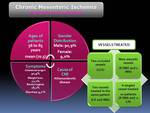
Patient demographics (Table 1):
The endovascular procedures were realized in 3 celiac arteries (CA),
8 superior mesenteric arteries (SMA) and 1 inferior messenteric artery (IMA) in 11 patients.
Most of patients with CMI were older than 55 years.
The ages of the patients ranged from 56 to 85 years (mean 70.5).
The gender distribution was: ten male (90.9%) and one female (9.0%).
Abdominal angor was the most frequent symptom in our data (90.9%) followed by weight loss (27.2%).
Others unespecific symptoms like rectorraghia (18.2%) and diarrhea (9.0%) were reported in three patients.
Atherosclerotic disease was the main cause of mesenteric ischemia in the 100% of patients.
With regard to the number of treated vessels,
the results were: two occluded vessels,
endovascular treatment was performed in the remaining stenotic vessel (2 SMA occluded and 2 CA treated) and nine stenotic vessels (8 SMA,
1 IMA) which were successfully treated.
In one patient two arteries were treated at the same time (CA and IMA).
At the remaining ten patients,
a single artery was treated (Fig. 9).
Technical success rates:
Complete procedural (per patient) technical success was achieved in 11 patients (100%).
Clinical success rates:
There were 11 complete clinical successes,
with immediate clinical improvement in all patients.
Procedural details:
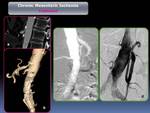
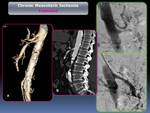
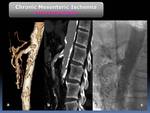
All patients with suspected CMI were evaluated using 64 or 16 MDCT on arterial phase. In all cases there was a good correlation between the CT findings with respect to the angiographic findings regarding the evaluation of the degree of stenosis and / or presence of arterial occlusion (Fig. 10 and Fig. 11).
All endovascular procedures performed were technically successful in our data.
We have used balloon-expandable stents in 6 patients and auto-expandable stents in 5 patients.
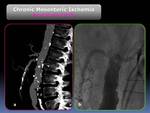
The six patients to whom they procedure was balloon-expandable stenting were followed by PTA (Table 1) (Fig. 12 and Fig. 13).
Complications were not reported in our series.
Follow-up:
During the follow-up period,
four patients (36.3%) died of unrelated causes to CMI.
All living patients were asymptomatic at the time of collection of information (Table 1).