HEMODYNAMICS OF THE NORMAL VESSELS OF THE LIVER
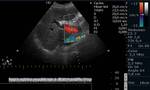
Physiologic portal venous flow should always be antegrade and hepatopetal (toward the transducer and therefore creates a waveform above the baseline).
Flow velocity in this vessel is relatively low (16ã40 cm/sec) compared with the hepatic artery.
The evaluation of the TAVM (Time average velocities,
mean and maximum) will provide a globally more accurate hemodynamic information rather than transient velocities,
and should range from 10 to 18 cm/sec on fasting state (Fig.1).
Normal phasicity may range from low to high.
Abnormally low phasicity results in a nonphasic waveform,
whereas abnormally high phasicity results in a pulsatile waveform.
Portal vein diameter usually range from 6 to 12mm but may slight increase in caliber with deep breathing.
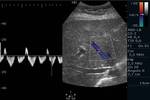
The normal hepatic venous waveform has historically been called triphasic; in reality,
however,
it is biphasic with predominantly antegrade flow (hepatofugal) and four inflection points: there is a complex alternating antegrade-retrograde flow variations,
created by pressure variations related to the cardiac cycle (Fig.2).
The caliber of these vessels should be lesser than 10mm (2cm away from the IVC) and may collapse with deep breathing.
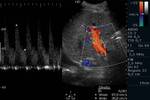
In normal subjects the hepatic artery is a low-resistance vessel (because the liver requires continuous blood flow),
with a pulsatile waveform.
In general,
low-resistance arteries normally have an RI of 0.55ã0.7,
however,
wider normal ranges of 0.55ã0.81 have been reported for this vessel (Fig.3).
Any measured RI above or below the normal range may represent disease (high resistance is less specific for disease than is low resistance).
PORTAL HYPERTENSION
Portal hypertension is a clinical syndrome that develops when the resistance of blood flow within the portal vein system increases and/or portal blood flow increases.
In developed countries it is mainly caused by liver cirrhosis,
in which elevated portal pressure results from a combination of increased portal inflow due to splanchnic arteriolar vasodilation,
and elevated resistance to outflow through distorted hepatic sinusoids.
Actual direct measurement of portal pressures is an invasive technique and obtained only in a small minority of patients.
On the other hand,
Doppler US is an accurate non-invasive method for evaluation of portal hemodynamics,
that provides valuable information on morphological,
qualitative and quantitative changes.