Keywords:
Vascular, Interventional vascular, Arteries / Aorta, MR-Angiography, CT-Angiography, Catheter arteriography, Stents, Recanalisation, Angioplasty, Obstruction / Occlusion, Dilatation
Authors:
B. Polanec1, S. Breznik2, A. Slanič3, J. Lučev3, J. Matela3; 1Pesnica/SI, 2Pernica /SI, 3Maribor/SI
DOI:
10.1594/ecr2013/C-1245
Results
Initial technical success was achieved in 42 (91,3%) of 46 procedures.
Four initial failures were due to inability to cross total occlusions.
That means that technical success in first and second group was 100% and 77%,
respectively.
The difference is statistically significant (Fischer's exact test; p=0,019).
Complications occurred in 5 of 46 procedures (10,9%).
Three access-site complications were hematomas (2 femoral and 1 brachial) and did not require operative repair.
Remaining 2 complications were embolisations from innominate artery to ipsilateral internal carotid artery and from left subclavian artery to brachial artery.
Former resulted in transient ischemic attack (TIA) without requirement for operative treatment and long-term consequence.
Latter required operative removal of thrombus which was not successful and ended in above-the-elbow amputation (Table 4).
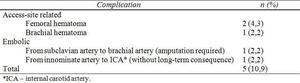

Table 4: Complications in 46 procedures.
References: Radiology department, UKC Maribor - Maribor/SI
Clinical follow-up is available for 39 (92,9%) of 42 patients,
at a mean time of 20 months (range,
4 to 45 months).
Three patients had recurrency of symptoms during follow-up,
therefore primary patency was 92,3%.
One patient had restenosis after PTA.
After second procedure stent was placed and the patient was symptom-free for at least 51 months.
Other 2 patients had in-stent restenosis which was treated with PTA.
Follow-up data after second intervention is not available.
Comparison of long-term follow-up in the two groups gave expected results.
Mean time follow-up in the group with stenoses shorter than 3 cm was 23 months (range,
6 to 45 months) and primary patency was 96,2%.
Patients with stenoses longer than 3 cm and occlusions had mean time follow-up of 12 months (range,
4 to 36 months) and primary patency was 84,6%.
Although the difference is not statistically significant (Mantel-Cox test; p=0,199),
the results are better in group 1.
Life-table data for the subclavian and innominate lesions,
including initial failures,
are presented in Fig.
4.
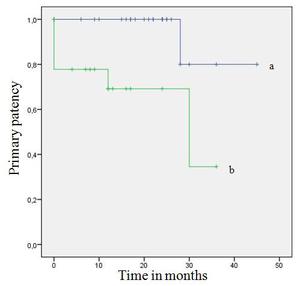
Fig. 4: Life-table data for the subclavian and innominate lesions, including initial failures, for both groups (a-group 1, b-group 2).
References: Radiology department, UKC Maribor - Maribor/SI





