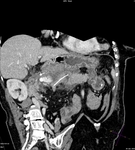
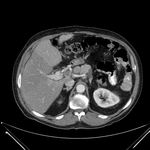
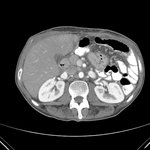
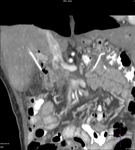
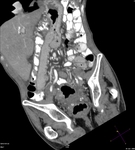
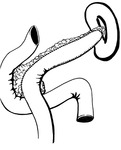
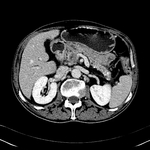
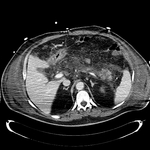
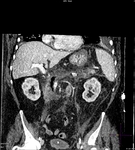
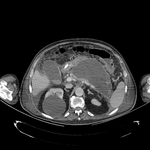
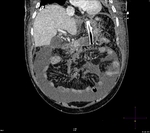
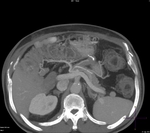
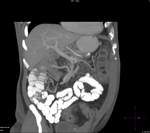
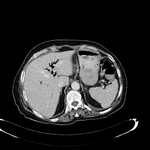
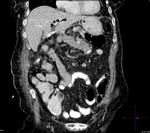
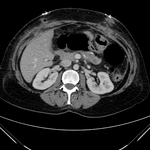
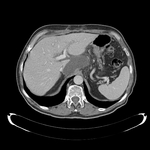
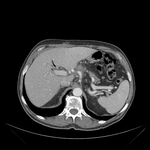
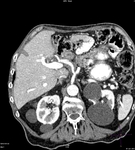
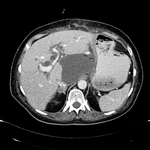
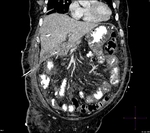
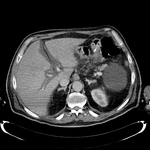
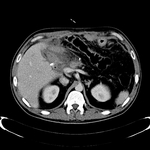
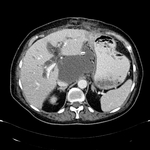
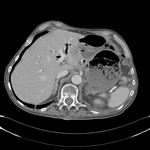
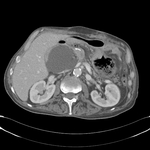
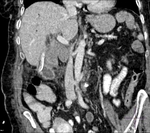
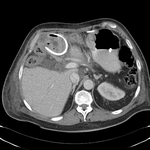
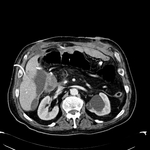
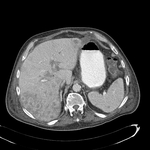
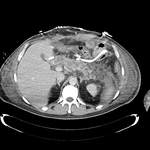
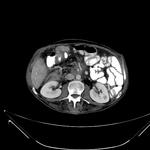
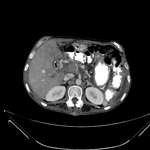
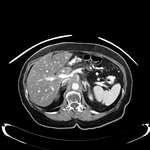
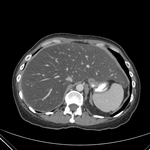
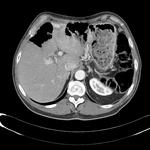
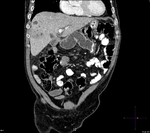
Pancreatic surgical procedures can be classified as either resection or drainage procedures.
1.-PANCREATIC SURGICAL PROCEDURES:
Pancreatic resection,
mostly performed to remove pancreatic tumors,
provides the only option leading to long-term survival or even to cure in pancreatic neoplasms.
The resection procedures registered in our hospital in the las four years include:
- Pancreatoduodenectomy (Whipple procedure)
- Central pancreatectomy.
- Distal pancreatectomy.
- Total pancreatectomy.
2.- DRAINAGE PROCEDURE:
There is another group of procedures which are usually performed to treat chronic pancreatitis,
also named drainage procedure,
and include the Puestow and Frey Procedure.
In our hospital Frey Procedure is the only drainage procedure performed in the last four years.
