From February 2006 to January 2012,
46 lesions of the subclavian and innominate arteries were endovascularly treated in 46 patients (24 men [52,2%] and 22 women [47,8%]; mean age at intervention,
62 years [range,
45 to 74 years]).
All patients were symptomatic: 20 (43,5%) had vertebrobasilar ischemia,
17 (37,0%) had upper limb ischemia and 9 (19,6%) had both.
Thirty-seven stenoses (80,5%) and 9 occlusions (19,5%) were treated. Descriptive data on the patient cohort are listed in Table 1. Lesions were classified in 4 categories according to the document of the Standards of Practise Committee of the Society of Interventional Radiology (Table 2) (12).
Those categories were divided in two groups.
Patients with lesions classified in category 1 - stenoses shorter than 3 cm - were in the first group (28 patients,
60,9%) and in the second group were patients with lesions classified in categories 2,
3 and 4 – stenoses longer than 3 cm and occlusions (18 patients,
39,1%).
In 39 (92,9%) procedures stent was placed and in 3 (7,1%) cases only PTA was performed.
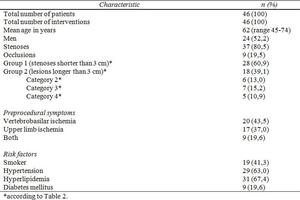
Table 1: Patients characteristics.
References: Radiology department, UKC Maribor - Maribor/SI

Table 2: Classification of the subclavian artery and innominate artery lesions (from Standards of Practice Committee of the Society of Interventional Radiology (12)).
References: Radiology department, UKC Maribor - Maribor/SI
All procedures were performed in an angiography suite with Axiom artis Siemens or Allura Xper FD 20 Philips.
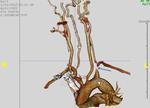
Computed tomography angiography (CTA) or digital subtraction angiography (DSA) was performed before procedures (Fig.
1).
Premedication was acetylsalicylic acid (100 mg per day) and clopidogrel (75 mg per day) for at least 3 days prior to the procedure.
Punction site was infiltrated with 1% lignocaine and arterial puncture was performed using Seldinger technic.
Transfemoral access was used in 38 procedures (82,6%).
Eight procedures (17,4%) were performed via combined access through femoral and brachial artery (Table 3).
After diagnostic aortic arch arteriography,
the target lesion was crossed with a hydrophilic 0.035-inch guidewire; heparin was administered during the procedure,
and the lesions were treated by means of angioplasty and/or stenting (Fig.
2).
If antegrade recanalization was unsuccessful,
retrograde attempt was made via brachial artery (Fig.
3).
The procedure was finished when anatomic success (brisk flow through the target lesion,
no evidence of thrombosis or dissection,
and less than 30% residual stenosis) was achieved.
Following the intervention,
aspirin has been continued indefinitely,
and clopidogrel was maintained for 6 weeks.
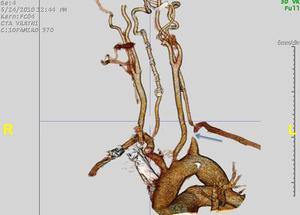
Fig. 1: CTA before procedure shows lesion of left subclavian artery (arrow).
References: Radiology department, UKC Maribor - Maribor/SI

Table 3: Procedural data for 46 interventions.
References: Radiology department, UKC Maribor - Maribor/SI
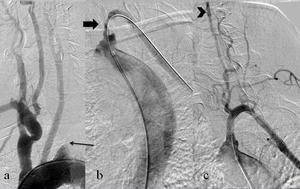
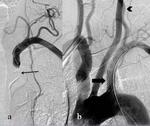
Fig. 2: Aortic arch angiography showed occlusion (thin arrow) of left subclavian artery (a). After antegrade recanalization with hydrophilic guidewire and predilatation (thick arrow) (b) stent was placed and antegrade vertebral flow achieved (arrowhead)(c).
References: Radiology department, UKC Maribor - Maribor/SI
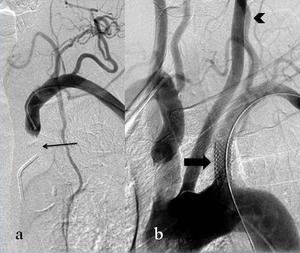
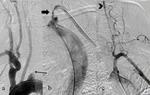
Fig. 3: In case of unsuccesful antegrade recanalization (thin arrow) retrograde attempt was made via brachial artery (a). Excellent technical success, including antegrade vertebral flow (arrowhead), was achieved after stent placement (thick arrow) (b).
References: Radiology department, UKC Maribor - Maribor/SI
Clinical success is defined as complete resolution of presenting symptoms.
Hemodynamic success is defined as improvement of the arterial pressure index by at least 0.15 (when compared with the normal contralateral arm) (2).
To be considered a late success,
the patient had to remain symptom-free,
and upper-extremity blood pressure had to remain normal or decrease by less than 0.15 (when compared with the contralateral arm).
Data regarding anatomic patency is not available,
because it is difficult to show those arteries noninvasively.
These criteria are consistent with adapted standards for reporting the results of surgical and percutaneous therapy for peripheral arterial disease (7,
13).