Discussion
Contrast-enhanced CT has been essential in the assessment of the condition of AD,
which includes the extent of dissection,
blood flow of the true and false lumen,
location of entry or re-entry sites,
and circulatory impairment of abdominal organs.
However,
it is well known that there is a complicated motion of the intimal flap during cardiac pulsation,
which leads to the inaccurate estimation of the entry site and diameter of the true lumen using conventional CT.
Recent adaptation of ECG-gated CT has merits not only in eliminating the influence of motion artifact,
but also in offering 4D images which allows the assessment of the kinetics of the intima in AD.
Previous investigations for ADs using ECG-gated CT has been confined to the thoracic aorta (5-8); however recent advances in technologies regarding ECG-gated CT enabled us to obtain whole aortic volume data sets during one breath hold,
which allowed us to perform systemic analysis of the motion of intimal flap throughout the aorta.
Our study is the first investigation of the motion of the intima throughout the descending aorta in dissected cases.
Quantitative analysis of diameter change of the true lumen during the cardiac cycle revealed that the diameter of the true lumen in the proximal thoracic aorta reaches its peak in early cardiac cycle at around 30%.
There is then a gradual and delayed movement of the peak toward the distal abdominal aorta.
These results seem to be reasonable when we speculate the dynamic force of blood flow generated in systolic phase makes a wavelike pressure transfer in the true lumen of the dissected aorta.
Rmax of the true lumen gradually increased at levels lower than Th10,
which means diameter alteration of the true lumen during the cardiac cycle is measurable in the lower thoracic or abdominal aorta.
These results indicate conventional CT or prospective ECG-gated CT in certain phases may lead to inaccurate estimations of the diameter of the intima.
When we need to assess the diameter of the true lumen in the lower thoracic aorta as a distal landing zone for stent-graft placement,
the systolic phase was preferable since the largest diameter was given.
However,
in the assessment of true lumen collapse to predict malperfusion,
the diastolic phase in the lower thoracic aorta and the systolic phase in the abdominal aorta is desirable for accurate estimation.
These phenomena also explain the fact that malperfusion of the leg is more common than that of abdominal organs because perfusions were mainly achieved in the systolic phase,
wherein collapse of the true lumen of the abdominal aorta tends to occur.
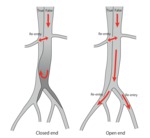
This study revealed the “closed end” false lumen in the distal dissected area could be a cause of true lumen collapse at the abdominal aorta (Fig. 11).
We may speculate the mechanism of the true lumen collapse is as follows. The pressure within the true or false lumen can dynamically divert during the cardiac cycle due to dynamic flows through the entry or re-entry sites and motion of the wall.
Communications between true and false lumen through re-entry sites has an effect of reducing the pressure difference between them,
which may lead to the relatively static state of the intima. Since the “closed end” false lumen in the abdominal aorta has no communication between the true and false lumen in the distal aorta,
the pressure of the false lumen in a certain cardiac phase does not escape,
which may result in the compression of the true lumen (Fig. 11,
Fig. 12, Fig. 13,
Fig. 14 and Fig. 15 )
This study also revealed that the duration from the onset of the dissection can be a factor of the stability of the intima.
According to our results,
the intimal motion is significantly less in the chronic phase when compared to the acute phase especially in the abdominal aorta. However,
we found no significant difference in the motion of the intima in other parts of the aorta.
While further studies with larger populations are needed,
using this method will help to evaluate intra-aortic hemodynamics and lumen behavior with dissection.
Summary of Discussions
-
In the lower thoracic aorta,
the diastolic phase is better for the assessment in terms of stent-graft planning in distal landing,
while systolic phase is better for the prediction of malperfusion.
-
In the lower abdominal aorta,
wherein collapse of the true lumen can occur,
the late systolic phase is desirable for accurate estimation of malperfusion.
-
"Closed end" false lumen which has no communication between the true and false lumen in the distal aorta can easily compresses true lumen and lead to the collapse of the true lumen.
Conclusion
We characterized the complicated and dynamic motion of the intima in the whole aorta in AD using retrospective ECG-gated CT.
The location of the re-entry sites,
extent of the dissection and duration from the onset can substantially affect the wall motion and could be a clue for comprehending the kinetics of the intima.
Furthermore,
precise and adequate evaluation using retrospective ECG-gated CT could help in determining treatment strategies for AD.