PORTAL HYPERTENSION
A portal vein diameter greater than 13 mm is a possible finding in portal hypertension.
However,
as a diagnostic indicator, it has a sensitivity of 40% or less.
Several physiologic factors including a postprandial increment in splanchnic flow,
respiratory phasic change and gravity together with patient positional change may cause size variation in the portal vein and,
therefore,
make this measurement diagnostically unreliable.
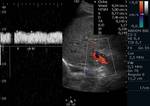
Abnormally slow portal venous flow is diagnostic for portal hypertension when peak velocity is less than 16 cm/sec (Fig.4).
In most cases of portal hypertension the flow is still hepatopetal but spectral analysis may demonstrate loss of respiratory phasicity and more pronounced cardiac periodicity which can progress to an absence of end-diastolic flow,
arterialized flow or bidirectional "to-and-fro" flow.
With increasing hepatic parenchymal scarring and fibrosis,
the pathway of least resistance for the hepatic arterial inflow becomes the portal vein resulting in reversed portal vein flow. A slow or reversed (hepatofugal) flow are two of the most specific findings for portal hypertension.
Absent flow in the portal vein may be due to stagnant flow in portal hypertension.
If the portal vein is only partially blocked (nonocclusive intraluminal filling defects),
there will be some degree of flow,
which may be increased at the stenosis.
Recanalization occurs in some cases of thrombosis but,
more frequently,
if portal vein thrombosis persists,
portal flow is reestablished via cavernous transformation (portal vein undergoes fibrosis and a tangle of tortuous collateral veins are seen along the usual course of the portal vein).
Two main types of alteration of hepatic venous waveform profile can be demonstrated in portal hypertension,
especially in patients with cirrhosis.
The first is regional flow acceleration resulting from focal compression by regenerative nodules.
The second is decreased hepatic venous phasicity (decreased pulsatility) and spectral broadening secondary to non-compliance caused by fibrotic parenchyma (Fig.5).
Narrowing of the hepatic veins can also be seen.
Dilated superior mesenteric vein (SMV) and splenic vein (SV),
which mean a calibre greater than 10mm,
are suggestive of portal hypertension.
In same cases reversed flow (hepatofugal) may be detected (Fig.6).
The effect of chronic hepatocellular disease on hepatic arterial microcirculation is complex and variable.
Arterial resistance has been shown to be decreased,
normal,
or increased in cirrhotic patients.
Some aspects of the disease process,
such as inflammatory edema,
arterial compression by regenerative nodules,
and arterial compression by noncompliant (fibrotic) parenchyma,
have been thought to increase arterial resistance index.
Other aspects,
such as the ãhepatic arterial buffer responseã (compensatory small artery proliferation and increased numbers of arteriolar beds) and arteriovenous shunting,
are thought to decrease resistance.
The overall balance of these factors have shown that hepatic arterial RI is not sufficiently specific or sensitive to allow a diagnosis of cirrhosis or predict its severity.
PORTOSYSTEMIC COLLATERALS
The most specific finding for portal hypertension is the development of portosystemic collaterals,
which form when the resistance to blood flow in the portal vessels exceeds the resistance to flow in the small communicating channels between the portal and systemic circulations.
The more severe the portal hypertension the higher the number of portosystemic pathways.
Portosystemic collaterals which drain into the inferior vena cava bypass the liver,
increasing the risk of encephalopathy.
Portosystemic collaterals which drain into the superior vena cava show higher risk of gastroesophageal bleeding.
On Doppler Ultrasound collateral vessels demonstrate continuous flow similar to that of the PV. The most commonly identified sites of portosystemic venous collaterals are:
- Paraumbilical vein:
Originates from the left portal vein and courses inferiorly along the anterior abdominal wall to connect to superior and inferior epigastric veins around umbilicus.
It runs in the recanalised ligamentum teres of the falciform ligament as a tubular structure measuring more than 3 mm.
Hepatofugal venous flow in the ligamentum teres with a velocity greater than 5 cm/sec is highly specific for the presence of portal hypertension (Fig.7).
- Gastroesophageal or short gastric:
They are best visualized through the left lobe of liver and are formed between the left gastric vein and the short gastric veins (Fig.8).
Normal left gastric vein is up to 6mm in diameter and shows hepatopetal flow whereas in portal hypertension it is enlarged and may show hepatofugal flow.
- Splenorenal and gastrorenal veins:
Tortuous vessels may be seen in the hilar region of spleen and left kidney representing collaterals between splenic,
left gastric and short gastric veins and the systemic left renal or adrenal veins (Fig.9).
Their existence may be inferred by asymmetrical enlargement of the left renal vein.
- Gallbladder:
Gallbladder varices are sometimes observed in portal hypertension patients and reflect shunting of blood from cystic vein to anterior abdominal wall or to patent paraumbilical vein branches in the liver.
On ultrasound they appear as cystic or tubular areas in the GB wall.
- Intestinal:
These collateral pathways occur in areas where the gastrointestinal tract is retroperitoneal (e.g.,
ascending and descending colon and duodenum) and they connect pancreaticoduodenal,
retroperitoneal and omental veins with renal,
phrenic and lumbar veins (Fig.10).
- Haemorrhoids:
Collaterals in the anorectal region connect the inferior mesenteric veins,
via the superior rectal veins,
with the middle and inferior rectal veins of the systemic circulation.
It is difficult to detect rectal/pararectal varices on transabdominal ultrasound but these can be seen using transvaginal scanning.
ASSOCIATED FINDINGS
Splenomegaly,
ascites and pleural effusion are often seen in patients with portal hypertension although these findings are nonspecific and may be seen in other pathologic conditions.