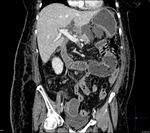
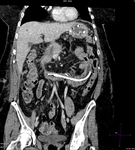
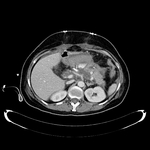
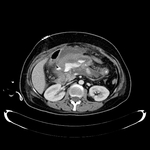
Fig. 1
3.- MISCELLANEOUS PROCEDURES:
- Necrosectomy
- Pseudocyst Derivation
1.1 PANCREATODUODENECTOMY.
WHIPPLE PROCEDURE
Pancreatoduodenectomy is indicated for treatment of tumors in the periampullary region (cancer in the head of pancreas,
the ampulla of Vater,
the distal bile duct,
and the duodenum).
The procedure consists of resection of the pancreatic head,
gastric antrum,
proximal 20 cm of jejunum,
gallbladder,
distal common bile duct,
and lymph nodes,
followed by three anastomoses: pancreaticojejunostomy,
hepaticojejunostomy and gastrojejunostomy. Fig. 2
1.2 CENTRAL PANCREATECTOMY
Central pancreatectomy is usually indicated to resect benign or low malignant-potential lesions in the neck or body region of the pancreas. Fig. 3
This procedure consists of resection of part of the neck or body of the pancreas; the distal remmanent is anasatomosed to a Roux-en-Y pancreaticojejunostomy,
and the proximal cut (head remmanent) is sutured. Fig. 4 Fig. 5 Fig. 6
1.3 DISTAL PANCREATECTOMY
Distal pancreatectomy is performed to resect neoplastic lesions in the distal neck,
body,
or tail of the pancreas,
or lessions located to the left of the portal confluence.
The blood that supplies the pancreatic tails comes from branches of the splenic artery,
that is why in most of cases the distal pancreas is resected along with en bloc removal of the spleen.
However,
according to some reports in the literature,
if the lesion is thought to be of low malignant potential or if the distal pancreatectomy is performed to chronic pancreatitis ,
the spleen may be preserved. Fig. 8
1.4 TOTAL PANCREATECTOMY
Total pancreatectomy is indicated for a reduced range of neoplastic conditions (nesidioblastosis,
multicentric endocrine tumors,
multifocal intraductal papillary mucinous neoplasms),
chronic pancreatitis,
or for emergency indications such as perioperative complications after pancreatic resections.
Fig. 9 Fig. 10 Fig. 11
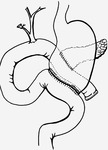
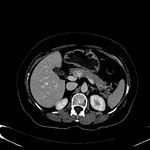
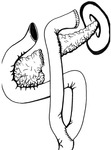
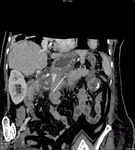
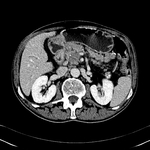
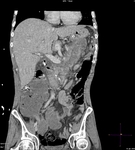
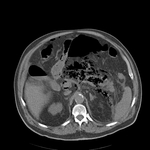
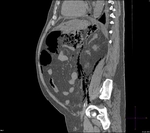
2.1 FREY PROCEDURE
Frey procedure is performed in chronic pancreatitis with head-dominant disease.
This procedure consists of a subtotal duodenal-preserving pancreatic head resection followed by a longitudinal incision of the pancreatic duct and a side-to-side Roux-en-Y retrocolic pancreaticojejunostomy.
Fig. 12 Fig. 13 Fig. 14 Fig. 15
3.
MISCELLANEOUS PROCEDURES:
- Necrosectomy.
The major risk factor for mortality in severe acute pacreatitis is the infected pancreatic necrosis; that is the reason why necrosectomy or abscess drainage is indicated in cases of severe acute pancreatitis with signs and symptoms of sepsis.
The evidence of gas bubbles in the peripancreatic fluid collections is very specific for infection,
although an enteric fistula should also be taken into account in the differential diagnosis.
Fig. 16 Fig. 17 Fig. 18 Fig. 19
- Pseudocyst Derivation. This procedure is usually indicated in patients with signs and symptoms of complications,
such as rupture,
obstruction,
secondary infection,
hemorrhage.
The procedure consist of creating a connection between the pseudocyst and the gastrointestinal tract,
either the stomach,
the duodenum,
or the jejunum. Fig. 20 Fig. 21
4.
NORMAL CT FINDINDS AFTER PANCREATIC SURGERY:
- Presence of unopacified anastomotic bowel loops in the porta hepatis.
It coulb be mistaken for fluid collections,
local recurrence,
lymphadenopathy...
Fig. 22
- Presence of metallic or opaque foreign bodies in the pancreatic surgical bed and in the anastomosis: clips,
stent across the pancreaticojejunal anastomosis and metal sutures in the anastomosis.
Fig. 23
- Pneumobilia.
Produced by the patency of the hepaticojejunostomy.
