal humerus and femur but also tibia,
calcaneum and pelvis in adults.
SBC may migrate from metaphysis to diaphysis during growth of the bone.
Conventional radiography: geographic osteolysis well defined inferiorly,
blowhole cortical or partitions may be seen.
When a fracture leads to diagnose the osteolysis,
a fallen fragment is appreciated and allows to affirm the fluid contents.
In case of fracture a periosteal reaction is also seen.
CT scan: only if uncertain diagnosis.
Liquid density,
air density in case of pneumatocyst
Complications:
Fracture (no delay for consolidation,
multilocular cyst)
Clinical forms:
-epiphyseal
-coralliform calcification
-pneumatocyst
Differential diagnosis:
Differential diagnosis: Aneurysmal bone cyst,
Fibrous Dysplasia when cystic.
Usually less expansion compared with ABC.
Treatment options:
-asymptomatic : Abstention
-Fracture: plaster
-To actif cyst (metaphyseal) in worrisome location(femoral neck): percutaneous injection of corticosteroid
VI-2.Aneurysmal cyst:
Definition: solitary expansile well-defined osteolytic bone lesion,
that is filled with blood.
It is named aneurysmal because it is expansile is thought to be the result of a reactive process secondary to trauma or increased venous pressure.
frequency : 10% of benign bone tumors
Age: under 20years ,
sex ratio : H /F=1/1 to 1/1.3
Clinical presentation : local pain and swelling,
pathologic fractures in up to 25% of cases spinal lesions can be associated with spinal cord compression or painful scoliosis.
Topography(Fig. 33): metaphysis of long bones : femur,tibia,fibula,
humerus and posterior arch of spine,
pelvis
Conventional radiography: an eccentric radiolucency and a purely lytic or,
occasionally,
trabecular process,
with its epicenter in the metaphysis of an unfused long bone.
The trabeculae in the cyst may create a soap-bubble appearance in the lesion.The margins of the lesion are well defined,
with a smooth inner margin and a rim of bone sclerosis.The expansion or ballooning of the cortex occasionally may result in the loss of the sharp definition of its margin.
In this case,
the finding should correctly be interpreted as an aggressive lesion rather than as solely diagnostic of malignant change.
No periosteal reaction occurs,
except when the periosteum is fractured.
CT: It can demonstrate the intraosseous and extraosseous extents of the lesion.
CT can be used to appreciate the cortex (destructed or thin),
to determine the nature of the matrix of the tumor.
Fluid-fluid levels may be seen in the cysts.
Fluid levels are depicted only when the patient is lying motionless for about 10 minutes and when the scans are obtained in the plane perpendicular to that of the fluid levels.
MRI: T1-weighted images show low to intermediate signal intensity with or without fluid levels.
Acute hemorrhage into the cyst may have high signal intensity.
T2-weighted images show areas of low to intermediate signal intensity or some areas of heterogeneous high signal intensity,
depending on the contents of the cyst.
A rim of low signal intensity with internal septa may produce a multicystic appearance.
Tumor enhancement with gadolinium is seen in aggressive lesions
Clinical forms:
-aggressive ABC: cortical destruction,
extension to soft tissues
-underlying lesion like GCT,
osteoblastoma or chondroblastoma.
Differential diagnosis :
-malignant lesions in some locations: It may mimic a sarcoma in the ribs,
scapula,
or sternum,
especially when associated with a large soft-tissue component .
-Fluid-fluid levels also are seen in giant cell tumors,
and in telangiectatic osteosarcomas.
Treatment options:
-Biopsy to llok for an underlying lesion
-Surgery
-Percutanous injection of Ethibloc or Embolisation
VI-3.Giant cell tumor:
Definition : tumor made up of mononuclear stromal cells and multinucleated giant cells.
The risk of malignant transformation in fibro or osteosarcoma is 10 to 20% after several local recurrence.
Frequency : 21% of benign bone tumors.
Age from 20 to 40 years,
Sex: Female > male.
Clinical presentation: Dull pain,
swelling,
pathologic fracture.
Topography(Fig. 34): Epiphyso-metaphyseal bone near the knee,
below the elbow.
Upper limb > lower limb.
Pelvis (near the joints),
sacrum,
vertebral body.
X-ray appearance (Fig. 35): metaphyseal-epiphyseal eccentric osteolysis,
containing shear walls,
blowing the cortex .
Sometimes achieving the adjacent epiphysis.
Sometimes,
signs of aggressiveness: ill-defined osteolysis,
cortical disruption,
extension to soft tissue (sign malignant degeneration or high risk of local recurrence) .
CT: Thecortex is blown or broken; partitions should not be confused with calcifications,
sometimes sero-bloody level.
MRI: Indispensable if the tumor is aggressive: to search intramedullary extension and in soft tissues.
Hypointense T1,
hyperintense T2,
sometimes liquid level.(Fig. 36)
Clinical forms:
- Multiple achieving: simultaneously or successively (hands,
metaphysis).
- TCG of Paget's disease.
Differential diagnosis:
-ABC may have the same radiographic features but is found in a younger age group.
-Chondroblastoma is also located in the epiphysis,
but is seen exclusively in the epiphysis without extention to the metaphysis and is seen in a younger age group.
-Metastases,
especially in older patients
What to do:
- If low-grade tumors: curettage + filling,
- If radiographically aggressive tumor or early aggressive recurrence after curettage: resection and reconstruction.
Evolution:
1 - Healing: After curettage,
even after one or two recurrences.
2 - Recurrence: 35 - 60%,
average time £ 6 years.
Radiography: gap adjacent to curettage,
delayed assimilation of a bone graft.
3 - Malignant degeneration: 10-20%,
usually after several recurrences,
average time: 13 years Radiography: signs of aggression: cortical disruption,
spicular periosteal reaction,
spur Codman,
invasion of soft tissues,
lung metastases.
VI-4.Lipoma:
Definition:Like soft tissue lipoma ,
it consists of mature fat cells separated into lobules by fibrovascular septa.
Frequency:Represents 0.3% of primary bone tumors biopsied.
Age:Occurs from 40 to 60 years,
Sex ratio: 1
Clinical presentation: asymptomatic,it is an incidental lesion.
Topography(Fig. 37): metaphysis,
sometimes diaphysis of long bones: fibula,
femur,
tibia: most frequent in lower limb than upper limb.
More rarely: calcaneus,
ribs,
skull,
spine (sacrum).
X-ray appearance : geographic osteolysis multilobed containing bony ridges,
surrounded by a thin border of condensation,
blowing the cortex and sometimes containing dystrophic calcifications.
CT: affirms thediagnosis: homogeneous fat content (negative density),
occupying the entire tumor.
MRI: fat signal (high signal T1,
T2,
disappearing in saturation fat).
Clinical form: Parosteal lipoma
asymptomatic mass with fat density coupled with a thickened and eroded cortical,
sometimes next to bony overgrowth.
Differential Diagnosis: unicameral bone cyst,
non-ossifying fibroma,
aneurysmal bone cyst,
chondrosarcoma,
fibrous dysplasia
What to do: if diagnosis affirmed by the scanner: abstension.
VI-5.Brown tumor:
Definition:It is a benign tumor occuring in hyperparathyroidism.
Topography: It can occur in any bone
Conventional radiography(Fig. 38): osteolytic lesion with sharp margins.Septa and ridges may be seen.
Differential diagnosis: ABC,
metastases and GCT depending on location and age.
The clinical and biological data have to be known for the diagnosis(renal failure++).