Study Patients :
The records of 47 patients (30 men and 17 women) with 48 histologically proven RCCs were retrospectively analyzed.
One patient presented with two synchronous RCCs in the same kidney.
The mean age of patient population was 60 years,
with a range of 31-84 years.
The mean interval between CT examinations and surgery was less than two weeks.
Radical nephrectomy was performed in all cases.
Approval of this retrospective study was obtained from our institutional review board.
This study was complied with the Health Insurance Portability and Accountability Act.
Computed Tomographic examination :
All CT examinations were performed on a 16-row CT scanner with 24-mm scanning span per rotation.
Patient’s preparation included the administration of 1,000 ml of water,
given orally 30 minutes prior to the examinations.
In all patients,
unenhanced scanning and three contrast-enhanced series,
including arterial phase (scan delay: 25 seconds),
portal phase (scan delay: 70 seconds) and a combined nephrographic-excretory phase (scan delay: 4 minutes) were performed.
CT images were obtained in a craniocaudal direction,
covering the area of the kidneys (unenhanced scan and arterial phase),
the area from the diaphragm to the iliac crests (portal phase) and the area from the upper pole of the kidneys to the symhysis pubis (nephrographic-excretory phase).
For the acquisition of all images,
a slice thickness of 0.8 mm,
a tube voltage of 120 kV,
a rotation time of 0.5 sec and a pitch of 1.2 were used.
A detector collimation of 16 x 1.5 mm and 16 x 0.75 mm was used for unenhanced and contrast-enhanced series,
respectively.
Images were reconstructed at 5 mm and 0.5 mm intervals,
for unenhanced and post-contrast enhanced scans,
respectively.
Both dose modulation (DOM) and automatic current settings (DoseRight) were used,
and the mean mAs per rotation for each scan was calculated at 115.
Contrast-enhanced images were obtained after the intravenous administration of 150 ml of non-ionic iodinated contrast medium,
administered at a flow rate of 3 mL/sec,
via mechanical injector.
CT data interpretation :
Image interpretation was performed on a workstation.
The CT data were assessed by two reviewers in consensus,
blinded to clinical and histopathologic data.
Transverse unenhanced CT images and multiplanar reformations in the transverse,
coronal and sagittal planes,
separately for each contrast-enhanced series (arterial,
portal and nephrographic-excretory phase) were used for data interpretation.
Reformatted images were of 5 mm thickness,
with 0.5 mm slice intervals.
Both soft-tissue (W: 350,
L: 50) and wide window (W: 1500,
L: 500) settings were used to assess the data of the nephrographic-excretory phase.
Wide window settings have been reported to improve the conspicuity of pelvicaliceal details [29].
The number and size of RCCs were assessed and compared with the intraoperative and histopathologic findings.
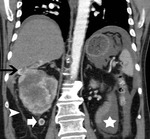
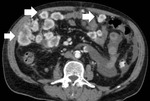
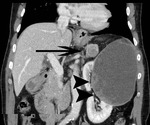
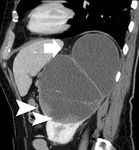
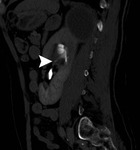
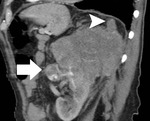
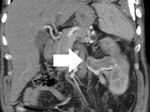
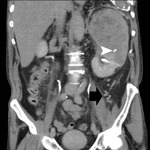
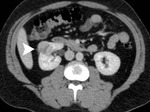
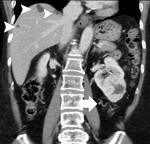
CT criteria used for the diagnosis of perinephric fat invasion included perinephric soft-tissue stranding,
peritumoral vascularity,
increased density of the perinephric fat,
tumoral margins and presence of contrast-enhancing soft-tissue nodules in the perinephric space (Fig. 1,
Fig. 2,
Fig. 3,
Fig. 4,
Fig. 5,
Fig. 6,
Fig. 7,
Fig. 8). Stranding of the perinephric fat was defined as linear areas of soft tissue attenuation,
corresponding to the bridging septa of the perinephric space (Fig. 9) [30,31].The bridging septa of the perinephric space of the contralateral kidney were used as the standard of reference (Fig. 10,
Fig. 11).
Presence of peritumoral vascularity was defined as asymmetrically enlarged,
often irregular vessels adjacent to the neoplasm,
within the perinephric space (Fig. 6,
Fig. 12) [21].
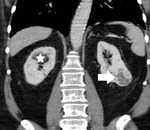
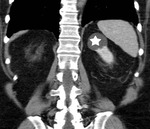
The CT density of the perinephric fat was measured by placing a circular region of interest (ROI),
as large as possible within the perirenal space,
close to RCC.
The CT density of the perinephric fat of the normal contralateral kidney,
measured at the area of the lower pole was used as the standard of reference (Fig. 3,
Fig. 4,
Fig. 5,
Fig. 6,
Fig. 7,
Fig. 8).
Three measurements were obtained and averaged.
Tumoral margins were evaluated and characterized as sharp or ill-defined.
A sharply-demarcated tumor was characterized as confined within the kidney (Fig. 10,
Fig. 11,
Fig. 12) and ill-defined margins as suggestive of neoplastic invasion of the PN fat (Fig. 1,
Fig. 2,
Fig. 6,
Fig. 7,
Fig. 8).
CT signs suggestive of neoplastic infiltration of renal sinus fat included tumor extension into the renal sinus,
proximity to the pelvicaliceal system and invasion of the pelvicaliceal system (Fig. 5, Fig. 8).
The final histopathologic diagnosis was used as the standard of reference.
Histopathologic data analysis
Histopathologic data used for the analysis was TNM stage,
histologic subtype,
Fuhrman nuclear grade,
tumor size and presence or absence of perinephric fat and/or renal sinus fat invasion.
The penetration of the renal capsule or the presence of neoplastic cells in direct contact with the perinephric fat was defined as PN fat invasion.
Direct contact of neoplastic cells with the renal sinus stroma or fat cells was defined as RS fat invasion.
Tumors infiltrating the pelvicaliceal system were characterized as infiltrating RS fat [10].
Statistical analysis :
Statistical analyses were performed using the IBM SPSS statistics,
version 20 and a two tailed value of p < 0.05 was considered statistically significant.
The normality of distribution of the CT density values of the perinephric fat was assessed using the Kolmogorov-Smirnov test.
Paired Samples T-test was used to assess whether the mean values of the CT density of the perinephric fat of the kidney with RCC and the normal contralateral kidney were statistically different from each other.
Independent samples T-test was used to study the differences between the mean CT density values of the perinephric fat of the diseased kidney in the presence or absence of PN fat invasion,
as confirmed on histopathology.
The Chi-square 2 way test was used to determine the significance of association between the various CT findings used to diagnose perinephric and/or renal sinus fat invasion.
Related descriptive statistical measures,
including accuracy,
sensitivity and specificity for each CT finding were also calculated.
Binary multiple logistic regression analysis (multi-step backward selection) was used to assess independent predictors of perinephric and/or renal sinus fat invasion among the various CT findings. Logistic regression analysis included coefficients,
standard errors (SEs),
adjusted odds ratios,
95% confidence intervals (CIs),
and the likelihood ratio chi-squared test for parameters in the final model obtained by maximum likelihood estimation.
Model fit was evaluated by the Hosmer-Lemeshow goodness-of-fit statistics.