The histologic subtypes of RCCs included clear cell RCC (n=33),
papillary RCC (n=2),
chromophobe RCC (n=5),
mixed RCC (clear cell and chromophobe,
n=1),
collecting duct carcinoma (n=1),
unclassified RCC (n=2),
multicystic RCC (n=3) and clear cell RCC,
with sarcomatoid differentiation (n=1).
Tumor grading included grade I in 3 (6%) tumors,
grade II in 26 (55%) tumors,
grade III in 15 (31%) tumors and grade IV in four (8 %) neoplasms.
Pathologic analysis revealed stage T1a in 17 (36%) tumors,
stage T1b in 13 (27%) tumors,
stage T3a in 16 (33%) neoplasms,
stage T3b in one (2%) case and stage T4 in one (2%) tumor.
Tumor size ranged from 1.2 to 15 cm,
with a mean maximal diameter of 5.1 cm; 44% (21 out of 48) of neoplasms measured equal or less than 4 cm,
on histopathology.
There were 12 (25 %) RCCs with peripheral perinephric fat invasion and 11 (23%) tumors with renal sinus fat invasion,
proved on pathologic analysis.
Among them,
seven (14.6%) neoplasms presented with PN fat invasion only,
six (12.5%) neoplasms with RS fat invasion only,
and five (10.4%) cases with infiltration of both PN and RS fat.
The size range of these RCCs varied from 2.4-15 cm,
and the mean size was 7.6 cm; 16 (89%) out of 18 neoplasms were larger than 4 cm in diameter.
Histologically,
11 (61.5%) RCCs with PN and/or RS fat invasion were of clear cell histology,
two (11%) of the papillary type,
two (11%) chomophobe RCCs,
one (5.5%) collective duct carcinoma,
one (5.5%) unclassified RCC and one (5.5%) multicystic RCC.
A low grade (grade II) was reported in 8 (44.5%) out of these 18 tumors and a high histologic grade was seen in 10 (55.5%) tumors (grade III,
n=7; grade IV,
n=3).
Tumor’s maximal diameter at CT varied from 1.4 to 15 cm,
with a mean diameter of 5.5 cm,
and this was in accordance with the pathology report.
Paired samples T-test showed a significant difference (p < 0.001) between the CT values of the perinephric fat in the vicinity of RCC (n=46),
compared to the CT density of the perinephric fat of the normal contralateral kidney (n=46).
The mean and standard deviation (SD) of the CT density of the perinephric fat of the diseased kidney and the contralateral kidney was -73 + 21 HU and -90 + 11 HU,
respectively.
Independent samples T-test showed that the mean CT density values of the perinephric fat close to RCC were significantly different (p =0.023) in cases of histologically proven PN fat infiltration (n= 12,
mean CT density measurement and SD: -61 + 18 HU) when compared to tumors without perinephric spread (n= 34,
mean CT density measurement and SD: -77 + 21 HU).
Two patients were excluded from CT density measurement analysis,
one case treated with radical nephrectomy for RCC years ago,
and another case with synchronous bilateral RCCs,
treated with radical nephrectomy and partial nephrectomy of the contralateral kidney.
The results of the Chi-square 2 way test in assessing the significance of association between the CT findings used to diagnose perinephric and/or renal sinus fat invasion are presented on Table 2.
Table 2. Results of the Chi-square 2 way test in assessing the association of CT findings with PN and RS fat invasion in patients with RCC (df: degrees of freedom).
|
CT findings
|
Chi-square value
|
df
|
P value
|
|
Perinephric fat invasion
|
|
|
|
|
perinephric stranding
peritumoral vessels
perinephric nodules
tumoral margins
|
3.361
3.367
16.111
16.456
|
1
1
1
1
|
0.067
0.067
< 0.001
< 0.001
|
|
Renal sinus fat invasion
|
|
|
|
|
extension into renal sinus
proximity to pelvicaliceal system
invasion of the pelvicaliceal system
|
2.039
2.436
33.061
|
1
1
1
|
0.153
0.119
< 0.001
|
The diagnostic performance of each CT finding in the detection of neoplastic infiltration of the PN and/or RS fat is illustrated on Table 3.
