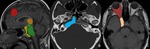
The neuroimaging of OP should include the whole efferent visual pathways,
from the cortical impulses to the orbit (Fig.
1).
We can schematically classify anatomical sites that could be involved in OP on the basis of the oculomotor cranial nerves’ nuclei into:
- supranuclear
- nuclear and internuclear
- infranuclear (cisternal,
skull base,
cavernous sinus,
orbit)
Generally speaking,
neuroimaging of OP rests on the use of CT and MR imaging techniques.
In selected cases conventional catheter digital subtraction angiography (DSA) is also necessary.
MR is the single most accurate imaging modality in the setting of OP.
Multiplanar images and different pulse sequences (T1-W,
T2-W,
FLAIR,
DWI,
3D-steady state free precession,
fat-saturated and post-contrast images) can demonstrate the underlying cause of OP.
Non-enhanced CT is the most common initial imaging examination in the emergency setting and can be a complementary tool to MR for the study of the osseous structures of the skull base.
Vascular imaging,
with MR-angiography (MRA),
CT-angiography (CTA),
or DSA,
is also used in selected cases.
Supranuclear OP: caused by lesions of different etiology involving cortical or subcortical frontal eye fields,
the thalami or the dorsal midbrain (pretectal area and superior colliculi).
While frontal eye fields,
located in the pre-frontal cortex,
initiate and control the contralateral gaze ocular movements,
dorsal midbrain controls vertical gaze and pupillary light reflex.
Moreover,
the thalami are important relays stations.
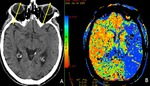
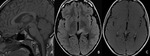
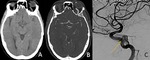
- Vascular diseases: ischemic strokes in the middle cerebral artery territory involving the frontal cortex can present acutely with a gaze preference towards the side of lesion (“right-way eyes” sign),
besides hemiparesis contralateral to the cortical lesions (Fig.
2) (3).
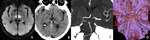
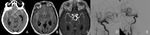
Acute ischemic or hemorrhagic lesions involving the thalami,
due to occlusion of the tip of the basilar artery (Fig.
3),
proximal posterior cerebral arteries,
or due to deep venous system thrombosis,
present with a complex constellation of symptoms and neurological signs (4).
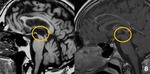
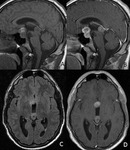
- Degenerative diseases: Progressive Supranuclear Palsy,
characterized by midbrain tegmentum atrophy,
downward gaze palsy ("surprised" look),
dysarthria,
parkinsonism and dementia.
Characteristics imaging findings include flattening or concavity of the normally convex superior profile of the midbrain,
dilation of the Sylvian aqueduct and relative increase in the length of interpeduncolar fossa (Fig.
4) (5).
- Metabolic-toxic diseases: Wernicke encephalopathy,
caused by thiamine deficiency and characterized by development of OP,
ataxia and acute confusion.
MR can demonstrate symmetrically increased T2 signal intensity in the mammillary bodies,
medial thalami,
tectal plate,
periaqueductal area (6).
- Compressive causes: compression of dorsal midbrain and pretectal area typically presents with upward gaze palsy,
convergence-retraction nystagmus and pupil light-near dissociation (pupils do not react to light,
but react to accomodation),
so called Parinaud’s syndrome.
It has been associated with different types of tumors,
such as pinealocytomas,
pinealoblastomas,
metastases,
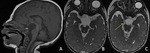
tectal gliomas and germ cells tumors (Fig.
5-6).
Also hydrocephalus (7) can determine a mass effect upon the tectum of the midbrain causing Parinaud’s syndrome.
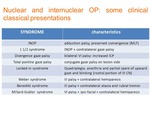
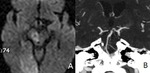
Nuclear and Internuclear OP: can be caused by lesions of the ventral midbrain and pons,
involving the nuclei of the cranial nerves III,
IV,
VI,
or the neuronal network connecting these nuclei,
such as the medial longitudinal fascicle (MLF) and paramedian pontine reticular formation (PPRF).
These structures are principally responsible for horizontal gaze and accommodation,
except for the CN IV,
whose dysfunction mainly causes vertical diplopia.
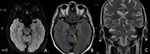
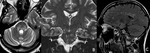
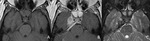
- Vascular diseases: ischemic infarcts in the territory of the basilar artery perforating branches,
with associated variable involvement of adjacent nervous structures (including cortico-spinal tracts and red nuclei) and consequent different clinical presentations (Fig.
7-9) (8,9).
Other causes consist of vasculitis and vascular malformations.
- Inflammatory causes: demyelinating lesions in multiple sclerosis (MS) can involve the brainstem causing OP (Fig.
10).
- Neoplastic diseases: including intra- and extra-axial tumors.
