This poster was previously presented in Spanish at the 2012 Congreso Nacional SERAM (Granada)
Type:
Educational Exhibit
Keywords:
Interventional vascular, Gastrointestinal tract, Emergency, Catheter arteriography, Embolisation, Haemorrhage
Authors:
G. Rodriguez Rosales, M. Echenagusia Boyra, M. González Leyte, A. E. Madrid Vallenilla, N. Mimica Haasz, F. Camúñez Alonso; Madrid/ES
DOI:
10.1594/ecr2013/C-0740
Imaging findings OR Procedure details
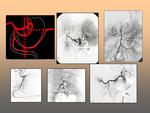
Angiographic technique for the diagnosis of NUBG requires selective angiograms of the celiac and superior mesenteric arteries.
A femoral approach is utilized to gain access to the arterial tree.
Embolotherapy is performed after diagnostic angiography even if no adtive bleeding is demosnstrated. A superselective angiogram of the left gastric artery is usually performed in cases in which bleeding is expected in the fundus of the stomach and superselective angiogram of the gastroduodenal artery is often performed in cases of suspected duodenal bleeding.
This technique provides a safe and thorough inspedtion of the mesenteric tree. Fig. 6
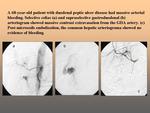
Direct angiographic signs of active GI bleeding include blood extravasation or intraluminal contrast pooling.
Blood extravasation is not always visualized.
In recent reviews of angiographic results,
blood extravasation or intraluminal blush was seen in 40-60 % of angiographic cases for NUGB.
Dempsey et al.
reported a similar rate of rebleeding when direct or indirect signs of bleeding were present during angiography.
Aina et al.confirmed Dempsey´s finding that early rebleeding and mortality was independent of direct or indirect angiographic findings.
In our experience,
no differences in outcomes were found (83% opposite to 50 %).
With a dual blood supply from the celiac and superior mesenteric arteries,
the upper GI tract tolerated embolization treatmente with less risk of intestinal ischemia compared with their lower GI counterparts.
And with new advances in hydrophilic,
steerable wires and microcatheters,
superselection and embolization in short segments of visceral arteries could be performed and were soon applied to the upper GI tract.
The review by Nicholson et al.
showed that the new embolization techniques were effective,
much safer,
and with fewer complications compared with tohose used in earlier series.
Similar series by Lang and Schenker et al.
showed that transcatheter embolization with microcatheters was beneficaial and safe when applied to the upper GI system.
Many embolization agents has likewise successfully including: particulate embolization such as polyvinyl alcohol particles or autologous clot,
coil/microcoil embolization,
Gelfoam embolization,
glue embolization such as N-butyl 2-cyanoacrylate.
Schenker et al.
found that none of the procedural variables,
including the type of embolization,
had a significant impact on clinical success.
Aina et al.
concluded that the use of coil embolization as a single therapy for NUGB was associated with a higher risk of early rebleeding.
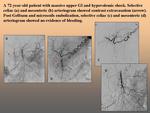
Although results have varied,
the combination of coils and embolic particles (“sandwiches”) has gained favour in controlling bleeding compared with single therapy.
The upper GI tract contains a rich collateral blood supply that ofter requires embolization of multiple arteries for successful outcomes.
Fig. 7 Fig. 8