Entry sites were located in zones 3 (n=2),
Th4 (n=5),
Th5 (n=3),
Th6 (n=1),
Th7 (n=3),
Th8 (n=2),
and L1 (n=1).
Single or multiple re-entry was detected in 15 cases while two cases had no re-entry.
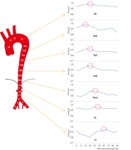
The color map explaining the site locations of entry or re-entries in each case is shown in Fig. 4.
Quantitative analysis of the diameter of the true lumen
The average diameter of a true lumen during the cardiac cycle at every zone2 level of the aorta was shown in Fig. 5 .
While the size of the true lumen in the proximal thoracic aorta reaches its peak during the early systolic phase,
the maximum diameter in lower thoracic or abdominal appears in the later cardiac phase.
Then,
A gradual and delayed wavelike movement of the peak toward the distal abdominal aorta is observed.
The greatest Rmax ,which was 34% on average (range 3-79%),
was frequently observed at the level of the lower thoracic aorta or abdominal aorta (Fig. 6).
The Dmin was 11.3mm on average (range 2.3-27.5mm),
and was frequently seen at the L3 level (Fig. 7).
In the assessment of the images,
collapse of the true lumen in the abdominal part was frequently seen in cases having no re-entry sites that were lower than L3.
Therefore,
we classified the 12 cases with AD at the L3 level into the following two groups based on the status of the false lumen:
- Closed end group: Cases without re-entry sites lower than L3 and thus having dead-end false lumen at the lower abdomen or iliac arteries
- Open end group: Cases with single or multiple re-entry sites lower than L3 and thus having open false lumen at the lower abdomen or iliac arteries
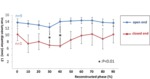
Diameter change in each cardiac phase for each group was shown in Fig. 8 and Fig. 9,
which reveals that the “closed end” group showed collapse of the true lumen at the early systolic phase while the “open end” group showed relatively stable diameter change.
Differences of the Rmax in terms of duration from the onset
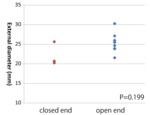
The comparison of the Rmax between acute and chronic phases is presented in Fig. 10.
At the L3 level,
acute aortic dissections have a significantly higher Rmax than chronic aortic dissections.