A retrospective review of all PSA detected in our radiology department from January 2011 to April 2012 was performed. All patients were evaluated by computed tomography.
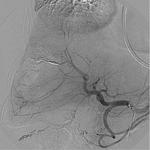
In some cases arteriography was available.
A multi-detector helical (16-slice) CT scanner was used to perform exams.
Our protocol included an axial non-contrast-enhanced CT scan and image acquisition after intravenous contrast,
completed with MPR and 3D reconstructions.
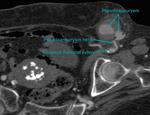
Unenhanced CT scans usually demonstrated a low-attenuation rounded structure arising from the side of the donor artery.
The wall of the pseudoaneurysm is usually smooth and well delineated except in a mycotic pseudoaneurysm,
whose wall is thickened,
irregular or ill-defined.
There may be a surrounding area of heterogeneous or even high attenuation if the pseudoaneurysm has ruptured and developed a hematoma.
After intravenous contrast administration and image acquisition in the arterial phase,
a pseudoaneurysm is confirmed because contrast material fills the sac to the same attenuation as the parent artery.
However,
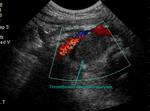
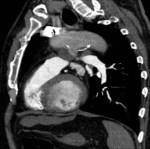
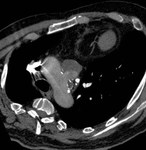
if the entire PSA does not fill with contrast material and low attenuation area remains within the sac a partial thrombosis is suspected (Fig.
12 and 13).
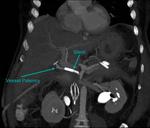
The donor artery is adjacent to the PSA,
and often the neck (area of communication between the sac and donor artery) can be seen and measured (Fig.
8 and 9).
The rupture of the PSA is noted as extravasation of contrast that is not contained within a round structure and often flows away from the point of injury.
On delayed images,
there will be washout of the contrast in the pseudoaneurysm,
whereas in extravasation it will persist in soft tissues.
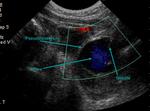
Size and location of the pseudoaneurysm provide important information about the risk of complications.
Length and width of the neck,
expendability of the donor artery and presence of collateral circulation are essential features in order to perform treatment planning (Fig.
8 and 9).
For example for superficial PSA with a narrow neck,
thrombin injection is considered the first line management option (Fig.
10 and 11).
If the sac is in a deep territory,
endovascular treatment is advised.
If the PSA arises from an expandable artery,
it can be embolized (Fig.
4). If the artery is not expandable,
the PSA neck must be evaluated. If it is narrow,
sac embolization is performed (usually with coils).
On the other hand,
if the neck is wide,
covered stent deployment (Fig.
7) or remodeling with stent or balloon are the options to be considered.
Surgery still plays a role when minimally invasive techniques cannot be performed or in infected PSAs.