Among intrinsic neoplasms,
the most common in adults are metastasis,
with brainstem gliomas and ependymomas more frequent in the pediatric population.
- Traumatic injuries: OP can be caused by shearing axonal injury in the brainstem (Fig.
11) and Duret’s haemorrhage,
as well as contusion to the dorso-lateral aspect of the midbrain against the tentorium following descending transtentorial herniation.
- Infectious diseases: rhomboencephalitis.
The most common etiologic agents are Listeria and Herpes.
- Metabolic diseases: OP can be part of severe brainstem dysfunction in central pontine myelinolysis.
The clinical presentation can be dramatic,
with “locked-in syndrome” (Fig.
7) (10).
Infranuclear OP: the infranuclear compartment refers to the entire course of the nerves,
distal to the nucleus and along their course to the EOMs in the orbits.
It includes different anatomical spaces: the subarachnoid space ventral to the brainstem (cisternal portion of the CNs III,
IV,
VI),
the skull base (for CN VI),
the cavernous sinuses,
and the orbits.
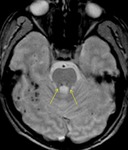
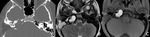
Subarachnoid: lesions in this compartment can result in OP with isolated or multiple CNs palsy.
- Vascular diseases: including micro-ischemia (with negative MR or nerve enhancement) (11),
neurovascular conflict and compression from aneurysm (Fig.
12).
- Traumatic injuries: as a complication of surgery or caused by shearing injury or contusion against the edge of the tentorium after trauma (12).
- Neoplastic diseases: intrinsic diseases (schwannomas or leptomeningeal metastasis) or compression by extrinsic neoplastic masses,
such as meningiomas,
clival chordomas,
dural or skull base metastasis,
brainstem tumors,
sellar tumors,
epidermoids,
or arachnoid cysts (Fig.
13).
- Infectious/inflammatory/degenerative/idiopathic diseases: infectious meningitis with leptomeningeal inflammation; viral neuritis; neurosarcoidosis; chronic idiopathic demyelinating polyneuropathy.
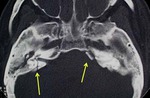
Skull base: the CN VI can be involved by pathological processes of the skull base due to its intraosseous course in Dorello’s canal through the clivus and petrous apex,
and then in the lateral basilar venous sinus.
- Traumatic injuries: skull base fractures can be the cause of traumatic Gradenigo’s syndrome with ipsilateral CNs VI and VII palsy and trigeminal pain.
Thin section CT with bone algorithm data reconstruction is the exam of choice (Fig.
14).
- Infectious diseases: inflammatory-infectious condition involving a pneumatized petrous apex with petrous apicitis and classical Gradenigo’s syndrome (13).
- Vascular diseases: internal carotid artery dissections; lateral and inferior petrous venous sinus thrombosis or increased venous pressure in these structures,
such as in dural fistulas,
can cause CN VI palsy (14).
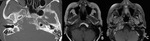
- Neoplastic causes: several neoplastic processes can involve the skull base and present with OP,
inclunding chordoma,
nasopharyngeal carcinoma and chondrosarcoma of the skull base,
metastasis,
plasmocytomas and also benign expansile processes of the petrous apex (epidermoids,
cholesterol granulomas and mucoceles) (Fig.
15-16).
Neuroimaging differential diagnosis basis on the supposed site of origin,
osseous changes (well depicted on unenhanced CT),
and on MR signal characteristics.
Cavernous sinus: pathological processes involving the cavernous sinus can cause cavernous sinus syndrome,
with paresis of some combination of the CNs III,
IV,
VI,
V1 and V2,
peri or retro-orbital pain,
and conjunctival chemosis.
- Vascular causes: carotid-cavernous fistula (Fig.
17),
post-traumatic or consequent to intracavernous aneurysmal rupture; sinus thrombosis (15); cavernous internal carotid artery aneurysms.
- Neoplastic diseases: including extrinsic masses invasion,
for instance due to intrasellar tumors and skull base cancers,
or intrinsic cavernous sinus tumors such as meningioma,
schwannoma and hemangioma.
- Inflammatory and pseudo-tumoral causes: Tolosa-Hunt syndrome (Fig.
18) (16) and sarcoidosis.
Orbit
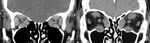
Pathological processes in the orbit can cause OP affecting the distal portion of the nerves or the EOMs.
There is frequent overlap of pathology and clinical picture between cavernous sinus and orbital apex (Fig.
19).
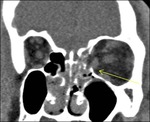
- Trauma: fracture of the orbital apex,
muscle entrapment (Fig.
20),
intra/extra-conal hematoma.
- Tumors: such as lymphoma,
meningioma,
schwannoma.
- EOMs myopathy (Fig.
21).
- Infections.