Table 3. Diagnostic performance of various CT findings in assessing PN and RS fat invasion in RCC.
|
CT findings
|
Sensitivity (%)
|
Specificity (%)
|
Accuracy (%)
|
|
Perinephric fat invasion
|
|
perinephric stranding
peritumoral vessels
perinephric nodules
tumoral margins
|
91.6
75.0
50
58.3
|
36.1
55.5
97.2
94.4
|
50.0
60.4
85.4
85.4
|
|
Renal sinus fat invasion
|
|
|
|
|
extension into renal sinus
proximity to pelvicaliceal system
invasion of the pelvicaliceal system
|
100
100
90.9
|
16.2
18.9
94.6
|
35.4
37.5
93.7
|
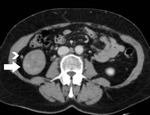
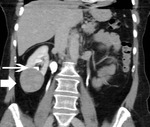
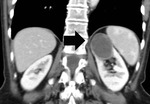
The presence of contrast-enhancing nodules in the perinephric fat (Fig. 1,
Fig. 2,
Fig. 3,
Fig. 4,
Fig. 5,
Fig. 6,
Fig. 7,
Fig. 8) proved accurate in 41 (85.4%) out of 48 RCCs in diagnosing the presence or absence of PN fat invasion,
with a significant difference.
In one false-positive,
an enhancing nodule was detected in the perinephric space close to RCC,
although the neoplasm was reported as confined within the kidney on the pathology report (Fig. 13,
Fig. 14).
Absence of perinephric nodules resulted in understaging of six RCCs in this report.
Tumoral margins proved accurate in 41 (85.4%) out of 48 cases in diagnosing extension of RCC into the perinephric space,
with a significant difference.
More specifically,
seven ill-defined RCCs proved histologically to infiltrate the PN fat (Fig. 1,
Fig. 2,
Fig. 6,
Fig. 7,
Fig. 8),
and 34 sharply-demarcated tumors (Fig. 10,
Fig. 11,
Fig. 12) found confined within the kidney on pathology.
In two false-positives,
RCCs with ill-defined margins reported negative for neoplastic infiltration of the PN fat on histology and in five false-negatives,
well-demarcated RCCs found to invade the perirenal fat histologically (Fig. 15).
Perinephric stranding and presence of peritumoral vessels enabled the diagnosis of PN fat invasion in 24 (50%) and 29 (60.4%) out of 48 tumors,
respectively,
and this was not proved significant.
Both CT findings although sensitive in diagnosing neoplastic infiltration of the perinephric fat,
had low specificities (36.1% and 55.5%,
respectively).
Twenty-three RCCs with thickened bridging septa in the perinephric fat and 16 tumors with peritumoral vessels were overstaged as T3a disease in the present study (Fig. 9,
Fig. 10,
Fig. 11,
Fig. 12).
Absence of perinephric stranding and collateral vessels resulted in understaging of one and three tumors,
respectively.
Invasion of the pelvicaliceal system proved accurate in 45 (93.7%) out of 48 RCCs in detecting the presence or absence of neoplastic involvement of renal sinus fat,
and this was proved significant (Fig. 5,
Fig. 8).
Extension of RCC into the renal sinus and proximity of the tumor to the pelvicaliceal system,
although sensitive in diagnosing infiltration of RS fat,
proved of low specificity (16.2% and 18.9%,
respectively,
Fig. 14 ).
Table 4 shows the results of multiple logistic regression analysis of CT criteria used to diagnose PN and/or RS fat invasion.
The most significant CT predictors in detecting perinephric fat invasion were the presence of contrast-enhancing nodules in the perinephric fat and tumoral margins.
Invasion of the pelvicaliceal system was the most significant predictor in the diagnosis of renal sinus fat invasion.
Table 4.Results of multivariate logistic regression analysis: independent predictors of CT findings in diagnosing perinephric and/or renal sinus fat invasion (PVC: pelvicaliceal system).
|
CT findings
|
Regression coefficient (SE)
|
Adjusted odds ratios
(95% CI)
|
Likelihood ratio test
|
Degrees of freedom
|
P value
|
|
PN fat invasion
neoplastic nodules
tumoral margins
|
2.65
(1.285)
-2.382(1.042)
|
14.16 (1.141-175.867)
0.92 (0.012- 0.712)
|
4.255
5.223
|
1
1
|
0.039
0.022
|
|
RS fat invasion
invasion of PVC
|
5.165(1.276)
|
175 (14.347-2134.534)
|
16.379
|
1
|
< 0.001
|