Gastrointestinal bleeding remains a frequent clinical dilemma,
often with poor outcomes despite multi-disciplinary treatment.
Multiple etiologies for NUGB have been described.
Peptic ulcer disease contributes to 50-75 % of the common causes of NUGB including duodenal ulcers,
gastric ulcers,
and erosive esophagitis/gastritis.
Fig. 1
Before the development of therapeutic endoscopy,
35-55 % of patients with massive NUBG required emergency surgery,
which was associated with a 20 % mortality.
With the development of therapeutic endoscopy,
emergency surgery is actually needed in only 5 % of cases because of massive hemorrhage or recurrent bleeding in the setting of endoscopic failure.
Many of these patients may have underlying conditions that can contribute to a poor outcome.
Before the advent of interventional endoscopy,
transcatheter arterial embolization was proposed as an alternative to surgery for the treatment of massive NUBG in patients with high surgical risk.
Since its introduction,
some authors have suggested this technique as rescue therapy after endoscopic treatment failure.
Fig. 2
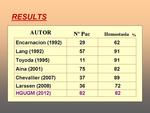
Transcatheter embolization are associated with a control rate of initial bleeding of 89-98% and clinical success rates ranging from 52-90% with most reports showing clinical successes of 70-80%.
Gomes et al.
had compared vasopressin infusion to embolization techniques and found the primary success rate with embolization therapy to be 71% and secondary success rate 88% compared with the primary success rate of 52% with vasoconstrictor infusion.
Fig. 9
While angiographic control of bleeding is achieved in a vast majority of patients,
less than 10% will develop recurrent bleeding.
Often these patients are amenable to angiographic reintervention.
More than half of the complications are considered minor.
Intestinal ischemia is usually transient,
requiring surgical intervention in less than 1%.
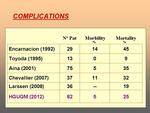
While the overall mortality of all patients with NUGB remains 6-10%,
the mortality rate for patients that require transcatheter embolization is 10-40%.
Clinical factors that predicted poor outcomes are multi-organ failure,
cirrhosis,
bleeding dyscrasia,
older age,
cancer,
and the recurrence of bleeding. Fig. 4
Lau et al.
presented a randomized,
controlled study showed no differences in bleeding control between a second endoscopic treatment and surgery after initial endoscopic treatment failure for bleeding peptic ulcers.
In our study (HGUGM),
surgery and embolotherapy,
two different therapeutic alternatives for bleeding peptic ulcers after endoscopic treatment failure,
were compared.
No differences were found in clinically relevant outcomes,
such as bleeding recurrence,
death,
and need for further surgery,
between patients who were treated with surgery versus embolotherapy.
Nevertheless,
patients who underwent embolotherapy were older and had more concomitant diseases,
especially heart disease,
two conditions related to a higher risk of bleeding recurrence and death.
There were also more patients who had received anticoagulant treatment,
which is associated with a higher risk of recurrent bleeding,
among those who had undergone embolization.
Despite the higher prevalence of these risk factors for poor outcome in the embolotherapy group,
no differences in outcomes were detected. Fig. 5