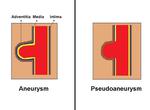
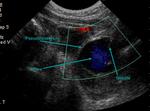
A pseudoaneurysm (PSA) is a common vascular injury that represents a rupture of the arterial wall contained in a defined sac of turbulent flow,
with a persistent connection (neck) to the artery. Arterial disruption is usually secondary to trauma,
inflammation/infection or iatrogenic causes.
They are in contrast to true aneurysms,
which have all three layers of intima,
media and adventitia that form the normal arterial wall,
with arteriosclerosis being the primary factor in their development.
Following injury of the arterial wall,
under the influence of sustained arterial pressure,
the blood dissects into the tissues around the damaged artery and forms a perfused sac.
The PSA is contained by the media or adventitia or simply by soft-tissue structures (Fig.
1).
PSA differs from active extravasation of blood.
In PSA blood inside the sac recirculates inside the artery,
while in the active bleeding it does not [3].
The etiology of the PSA is important for treatment planning and follow-up; they appear as a consequence of an injury of the vessel wall,
but there are multiple etiologies [4]:
- Blunt and penetrating trauma: gunshot wounds (especially in subacute cases by the expansive wave).
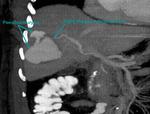
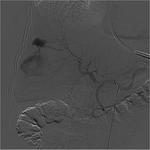
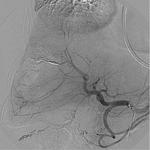
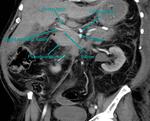
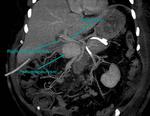
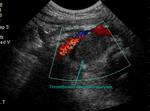
- Infection (Fig.
2,
3 and 4).
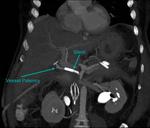
- Inflammatory condition: for example the extravasation of pancreatic enzymes (Fig.
5,
6 and 7).
- Multisystemic disease: Behçet disease.
- Benign and malignant tumor: invasion and erosion of arterial wall by the tumor (renal angiomyolipoma,
osteochondroma,
choriocarcinoma and lymphoma).
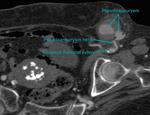
- Iatrogenic causes (Fig 8,
9,
10 and 11):
- Surgery.
- Suture failure in transplant patients.
- Percutaneous biopsy or drainage.
- Obstetric procedures: curettage and cesarean section.
- Intravenous drug abusers.
A PSA may appear in any vessel,
and its location will depend on the area where the injury is produced.
Pseudoaneurysms are becoming more present in radiological studies due to:
1.
The increase in the number of surgical and arteriographic invasive procedures with the use of large vascular introducer sheaths and periprocedural anticoagulation.
2.
The improvement of sensitivity of modern imaging techniques.
Clinically a pseudoaneurysm may be silent and detected only incidentally during radiologic investigation of other conditions.
It can manifest as a palpable thrill,
audible bruit or pulsatile mass.
But it also may present with local or systemic signs and symptoms.
Local effects are secondary to mass effect of the sac on adjacent structures:
- Ischemia of the surrounding tissues due to vascular compromise can produce necrosis of the skin and subcutaneous tissue [4].
- Neurologic symptoms may develop secondary to nerve compression or ischemia.
- Compression of adjacent veins may lead to edema and deep venous thrombosis.
B) The systemic features include distal ischemia,
embolization or sepsis.
The most feared complication is the rupture,
which can have catastrophic consequences.
Pseudoaneurysms can communicate into the gut,
the biliary system,
and the thoracic,
peritoneal,
pelvic and retroperitoneal spaces,
depending on its location.
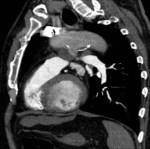
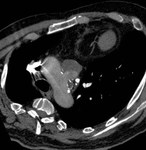
CT angiography,
especially with the advent of multi-detector row helical CT scanners,
has several advantages compared to other imaging modalities: it is not operator dependent,
has a shorter acquisition time and provides an overview of the entire vasculature.
Furthermore,
CT can help detect associated injuries or other associated disease entities such as pancreatitis that may not be detected with other modalities.
Three-dimensional CT allows visualization of the lesion in different angles and provides a global perspective of the entire vasculature,
including adjacent vascular beds.
CT helps in planning endovascular treatment before invasive angiography to ensure a one-step treatment option.
It allows a faster and more efficient therapeutic angiography and avoids increasing of irradiation and contrast dose,
since it helps us to choose the proper projection during the process.
The usefulness of CT is still limited by imaging artifacts caused by metallic objects.
It is also limited (like the rest of the imaging techniques) to distinguish between PSA and saccular true aneurysms if there is not a known history of injury of the vessel (Fig.
12 and 13).
Currently,
the use of CT angiography is the first line imaging investigation in patients with suspected arterial injury.
CT angiography had a sensitivity and specificity of 95.1% and 98.7% respectively,
in detecting traumatic pseudoaneurysms in the proximal extremites [5].
It is generally agreed that symptomatic PSA should be treated; however,
the decision to treat asymptomatic PSA is controversial because there is no proven method to date to determine which pseudoaneurysm will spontaneously thrombose or which will bleed [5].
The location of PSA may affect its handling.
The risk of rupture of visceral PSA is very high regardless of their size,
so definitive treatment should be performed in those cases.
Some investigators recommend observing the small,
asymptomatic non-visceral PSA and treating them only if they enlarge,
do not resolve,
or become symptomatic [4].
The treatment of pseudoaneurysms include surgery,
US-guided compression,
US- guided percutaneous thrombin injection,
transcatheter arterial embolization with a variety of agents (coils,
glue,
Gelfoam and sclerosing agents),
endovascular covered stent insertion and combination of methods for complex cases.
The therapeutic options should be chosen depending on their location,
morphological features,
rupture risk and clinical setting of the pseudoaneurysm as well as to patient comorbidities.