Fig. 24 Fig. 25
- Small amount of fluid and small transient fluid collections in the pancreatic surgical bed in the immediate perioperative period.
It is normal to find transient fluid collections in the surgical bed and at the sites of anastomoses during the early postoperative period (first two weeks). Fig. 26 Fig. 27 Fig. 27 Fig. 28
- Presence of soft tissue perivascular cuffing.
In the early postoperative period,
soft tissue stranding in the mesenteric fat of the surgical bed and soft tissue perivascular cuffing are indistinguishable from tumor recurrence.
These findings are likely inflammatory in patients with negative surgical margins and unlike tumor recurrence,
perioperative soft tissue perivascular cuffing undergoes a gradual decrease,
not increase.
By 3-6 months much of the inflammatory change surrounding the surgical bed should have resolved; however,
some mild induration in the surgical bed can persist indefinitely and in one series it was seen for a maximum duration of 13 months.
Some patients who undergo a pancreatic surgical procedure receive adjuvant chemotherapy and radiotion therapy,
which can result in stranding of the mesenteric fat within the radiation field.
Fig. 29 Fig. 30
5.
ACUTE SURGICAL COMPLICATIONS
- Leakage or fistula either from the pancraticojejunal anastomosis or from hepaticojejunal anastomosis.
The diagnosis of a leak is suggested by the presence of a focal fluid collection close to the anastomosis.
However,
it is difficult to confirm whether a leak arises from the pancreaticojejunostomy or from the hepaticojejunal anastomosis.
Leakage at the latter is suspected clinically if there is > 50 ml of bilious fluid in the drainage catheters after the fourth postoperative day.
Fig. 34 Fig. 35 Fig. 36 Fig. 38 Pancreaticojejunostomy leakage or pancreatic fistula is suspected if there is a volume of drainage with an amylase content >3 times the normal value for serum.
Development of a pancreatic fistula is associated with complications such as pancreatitis,
peripancreatic fluid collections (the presence of air bublles should raise concern abour pancreatic fistula),
abscess,
hemorrhage and sepsis.
Fig. 31 Fig. 32 Fig. 33
- Peripancreatic fluid collections. Fig. 39 Fig. 40
- Subhepatic abscess.
Intraabdominal abscesses can arise secondary to an underlying pancreatic fistula,
superinfection of an acute postoperative fluid collection,
or secondary to a leakage.
Fig. 41 Fig. 42 Fig. 43
- Peritoneal and hepatic candidiasis.
- Acute pancreatitis of the remnant.
Fig. 45
- Afferent loop syndrome.
This complication results from a mechanical obstruction of the afferent loop of a Billroth II loop gastrojejunostomy performed.
Although rare,
the afferent loop syndrome has been reported after other types of procedures,
such as Roux-en-Y reconstruction or Whipple procedure.
Fig. 46 Fig. 47
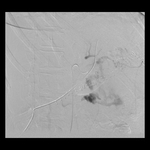
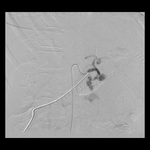
- Hemorrhage.
Early postoperative bleeding occurs within the first 24 h after surgery and often results from active bleeding at an artery stump at the surgical bed.
Late postoperative hemorrhage occurs after 5 days and it is normally secondary to a structural abnormality in the mesenteric vasculature.
Fig. 48 Fig. 49 Fig. 50 Fig. 51
- Thrombosis of mesenteric vessels.
Fig. 52
- Splenic Infarction.
Fig. 53
6.
LONGER-TERM LATE POSTSURGICAL COMPLICATIONS
- Tumor recurrence in the Surgical Bed.
The most frequent sites of recurrence pancreatic cancer are liver and pancreatic bed.
As mentioned before,
locally recurrent disease appears as a soft-tissue infiltrating mass int he surgical bed,
with perineural invasion and encasement of the mesenteric vessels,
which is difficult to differentiate from the postoperative inflammatory changes.
However,
an increase in the amount of soft tissue in the pancreatic bed or perivascular cuffing should be suggestive of recurrence.
Fig. 54 Fig. 55 Fig. 56
- Fatty infiltration of the liver. Many patients who undergo a pancreatic surgical procedure receive adjuvant chemotherapy and radiation therapy which can result in fatty infiltration of the liver.
Fig. 57
- Anastomotic strictures.
It is possibly one of the most delayed complication of the Whipple procedure; anasmotic stricture can be found either at the pancreaticojejunostomy or at the hepaticojejunostomy. Fig. 58 Fig. 59
- Thrombosis.