A retrospective review of patients who were treated with endovascular therapy for CMI between July 2005 and November 2011 at a single institution was performed.
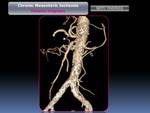
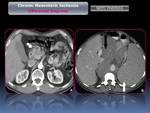
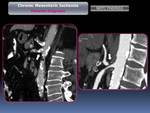
Inclusion criteria were clinical and radiological findings consistent with CMI who underwent endovascular therapy (Fig. 2).
Exclusion criteria were: incidental mesenteric artery stenosis without symptoms,
prior open surgical revascularization of a mesenteric artery for CMI and acute mesenteric ischemia.
Patients Diagnosis:
We obtained a non-invasive imaging in patients who had clinical symptoms of CMI (postprandial pain,
generally epigastric or periumbilical,
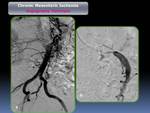
fear of eating and history of vascular disease) to confirm the suspicious, using 64 or 16 multidetector computed tomography (MDCT) obtained on arterial phase with the purpose of evaluate the presence of collateral vessels (Fig. 3), the shape and appearance of the atheroma plaques (calcified,
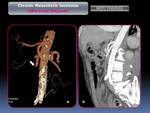
hypodense or heterogeneous) (Fig. 4),
the stenosis degree,
and other causes of abdominal symptoms like abdominal neoplasic,
inflammatory and vascular disease (Fig. 5 and Fig. 6).
In case of stenosis or occlusion of two or more visceral trunks they were proposed to perform an angiography.
Angiographic technique:
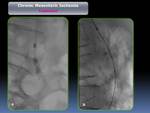
Non selective abdominal angiography and selective visceral angiography was performed to confirm MDCT findings and to select the most appropriate therapeutic option (Fig. 7).
Selective catheterization of each mesenteric arteries was necessary to measure luminal narrowing and assess the downstream bed and collateral flow.
When one of the arteries was completely occluded,
catheterization of one or both of the other arteries was used to determine whether recanalization is feasible.
Techniques of PTA:
All 11 procedures were performed by axillary approach due to there is a slight advantage in cases of acute angulation at the mesenteric vessel arisen of the aorta.
A non selective catheter (pig-tail) was advanced through the sheath into the abdominal aorta,
and a diagnostic angiogram was performed in posterior-anterior and lateral projections.
Catheterization of the selected vessels to treat was made using a selective catheter (multipourpose,
cobra or shepherd-hook).
Intra-arterial heparin (50 UI/Kg) and nitroglycerine (100-200 µg) was injected as soon as selective catheterization had started,
to reduce the risk of thrombosis and vasospasm.
Indications of treatment:
Indications for stent placement were: calcified ostial or high-grade eccentric stenosis and chronic occlusions.
Two types of stents were used in endovascular treatment of CMI: auto-expandable stents and balloon-expandable stents,
the last one offers additional precise placements.
Placement with 1- to 2-mm protrusion into the aortic lumen is recommended (Fig. 8).
The goals of treatment were to ensure symptom resolution,
to correct nutritional status and to prevent intestinal infarction.
The decision to perform open surgery versus angioplasty and/or stenting was based upon the patient's age,
comorbidities,
the number and severity of occluded vessels,
and the ease of vascular access to the stenosed vessels.
Follow-up:
Follow-up was performed by review of patient medical records and imaging reports.
Technical success was defined as the successful revascularization of all arteries that were treated in which there was less than 30% residual stenosis and clinical success was defined as complete resolution of symptoms; restenosis rates,
need for re-intervention,
and mortality rates was evaluated after the procedure to demonstrated high procedural success rates.
Patient's symptoms,
number of arteries and total treated occlusions,
access site and devices used,
procedural success,
complications,
and clinical and imaging follow-up were assessed.